Prospective Evaluation of Automated Contouring for CT-Based Brachytherapy for Gynecologic Malignancies
- PMID: 38435965
- PMCID: PMC10906166
- DOI: 10.1016/j.adro.2023.101417
Prospective Evaluation of Automated Contouring for CT-Based Brachytherapy for Gynecologic Malignancies
Abstract
Purpose: The use of deep learning to auto-contour organs at risk (OARs) in gynecologic radiation treatment is well established. Yet, there is limited data investigating the prospective use of auto-contouring in clinical practice. In this study, we assess the accuracy and efficiency of auto-contouring OARs for computed tomography-based brachytherapy treatment planning of gynecologic malignancies.
Methods and materials: An inhouse contouring tool automatically delineated 5 OARs in gynecologic radiation treatment planning: the bladder, small bowel, sigmoid, rectum, and urethra. Accuracy of each auto-contour was evaluated using a 5-point Likert scale: a score of 5 indicated the contour could be used without edits, while a score of 1 indicated the contour was unusable. During scoring, automated contours were edited and subsequently used for treatment planning. Dice similarity coefficient, mean surface distance, 95% Hausdorff distance, Hausdorff distance, and dosimetric changes between original and edited contours were calculated. Contour approval time and total planning time of a prospective auto-contoured (AC) cohort were compared with times from a retrospective manually contoured (MC) cohort.
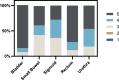
Results: Thirty AC cases from January 2022 to July 2022 and 31 MC cases from July 2021 to January 2022 were included. The mean (±SD) Likert score for each OAR was the following: bladder 4.77 (±0.58), small bowel 3.96 (±0.91), sigmoid colon 3.92 (±0.81), rectum 4.6 (±0.71), and urethra 4.27 (±0.78). No ACs required major edits. All OARs had a mean Dice similarity coefficient > 0.86, mean surface distance < 0.48 mm, 95% Hausdorff distance < 3.2 mm, and Hausdorff distance < 10.32 mm between original and edited contours. There was no significant difference in dose-volume histogram metrics (D2.0 cc/D0.1 cc) between original and edited contours (P values > .05). The average time to plan approval in the AC cohort was 19% less than the MC cohort. (AC vs MC, 117.0 + 18.0 minutes vs 144.9 ± 64.5 minutes, P = .045).
Conclusions: Automated contouring is useful and accurate in clinical practice. Auto-contouring OARs streamlines radiation treatment workflows and decreases time required to design and approve gynecologic brachytherapy plans.
© 2024 The Authors.
Conflict of interest statement
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Figures

References
-
- Bauer-Nilsen K, Hill C, Trifiletti DM, et al. Evaluation of delivery costs for external beam radiation therapy and brachytherapy for locally advanced cervical cancer using time-driven activity-based costing. Int J Radiat Oncol Biol Phys. 2018;100:88–94. - PubMed
-
- Ning MS, Klopp AH, Jhingran A, et al. Quantifying institutional resource utilization of adjuvant brachytherapy and intensity-modulated radiation therapy for endometrial cancer via time-driven activity-based costing. Brachytherapy. 2019;18:445–452. - PubMed
-
- Mulherkar R, Keller A, Showalter TN, Thaker N, Beriwal S. A primer on time-driven activity-based costing in brachytherapy. Brachytherapy. 2022;21:43–48. - PubMed
-
- Cardenas CE, Yang J, Anderson BM, Court LE, Brock KB. Advances in Auto-Segmentation. Semin Radiat Oncol. 2019;29:185–197. - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources

