Growth Patterns of Prostate Cancers Undetected by Prostate 3T Multiparametric MRI
- PMID: 38418107
- PMCID: PMC10905436
- DOI: 10.21873/invivo.13508
Growth Patterns of Prostate Cancers Undetected by Prostate 3T Multiparametric MRI
Abstract
Background/aim: The multiparametric magnetic resonance imaging (mpMRI)-ultrasound (US) fusion targeted biopsy (TB) is a useful diagnostic device for men with suspected prostate cancer (PC) and can increase the detection rate for clinically significant PCs (csPC). However, few studies have shown pathological findings of undetectable csPCs on the prostate mpMRI.
Patients and methods: This study investigated the growth patterns of csPC undetected in prostate mpMRI. The study enrolled 248 patients with suspected PCs and ≥PI-RADS 2 lesions, who then underwent mpMRI-US fusion TB and nearly prostate-mapping systematic biopsies (SB). A total 248 biopsies included 404 regions of interest in TB and 2976 mapping-regions in SB.
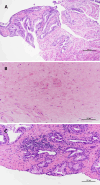
Results: The detection rates of csPC, defined as PC grade group (GG) ≥2, were 42% in TB and 44% in SB, and the highest detection rate was 50%, using both TB and SB. Approximately 79% of PI-RADS 3/4/5 with any PC showed csPC. A total 201 PI-RADS 3/4/5 lesions showed benign prostatic hyperplasia, lymphocytic prostatitis, or fibromuscular stroma only in the core tissues. Notably, 22 csPCs detected in SB but undetected in prostate mpMRI preferentially showed a pattern of mixed well-formed and fused PC glands. The other patterns including cribriform glands and poorly formed glands with intracytoplasmic vacuoles were also seen. Approximately 85% of the 22 csPCs showed tumor volume less than 50% of core tissues.
Conclusion: Changes in prostatic stroma amounts, inflammation severity, tumor volume and growth patterns of PC glands affected the detectability of prostate mpMRI.
Keywords: Multiparametric MRI; biopsy; fusion; pathology; ultrasound.
Copyright © 2024, International Institute of Anticancer Research (Dr. George J. Delinasios), All rights reserved.
Conflict of interest statement
The Authors declare no conflicts of interest.
Figures

Similar articles
-
Targeted multiparametric magnetic resonance imaging/transrectal ultrasound-guided (mpMRI/TRUS) fusion prostate biopsy versus systematic random prostate biopsy: A comparative real-life study.Cancer Rep (Hoboken). 2024 Feb;7(2):e1962. doi: 10.1002/cnr2.1962. Epub 2024 Jan 12. Cancer Rep (Hoboken). 2024. PMID: 38217298 Free PMC article.
-
Effectiveness of Magnetic Resonance Imaging/Ultrasound-guided Target Biopsy in Detecting Clinically Significant Prostate Cancer.Anticancer Res. 2024 Feb;44(2):679-686. doi: 10.21873/anticanres.16858. Anticancer Res. 2024. PMID: 38307559
-
Detection of Clinically Significant Prostate Cancer Using Targeted Biopsy with Four Cores Versus Target Saturation Biopsy with Nine Cores in Transperineal Prostate Fusion Biopsy: A Prospective Randomized Trial.Eur Urol Oncol. 2023 Feb;6(1):49-55. doi: 10.1016/j.euo.2022.08.005. Epub 2022 Sep 26. Eur Urol Oncol. 2023. PMID: 36175281 Clinical Trial.
-
Use of multiparametric magnetic resonance imaging (mpMRI) in active surveillance for low-risk prostate cancer: a scoping review on the benefits and harm of mpMRI in different biopsy scenarios.Prostate Cancer Prostatic Dis. 2021 Sep;24(3):662-673. doi: 10.1038/s41391-021-00320-9. Epub 2021 Mar 2. Prostate Cancer Prostatic Dis. 2021. PMID: 33654249
-
Prostate MRI and image Quality: It is time to take stock.Eur J Radiol. 2023 Apr;161:110757. doi: 10.1016/j.ejrad.2023.110757. Epub 2023 Feb 25. Eur J Radiol. 2023. PMID: 36870241 Free PMC article. Review.
References
-
- Cooperberg MR, Pasta DJ, Elkin EP, Litwin MS, Latini DM, Du Chane J, Carroll PR. The University of California, San Francisco cancer of the prostate risk assessment score: A straightforward and reliable preoperative predictor of disease recurrence after radical prostatectomy. J Urol. 2005;173(6):1938–1942. doi: 10.1097/01.ju.0000158155.33890.e7. - DOI - PMC - PubMed
-
- Hassan O, Han M, Zhou A, Paulk A, Sun Y, Al-Harbi A, Alrajjal A, Baptista Dos Santos F, Epstein JI. Incidence of extraprostatic extension at radical prostatectomy with pure Gleason score 3+ 3=6 (grade group 1) cancer: Implications for whether Gleason score 6 prostate cancer should be renamed “not cancer” and for selection criteria for active surveillance. J Urol. 2018;199(6):1482–1487. doi: 10.1016/j.juro.2017.11.067. - DOI - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous
