Neurological involvement among non-hospitalized adolescents and young adults 6 months after acute COVID-19
- PMID: 38385031
- PMCID: PMC10879600
- DOI: 10.3389/fneur.2024.1345787
Neurological involvement among non-hospitalized adolescents and young adults 6 months after acute COVID-19
Abstract
Introduction: The post-COVID-19 condition (PCC) is characterized by debilitating persistent symptoms, including symptoms suggesting neurological aberrations such as concentration difficulties, impaired memory, pain, and sleep disturbances. The underlying mechanisms remain elusive. This study aimed to investigate brain injury biomarkers, neurocognitive test performance, and self-reported neurological and neuropsychological symptoms in young people with PCC.
Methods: A total of 404 non-hospitalized adolescents and young adults aged 12-25 years who tested positive for SARS-CoV-2, along with 105 matched SARS-CoV-2 negative individuals, were prospectively enrolled and followed-up for 6 months (Clinical Trials ID: NCT04686734). All participants underwent comprehensive assessment encompassing clinical examinations, questionnaires, neurocognitive testing and blood sampling. Serum samples were immunoassayed for the brain injury biomarkers neurofilament light chain (Nfl) and glial fibrillary acidic protein (GFAp). At 6 months, cross-sectional analyses of serum Nfl/GFAp, neurocognitive test results and symptom scores were performed across groups based on adherence to PCC criteria as well as initial SARS-CoV-2 test results. Also, associations between Nfl/GFAp, neurocognitive test results, and symptom scores were explored.
Results: A total of 381 SARS-CoV-2 positive and 85 SARS-CoV-2 negative were included in the final analysis at 6 months, of whom 48% and 47%, respectively, adhered to the PCC criteria. Serum levels of Nfl and GFAp were almost equal across groups and did not differ from reference values in healthy populations. Also, neurocognitive test results were not different across groups, whereas symptom scores were significantly higher in patients fulfilling PCC criteria (independent of initial SARS-CoV-2 status). No significant associations between Nfl/GFAp, neurocognitive test results, and symptom scores were found.
Conclusion: Normal brain injury biomarkers and neurocognitive performance 6 months after mild COVID-19 implies that the persistent symptoms associated with PCC are not concurrent with ongoing central nervous system damage or permanent disruption of cognitive functions. This finding contradicts the notion of neuroinflammation as a likely explanation for the persistent symptoms.
Keywords: COVID-19; adolescents; cognitive functions; fatigue; glial fibrillary acidic protein; neurofilament; post-COVID-19 condition.
Copyright © 2024 Havdal, Selvakumar, Lund Berven, Stiansen-Sonerud, Zetterberg, Blennow, Holmøy and Wyller.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest. The author(s) declared that they were an editorial board member of Frontiers, at the time of submission. This had no impact on the peer review process and the final decision.
Figures


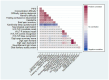
References
-
- Haddad A, Janda A, Renk H, Stich M, Frieh P, Kaier K, et al. . Long COVID symptoms in exposed and infected children, adolescents and their parents one year after SARS-CoV-2 infection: a prospective observational cohort study. EBioMedicine. (2022) 84:104245. doi: 10.1016/j.ebiom.2022.104245, PMID: - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous

