Anatomic Reduction of Greater Tuberosity Fragment for Shoulder Hemiarthroplasty: a Predictor of Good Clinical Outcome
- PMID: 38420517
- PMCID: PMC10898802
- DOI: 10.22038/ABJS.2023.74441.3448
Anatomic Reduction of Greater Tuberosity Fragment for Shoulder Hemiarthroplasty: a Predictor of Good Clinical Outcome
Abstract
Objectives: Proximal humerus fractures account for four-five % of all fractures. Shoulder hemiarthroplasty is indicated for complex fractures with high complication rates when treated with ORIF. This study aims to evaluate the correlation between the proper intraoperative tuberosity reduction, and the mid-to-long-term clinical outcome in a series of patients treated with hemiarthroplasty after proximal humerus fracture.
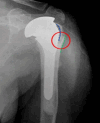
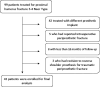
Methods: Forty-one patients with proximal humerus fractures who underwent hemiarthroplasty surgery between July 2009 and December 2019 were retrospectively reviewed. Quantitative analysis of the reduction of the tuberosities was performed on postoperative X-rays focusing on the distance between reconstructed greater tuberosity and the apex of the head of the prosthesis, (head-tuberosity distance), and contact between tuberosity and humerus diaphysis. The University of California Los Angeles Score (UCLA) was calculated for each patient.
Results: The mean time to surgery was 6.29 ± 2.8 days (range 2-18 days). Nine patients out of 41 (22%) had non anatomic tuberosity, and 32 (78%) were anatomic reduced. The UCLA score at the final follow-up was good and excellent (≥27) in 27 patients (66%), and poor (<27) in 14 (34%). A significant correlation was observed between proper tuberosity reduction and good/excellent UCLA scores (P<0.001).
Conclusion: Hemiarthroplasty is a valid and reliable technique for the treatment of proximal humerus fracture not eligible for internal fixation, with high risk of failure. The proper tuberosity reconstruction, paying special attention to the HTD and the contact between the cortical of the humeral diaphysis and the reconstructed tuberosity, is essential to reach a good clinical outcome.
Keywords: Clinical outcome; Hemiarthroplasty; Proximal humerus fractures; Shoulder; Tuberosities reduction.
2024 © BY THE ARCHIVES OF BONE AND JOINT SURGERY.
Conflict of interest statement
None
Figures

References
-
- Court-Brown CM, Caesar B. Epidemiology of adult fractures: A review. Injury. 2006;37(8):691–697. - PubMed
-
- Roux A, Decroocq L, El Batti S, et al. Epidemiology of proximal humerus fractures managed in a trauma center. Orthop Traumatol Surg Res. 2012;98(6):715–719. - PubMed
-
- Court-Brown CM, Garg A, McQueen MM. The epidemiology of proximal humeral fractures. Acta Orthop Scand. 2001;72(4):365–371. - PubMed
-
- Kannus P, Palvanen M, Niemi S, Parkkari J, Järvinen M, Vuori I. Osteoporotic fractures of the proximal humerus in elderly Finnish persons: sharp increase in 1970-1998 and alarming projections for the new millennium. Acta Orthop Scand. 2000;71(5):465–470. - PubMed
-
- Richard GJ, Denard PJ, Kaar SG, et al. Outcome measures reported for the management of proximal humeral fractures: a systematic review. J Shoulder Elb Surg. 2020;29(10):2175–2184. - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous
