Cardiopulmonary Exercise Performance of Children Born Non-Extremely Preterm
- PMID: 38397309
- PMCID: PMC10887626
- DOI: 10.3390/children11020198
Cardiopulmonary Exercise Performance of Children Born Non-Extremely Preterm
Abstract
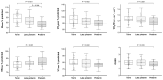
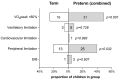
Data on exercise tolerance of children born non-extremely preterm are sparse. We aimed to explore the cardiopulmonary exercise testing (CPET) characteristics in this population. We studied 63 children (age 7-12 years) born at 290/7-366/7 weeks of gestation (34 were late preterm, 29 were preterm) and 63 age-matched, term-born controls. All performed spirometry and CPET (cycle ergometry). There were no differences in activity levels and spirometric parameters between the group of preterm-born children and controls. A peak oxygen uptake (VO2peak) of <80% was noted in 25.4% of the term-born and 49.2% of preterm-born children (p = 0.001). Term-born participants presented similar VO2peak to late-preterm children but higher than those born at <340/7 weeks of gestation (p = 0.002). Ventilatory limitation was noted in 4.8% of term and 7.9% of preterm participants, while only one preterm child presented cardiovascular limitation. Children born before 34 weeks of gestation had higher respiratory rates and smaller tidal volumes at maximum exercise, as well as lower oxygen uptake for the level of generated work. We conclude that school-age children born at 29-34 weeks of gestation may present decreased exercise performance attributed to an altered ventilatory response to exercise and impaired O2 utilization by their skeletal muscles rather than other cardiopulmonary limiting factors.
Keywords: cardiopulmonary exercise testing; children; exercise performance; exercise tolerance; prematurity; preterm children.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
Similar articles
-
Impact of premature birth on cardiopulmonary function in later life.Eur J Pediatr. 2023 Jul;182(7):3265-3274. doi: 10.1007/s00431-023-04952-y. Epub 2023 May 6. Eur J Pediatr. 2023. PMID: 37147470 Free PMC article.
-
Altered breathing mechanics and ventilatory response during exercise in children born extremely preterm.Thorax. 2016 Nov;71(11):1012-1019. doi: 10.1136/thoraxjnl-2015-207736. Epub 2016 Jun 3. Thorax. 2016. PMID: 27259338 Free PMC article.
-
Lung abnormalities do not influence aerobic capacity in school children born preterm.Eur J Appl Physiol. 2021 Feb;121(2):489-498. doi: 10.1007/s00421-020-04530-2. Epub 2020 Nov 3. Eur J Appl Physiol. 2021. PMID: 33141263
-
Respiratory and cardiopulmonary limitations to aerobic exercise capacity in adults born preterm.J Appl Physiol (1985). 2020 Oct 1;129(4):718-724. doi: 10.1152/japplphysiol.00419.2020. Epub 2020 Aug 13. J Appl Physiol (1985). 2020. PMID: 32790592 Free PMC article. Review.
-
Preterm birth and exercise capacity: what do we currently know?Front Pediatr. 2023 Oct 6;11:1222731. doi: 10.3389/fped.2023.1222731. eCollection 2023. Front Pediatr. 2023. PMID: 37868270 Free PMC article. Review.
Cited by
-
Physiological responses to exercise in survivors of preterm birth: a meta-analysis.Eur Respir Rev. 2025 Jun 18;34(176):240163. doi: 10.1183/16000617.0163-2024. Print 2025 Apr. Eur Respir Rev. 2025. PMID: 40533101 Free PMC article.
References
Grants and funding
LinkOut - more resources
Full Text Sources

