Telehealth Access and Substitution in the VHA
- PMID: 38393611
- PMCID: PMC10937886
- DOI: 10.1007/s11606-023-08465-0
Telehealth Access and Substitution in the VHA
Abstract
Background: In response to COVID-19, the Veterans Health Administration (VHA) expanded telehealth availability, allowing veterans to receive care at home. We explore the extent of substitution of telehealth for in-person care among medical centers (facilities), providers, and patients. We explore the extent to which patient preferences drive telehealth utilization, and compare access to care (as measured by waiting times) for telehealth and in-person visits.
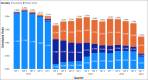
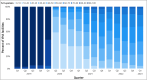
Methods: We use VHA electronic health records to identify scheduled outpatient mental health (MH) appointments from January 2019 through February 2023 focusing on care delivered by social workers, psychologists, and psychiatrists. For each quarter, we compute the proportion of completed appointments that were delivered via phone or video by each facility, provider, and patient and show the changes in these proportions before, during, and after the onset of COVID-19. To explore patient preferences, we match providers of patients with high rates of telehealth utilization and examine the extent to which those providers deliver in-person care. To examine access to care, we compute waiting times for in-person, video, and phone new patient appointments. We investigate differences between urban and rural patients, and patients of different ages.
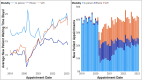
Key results: Telehealth for MH grew dramatically in the VHA after the onset of COVID-19. While some facilities provided more telehealth than others, all facilities (as of early 2023) provided some telehealth MH services. Approximately 86% of individual providers provided telehealth, with 27% scheduling MH appointments almost exclusively as telehealth appointments and 59% providing a mix. Patients exhibited more polarization, with 36% scheduling only in-person visits for almost all their MH visits and 56% of them scheduling exclusively telehealth, and only 8% of them utilizing a mix of modalities. Of those who exclusively received telehealth care, a majority of them utilized video (80%) over phone (20%). Take-up of MH among younger patients was higher relative to older patients. Urban patients used telehealth more than rural patients. Patient preferences rather than provider preferences drove utilization of patients who almost exclusively utilized telehealth. Between April 2021 and February 2023, the average difference in waiting time for in-person and video appointments was less than 1 day, with comparable appointment volumes, suggesting that the supply of and demand for in-person and video were not different enough to merit waiting longer. Telehealth was chosen over in-person more among urban and younger patients, as older and rural patients exhibited higher willingness to wait for in-person over video appointments. By contrast, appointment volumes and waiting times for phone appointments were lower across all groups, suggesting that phone may not be as substitutable for in-person visits in MH.
Conclusions: We find that the VHA has made telehealth widely available, providing access to many veterans. While telehealth utilization has increased, face-to-face care persists for MH services, suggesting that one modality may not serve all purposes and preferences for care. Patient preferences drive the modality decision among those who exclusively use MH care via telehealth. For those who persist in mostly utilizing in-person care, there may be various factors influencing those preferences such as issues with limited internet connectivity, language barriers, and digital literacy, especially for older and rural patients who utilize in-person care more than those who are younger and more urban. Further investigation is required to investigate the optimal mix of modalities which may allow for potential increases in patient satisfaction, quality of care, and clinic efficiency.
© 2024. The Author(s).
Conflict of interest statement
The authors declare that they do not have a conflict of interest.
Figures


Similar articles
-
Evidence Brief: Comparative Effectiveness of Appointment Recall Reminder Procedures for Follow-up Appointments [Internet].Washington (DC): Department of Veterans Affairs (US); 2015 Jul. Washington (DC): Department of Veterans Affairs (US); 2015 Jul. PMID: 27606388 Free Books & Documents. Review.
-
Getting Connected: a Retrospective Cohort Investigation of Video-to-Home Telehealth for Mental Health Care Utilization Among Women Veterans.J Gen Intern Med. 2022 Sep;37(Suppl 3):778-785. doi: 10.1007/s11606-022-07594-2. Epub 2022 Aug 30. J Gen Intern Med. 2022. PMID: 36042096 Free PMC article.
-
Rural patient and provider perceptions of telehealth implemented during the COVID-19 pandemic.BMC Health Serv Res. 2023 Sep 12;23(1):981. doi: 10.1186/s12913-023-09994-4. BMC Health Serv Res. 2023. PMID: 37700286 Free PMC article.
-
Patient and provider predictors of telemental health use prior to and during the COVID-19 pandemic within the Department of Veterans Affairs.Am Psychol. 2022 Feb-Mar;77(2):249-261. doi: 10.1037/amp0000895. Epub 2021 Dec 23. Am Psychol. 2022. PMID: 34941310 Free PMC article.
-
Telemedicine and Its Perceptions in a Border Community: A Review of How Health Care Technology Has Helped Increase Access.Telemed J E Health. 2024 Apr;30(4):987-993. doi: 10.1089/tmj.2023.0179. Epub 2023 Nov 17. Telemed J E Health. 2024. PMID: 37976130 Review.
Cited by
-
Evaluating spoke facilitation costs of implementing TelePain in the Veterans Health Administration.Implement Sci Commun. 2025 May 1;6(1):51. doi: 10.1186/s43058-025-00729-6. Implement Sci Commun. 2025. PMID: 40312743 Free PMC article.
-
Mental Health Treatment among U.S. Military Veterans: Insights from the National Health Interview Survey.J Gen Intern Med. 2025 Jan 3. doi: 10.1007/s11606-024-09320-6. Online ahead of print. J Gen Intern Med. 2025. PMID: 39753811
References
-
- Ferguson JM, Jacobs J, Yefimova M, Greene L, Heyworth L, Zulman DM. Virtual care expansion in the Veterans Health Administration during the COVID-19 pandemic: clinical services and patient characteristics associated with utilization. J Am Med Inform Assoc. 2021;28(3):453–462. doi: 10.1093/jamia/ocaa284. - DOI - PMC - PubMed
-
- Darkins A, Ryan P, Kobb R, Foster L, Edmonson E, Wakefield B, Lancaster AE. Care coordination/home telehealth: the systematic implementation of health informatics, home telehealth, and disease management to support the care of veteran patients with chronic conditions. Telemed e_Health. 2008;14(10):1118–1126. doi: 10.1089/tmj.2008.0021. - DOI - PubMed
-
- Sadej I, Lum J, Pearson E, Pizer SD. “Virtual Health Care: Using Telehealth to Provide Care in VHA.” Partnered Evidence-based Policy Resource Center Brief, August 2021.
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

