Analgesic efficacy of surgeon placed paravertebral catheters compared with thoracic epidural analgesia after Ivor Lewis esophagectomy: a retrospective non-inferiority study
- PMID: 38410611
- PMCID: PMC10894387
- DOI: 10.21037/jtd-23-689
Analgesic efficacy of surgeon placed paravertebral catheters compared with thoracic epidural analgesia after Ivor Lewis esophagectomy: a retrospective non-inferiority study
Abstract
Background: The Ivor Lewis esophagectomy is an operation that involves a laparotomy and a right thoracotomy, both of which are associated with severe postoperative pain and subsequent impairment of respiratory function. Currently, the accepted "gold standard" for postoperative analgesia for laparotomies and thoracotomies is the thoracic epidural. A systematic review has shown paravertebral blocks to be equivalent to epidural analgesia for post-thoracotomy pain control and have decreased incidence of nausea and vomiting, hypotension and respiratory depression. To our knowledge, the use of the paravertebral catheter (PVC) in open Ivor Lewis esophagectomy has not been formally studied. The primary outcome is the area under the curve (AUC) pain scores in the first 48 hours after surgery.
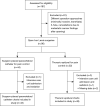
Methods: We performed a retrospective chart review of the open Ivor Lewis esophagectomy patients at our local institution, with local research ethics board (REB) approval.
Results: A total of 92 patients were included in this study: 43 patients had a PVC and 49 had a thoracic epidural for postoperative pan control. Overall, the PVC group was non-inferior and statistically equivalent to the epidural group. Time to ambulation in the PVC group was non-inferior compared to epidurals. The PVC group was superior when comparing total opioid consumption.
Conclusions: Our retrospective study continues to challenge the role of epidurals as the gold standard of pain control post thoracotomy and laparotomy. Further prospective studies with a larger population are needed to better compare the two modalities.
Keywords: Esophagectomy; pain management; paravertebral; thoracotomy.
2024 Journal of Thoracic Disease. All rights reserved.
Conflict of interest statement
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at https://jtd.amegroups.com/article/view/10.21037/jtd-23-689/coif). D.F. reports consulting fees from AstraZeneca. The other authors have no conflicts of interest to declare.
Figures

Similar articles
-
Continuous paravertebral extrapleural infusion for post-thoracotomy pain management.Surgery. 1999 Oct;126(4):650-6; discussion 656-7. Surgery. 1999. PMID: 10520911 Clinical Trial.
-
Multimodal analgesia using intrathecal diamorphine, and paravertebral and rectus sheath catheters are as effective as thoracic epidural for analgesia post-open two-phase esophagectomy within an enhanced recovery program.Dis Esophagus. 2018 Jun 1;31(6). doi: 10.1093/dote/doy006. Dis Esophagus. 2018. PMID: 29800270
-
Dual-epidural catheter technique and perioperative outcomes after Ivor-Lewis esophagectomy.Reg Anesth Pain Med. 2013 Jan-Feb;38(1):3-8. doi: 10.1097/AAP.0b013e318276a714. Reg Anesth Pain Med. 2013. PMID: 23222360
-
Intra-operative paravertebral block for postoperative analgesia in thoracotomy patients: a randomized, double-blind, placebo-controlled study.Eur J Cardiothorac Surg. 2011 Oct;40(4):902-6. doi: 10.1016/j.ejcts.2011.01.067. Epub 2011 Mar 5. Eur J Cardiothorac Surg. 2011. PMID: 21377888 Review.
-
Update on the role of paravertebral blocks for thoracic surgery: are they worth it?Curr Opin Anaesthesiol. 2009 Feb;22(1):38-43. doi: 10.1097/ACO.0b013e32831a4074. Curr Opin Anaesthesiol. 2009. PMID: 19237975 Review.
References
-
- Reed CE. Technique of Open Ivor Lewis Esophagectomy. Oper Tech Thorac Cardiovasc Surg 2009;14:160-75.
-
- Davies RG, Myles PS, Graham JM. A comparison of the analgesic efficacy and side-effects of paravertebral vs epidural blockade for thoracotomy--a systematic review and meta-analysis of randomized trials. Br J Anaesth 2006;96:418-26. Erratum in: Br J Anaesth 2007;99:768.10.1093/bja/ael020 - DOI - PubMed
-
- Howells P, Bieker M, Yeung J. Oesophageal cancer and the anaesthetist. BJA Educ 2017;17:68-73.
LinkOut - more resources
Full Text Sources
