Tritesting in Battor, Ghana: an integrated cervical precancer screening strategy to mitigate the challenges of multiple screening visits and loss to follow-up
- PMID: 38414966
- PMCID: PMC10898900
- DOI: 10.3332/ecancer.2023.1645
Tritesting in Battor, Ghana: an integrated cervical precancer screening strategy to mitigate the challenges of multiple screening visits and loss to follow-up
Abstract
Background: Human papillomavirus (HPV) DNA testing is more sensitive than cytology for detecting cervical precancer; however, increasing reports of high-risk HPV (hr-HPV)-negative cases of cervical intraepithelial neoplasia (CIN) and even malignancy motivate the use of combined testing. We present our experience with 'tritesting', defined as the performance of HPV DNA testing, cytology and visual inspection in a single session at the Cervical Cancer Prevention and Training Centre, Ghana. We further determined the prevalence rates of hr-HPV infection, abnormal cytology and cervical lesions among women screened using tritesting.
Methods: This descriptive retrospective cross-sectional study assessed all women screened via tritesting between April 2019 to April 2023. HPV DNA testing was performed using the Sansure MA-6000, GeneXpert or AmpFire platforms. Visual inspection was performed using enhanced visual assessment mobile colposcopy or visual inspection with acetic acid. Liquid-based cytology was performed using cervical samples taken with a Cervex-Brush® and fixed in PreservCyt, while samples for conventional cytology were taken using an Ayre spatula and cytobrush.
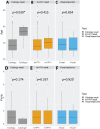
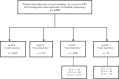
Results: Among 236 women screened (mean age, 39.1 years (standard deviation, 10.9)), the overall prevalence rates of hr-HPV infection and cervical lesions were 17.8% (95% confidence interval (CI), 13.1-23.3) and 11.9% (95% CI, 8.0-16.7), respectively. Cytology yielded findings of atypical squamous cells of undetermined significance or worse in 2.5% (95% CI, 0.9-5.5) of women. Histopathology following loop electrosurgical excision procedure revealed CIN I (tritest positive) and CIN III (hr-HPV-positive, visual inspection 'positive', cytology-negative) in one woman each. Factors independently associated with hr-HPV infection among 'tritested' women were age ≥ 39 years, tertiary level of education and current contraceptive use. Twenty-seven out of 39 hr-HPV-positive women (69.2%; 95% CI, 52.4-83.0) showed a type 3 transformation zone and would have needed to be recalled for a cytologic sample to be taken in a 'see and triage' approach with HPV DNA testing and a visual inspection method.
Conclusion: This study brings tritesting into the spotlight, as an alternative to other methods, particularly for women who prefer this due to the advantage of a single visit to a health facility and being more cost-effective, if they have to travel long distances to access cervical screening services.
Keywords: Papanicolaou test; colposcopy; cytology; human papillomavirus DNA test; human papillomavirus infection; uterine cervical neoplasm.
© the authors; licensee ecancermedicalscience.
Conflict of interest statement
The authors declare that they have no conflict of interest.
Figures
Similar articles
-
HPV DNA Testing and Mobile Colposcopy for Cervical Precancer Screening in HIV Positive Women: A Comparison Between Two Settings in Ghana and Recommendation for Screening.Cancer Control. 2024 Jan-Dec;31:10732748241244678. doi: 10.1177/10732748241244678. Cancer Control. 2024. PMID: 38563112 Free PMC article.
-
Concurrent HPV DNA testing and a visual inspection method for cervical precancer screening: A practical approach from Battor, Ghana.PLOS Glob Public Health. 2023 Apr 20;3(4):e0001830. doi: 10.1371/journal.pgph.0001830. eCollection 2023. PLOS Glob Public Health. 2023. PMID: 37079498 Free PMC article.
-
Nationwide cervical precancer screening in Ghana: concurrent HPV DNA testing and visual inspection under an expanded hub-and-spoke model.Sci Rep. 2025 Jan 11;15(1):1744. doi: 10.1038/s41598-024-81274-5. Sci Rep. 2025. PMID: 39799219 Free PMC article.
-
Overview of human papillomavirus-based and other novel options for cervical cancer screening in developed and developing countries.Vaccine. 2008 Aug 19;26 Suppl 10:K29-41. doi: 10.1016/j.vaccine.2008.06.019. Vaccine. 2008. PMID: 18847555 Review.
-
Evidence regarding human papillomavirus testing in secondary prevention of cervical cancer.Vaccine. 2012 Nov 20;30 Suppl 5:F88-99. doi: 10.1016/j.vaccine.2012.06.095. Vaccine. 2012. PMID: 23199969 Review.
Cited by
-
Expanding management strategies for cervical precancerous lesions in resource-limited settings: insights from a training center in a district hospital in Ghana.BMC Womens Health. 2024 Jul 27;24(1):428. doi: 10.1186/s12905-024-03263-0. BMC Womens Health. 2024. PMID: 39060995 Free PMC article.
-
Cross-sectional evaluation of a peer educator-led empowerment initiative for improving participation in cervical precancer screening among female sex workers in Ghana.Ecancermedicalscience. 2025 Mar 11;19:1869. doi: 10.3332/ecancer.2025.1869. eCollection 2025. Ecancermedicalscience. 2025. PMID: 40492225 Free PMC article.
-
Rural-urban disparities in cervical cancer screening uptake and its predictors among women aged 30-49 years in Ghana: a multivariate decomposition analysis.BMC Womens Health. 2025 Aug 19;25(1):396. doi: 10.1186/s12905-025-03962-2. BMC Womens Health. 2025. PMID: 40830789 Free PMC article.
References
LinkOut - more resources
Full Text Sources
Miscellaneous
