Continuous Interscalene Brachial Plexus Blocks: An Anatomical Challenge between Scylla and Charybdis?
- PMID: 38399521
- PMCID: PMC10890524
- DOI: 10.3390/medicina60020233
Continuous Interscalene Brachial Plexus Blocks: An Anatomical Challenge between Scylla and Charybdis?
Abstract
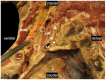
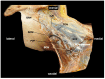
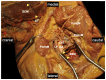
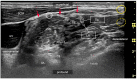
Brachial plexus blocks at the interscalene level are frequently chosen by physicians and recommended by textbooks for providing regional anesthesia and analgesia to patients scheduled for shoulder surgery. Published data concerning interscalene single-injection or continuous brachial plexus blocks report good analgesic effects. The principle of interscalene catheters is to extend analgesia beyond the duration of the local anesthetic's effect through continuous infusion, as opposed to a single injection. However, in addition to the recognized beneficial effects of interscalene blocks, whether administered as a single injection or through a catheter, there have been reports of consequences ranging from minor side effects to severe, life-threatening complications. Both can be simply explained by direct mispuncture, as well as undesired local anesthetic spread or misplaced catheters. In particular, catheters pose a high risk when advanced or placed uncontrollably, a fact confirmed by reports of fatal outcomes. Secondary catheter dislocations explain side effects or loss of effectiveness that may occur hours or days after the initial correct function has been observed. From an anatomical and physiological perspective, this appears logical: the catheter tip must be placed near the plexus in an anatomically tight and confined space. Thus, the catheter's position may be altered with the movement of the neck or shoulder, e.g., during physiotherapy. The safe use of interscalene catheters is therefore a balance between high analgesia quality and the control of side effects and complications, much like the passage between Scylla and Charybdis. We are convinced that the anatomical basis crucial for the brachial plexus block procedure at the interscalene level is not sufficiently depicted in the common regional anesthesia literature or textbooks. We would like to provide a comprehensive anatomical survey of the lateral neck, with special attention paid to the safe placement of interscalene catheters.
Keywords: catheter malposition; interscalene brachial plexus block; interscalene catheter; scalenovertebral triangle; shoulder surgery; ultrasound.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
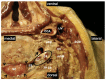
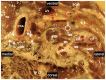
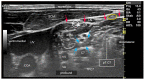
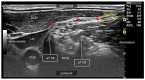
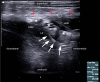
References
-
- Stundner O., Meissnitzer M., Brummett C.M., Moser S., Forstner R., Koköfer A., Danninger T., Gerner P., Kirchmair L., Fritsch G. Comparison of tissue distribution, phrenic nerve involvement, and epidural spread in standard- vs. low-volume ultrasound-guided interscalene plexus block using contrast magnetic resonance imaging: A randomized, controlled trial. Br. J. Anaesth. 2016;116:405–412. doi: 10.1093/bja/aev550. - DOI - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources

