Age-specific malaria vulnerability and transmission reservoir among children
- PMID: 38440360
- PMCID: PMC10911094
- DOI: 10.1016/j.gpeds.2023.100085
Age-specific malaria vulnerability and transmission reservoir among children
Abstract
Purpose: The pediatric population, especially under-five children, is highly susceptible to malaria and accounts for 76 % of global malaria deaths according to the World Malaria Report 2022. The purpose of this manuscript is to discuss the various factors involved in the susceptibility of the pediatric population to Malaria and the importance of this age group for malaria elimination.
Methodology: Data on pediatric malaria epidemiology that includes prevalence, risk factors, immune factors, socioeconomic factors, control methods, etc. were extracted from published literature using PubMed and Google Scholar. This data was further correlated with malaria incidence data from the World Health Organization (WHO) and the National Center for Vector Borne Diseases Control (NCVBDC).
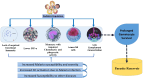
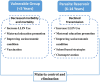
Results: The younger age group is vulnerable to severe malaria due to an immature immune system. The risk of infection and clinical disease increases after the waning of maternal immunity. In the initial years of life, the developing brain is more susceptible to malaria infection and its after-effects. The pediatric population may act as a malaria transmission reservoir due to parasite density and asymptomatic infections. WHO recommended RTS,S/AS01 has limitations and may not be applicable in all settings to propel malaria elimination.
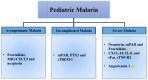
Conclusion: The diagnosis of malaria is based on clinical suspicion and confirmed with microscopy and/or rapid diagnostic testing. The school-age pediatric population serves as a transmission reservoir in the form of asymptomatic malaria since they have acquired some immunity due to exposure in early childhood. Targeting the hidden reservoir in the pediatric population and protecting this vulnerable group will be essential for malaria elimination from the countries targeting elimination.
Keywords: Asymptomatic malaria; Malaria elimination; Malaria pathogenesis; Malaria transmission reservoir; Pediatric malaria.
© 2023 The Author(s).
Conflict of interest statement
All the authors agree with the content of the manuscript and give their consent to submit and consent has also been obtained from authorities in the institutes. Authors declare no conflict of Interest.
Figures
References
-
- World Health Organization; Geneva: 2022. World Malaria Report 2022. Licence: CC BY-NC-SA 3.0 IGO.
-
- World Health Organization; Geneva: 2021. World Malaria Report 2021. Licence:CC BY-NC-SA 3.0 IGO.
-
- Ashley E.A., Poespoprodjo J.R. Treatment and prevention of malaria in children. Lancet Child Adolesc Health. 2020;4(10):775–789. - PubMed
-
- Lufungulo Bahati Y., Delanghe J., Bisimwa Balaluka G., Sadiki Kishabongo A., Philippe J. Asymptomatic submicroscopic plasmodium infection is highly prevalent and is associated with anemia in children younger than 5 Years in South Kivu/Democratic Republic of Congo. Am J Trop Med Hyg. 2020;102(5):1048–1055. - PMC - PubMed
-
- Ranjha R., Dutta G.D.P., Gitte S.V. School-age children as asymptomatic malaria reservoir in tribal villages of Bastar Region, Chhattisgarh. Indian Pediatr. 2019;56(10):873–875. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
