Classes and predictors of reversal in male patients with congenital hypogonadotropic hypogonadism: a cross-sectional study of six international referral centres
- PMID: 38437850
- PMCID: PMC10996025
- DOI: 10.1016/S2213-8587(24)00028-7
Classes and predictors of reversal in male patients with congenital hypogonadotropic hypogonadism: a cross-sectional study of six international referral centres
Abstract
Background: Although some male patients with congenital hypogonadotropic hypogonadism (CHH) undergo spontaneous reversal following treatment, predictors of reversal remain elusive. We aimed to assemble the largest cohort of male patients with CHH reversal to date and identify distinct classes of reversal.
Methods: This multicentre cross-sectional study was conducted in six international CHH referral centres in Brazil, Finland, France, Italy, the UK, and the USA. Adult men with CHH (ie, absent or incomplete spontaneous puberty by age 18 years, low serum testosterone concentrations, and no identifiable cause of hypothalamic-pituitary-gonadal [HPG] axis dysfunction) were eligible for inclusion. CHH reversal was defined as spontaneous recovery of HPG axis function off treatment. Centres provided common data elements on patient phenotype, clinical assessment, and genetics using a structured, harmonised data collection form developed by COST Action BM1105. Latent class mixture modelling (LCMM) was applied to establish whether at least two distinct classes of reversal could be identified and differentially predicted, and results were compared with a cohort of patients without CHH reversal to identify potential predictors of reversal. The primary outcome was the presence of at least two distinct classes of reversal.
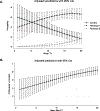
Findings: A total of 87 male patients with CHH reversal and 108 without CHH reversal were included in the analyses. LCMM identified two distinct reversal classes (75 [86%] in class 1 and 12 [14%] in class 2) on the basis of mean testicular volume, micropenis, and serum follicle-stimulating hormone (FSH) concentration. Classification probabilities were robust (0·998 for class 1 and 0·838 for class 2) and modelling uncertainty was low (entropy 0·90). Compared with class 1, patients in class 2 had significantly larger testicular volume (p<0·0001), no micropenis, and higher serum FSH concentrations (p=0·041), consistent with the Pasqualini syndrome (fertile eunuch) subtype of CHH. Patients without CHH reversal were more likely to have anosmia (p=0·016), cryptorchidism (p=0·0012), complete absence of puberty (testicular volume <4 cm³; p=0·0016), and two or more rare genetic variants (ie, oligogenicity; p=0·0001). Among patients who underwent genetic testing, no patients (of 75) with CHH reversal had a rare pathogenic ANOS1 variant compared with ten (11%) of 95 patients without CHH reversal. Individuals with CHH reversal had a significantly higher rate of rare variants in GNRHR than did those without reversal (nine [12%] of 75 vs three [3%] of 95; p=0·025).
Interpretation: Applying LCMM to a large cohort of male patients with CHH reversal uncovered two distinct classes of reversal. Genetic investigation combined with careful clinical phenotyping could help surveillance of reversal after withdrawing treatment, representing the first tailored management approach for male patients with this rare endocrine disorder.
Funding: National Institutes of Health National Center for Advancing Translational Sciences; Ministry of Health, Rome, Italy; Ministry of University, Rome, Italy; National Institutes of Health Eunice Kennedy Shriver National Institute of Child Health and Human Development; and the Josiah Macy Jr Foundation.
Translation: For the Italian translation of the abstract see Supplementary Materials section.
Copyright © 2024 Elsevier Ltd. All rights reserved.
Conflict of interest statement
Declaration of interests We declare no competing interests.
Figures
Comment in
-
Reversibility of congenital hypogonadotropic hypogonadism: lessons from a rare disease.Lancet Diabetes Endocrinol. 2024 Apr;12(4):219-221. doi: 10.1016/S2213-8587(24)00065-2. Epub 2024 Mar 1. Lancet Diabetes Endocrinol. 2024. PMID: 38437851 No abstract available.
Similar articles
-
Clinical presentation of congenital hypogonadotropic hypogonadism in males with delayed puberty according to genetic etiology: a systematic review and meta-analysis after reclassification of gene variants.Hum Reprod. 2025 May 1;40(5):904-918. doi: 10.1093/humrep/deaf041. Hum Reprod. 2025. PMID: 40101754
-
ANOS1 variants in a large cohort of Chinese patients with congenital hypogonadotropic hypogonadism.Zhong Nan Da Xue Xue Bao Yi Xue Ban. 2022 Jul 28;47(7):847-857. doi: 10.11817/j.issn.1672-7347.2022.220071. Zhong Nan Da Xue Xue Bao Yi Xue Ban. 2022. PMID: 36039580 Free PMC article.
-
GNRHR-related central hypogonadism with spontaneous recovery - case report.Ital J Pediatr. 2022 Nov 12;48(1):184. doi: 10.1186/s13052-022-01377-5. Ital J Pediatr. 2022. PMID: 36371229 Free PMC article.
-
Correlation Analysis of Genotypes and Phenotypes in Chinese Male Pediatric Patients With Congenital Hypogonadotropic Hypogonadism.Front Endocrinol (Lausanne). 2022 May 20;13:846801. doi: 10.3389/fendo.2022.846801. eCollection 2022. Front Endocrinol (Lausanne). 2022. PMID: 35669683 Free PMC article.
-
Congenital hypogonadotropic hypogonadism and Kallmann syndrome as models for studying hormonal regulation of human testicular endocrine functions.Ann Endocrinol (Paris). 2014 May;75(2):79-87. doi: 10.1016/j.ando.2014.04.011. Epub 2014 May 9. Ann Endocrinol (Paris). 2014. PMID: 24815726 Review.
Cited by
-
Spontaneous Improvement of Hypogonadotropic Hypogonadism in a Patient with PCSK1 and HS6ST1 Mutations: A Case Report.Life (Basel). 2025 Jul 21;15(7):1151. doi: 10.3390/life15071151. Life (Basel). 2025. PMID: 40724652 Free PMC article.
-
Kallmann Syndrome: Functional Analysis of a CHD7 Missense Variant Shows Aberrant RNA Splicing.Int J Mol Sci. 2024 Nov 10;25(22):12061. doi: 10.3390/ijms252212061. Int J Mol Sci. 2024. PMID: 39596130 Free PMC article.
-
Current landscape of fertility induction in males with congenital hypogonadotropic hypogonadism.Ann N Y Acad Sci. 2024 Oct;1540(1):133-146. doi: 10.1111/nyas.15214. Epub 2024 Aug 27. Ann N Y Acad Sci. 2024. PMID: 39190467 Review.
References
-
- Boehm U, Bouloux PM, Dattani MT, de Roux N, Dode C, Dunkel L, et al. Expert consensus document: European Consensus Statement on congenital hypogonadotropic hypogonadism--pathogenesis, diagnosis and treatment. Nat Rev Endocrinol. 2015;11(9):547–64. - PubMed
-
- Young J, Xu C, Papadakis GE, Acierno JS, Maione L, Hietamaki J, et al. Clinical Management of Congenital Hypogonadotropic Hypogonadism. Endocr Rev. 2019;40(2):669–710. - PubMed
-
- Cangiano B, Swee DS, Quinton R, Bonomi M. Genetics of congenital hypogonadotropic hypogonadism: peculiarities and phenotype of an oligogenic disease. Hum Genet. 2021;140(1):77–111. - PubMed
-
- Rastrelli G, Corona G, Mannucci E, Maggi M. Factors affecting spermatogenesis upon gonadotropin-replacement therapy: a meta-analytic study. Andrology. 2014;2(6):794–808. - PubMed

