Progranulin and neuropathological features of Alzheimer's disease: longitudinal study
- PMID: 38441695
- PMCID: PMC10914850
- DOI: 10.1007/s40520-024-02715-9
Progranulin and neuropathological features of Alzheimer's disease: longitudinal study
Abstract
Background: Progranulin is an anti-inflammatory protein that plays an essential role in the synapse function and the maintenance of neurons in the central nervous system (CNS). It has been shown that the CSF level of progranulin increases in Alzheimer's disease (AD) patients and is associated with the deposition of amyloid-beta (Aβ) and tau in the brain tissue. In this study, we aimed to assess the longitudinal changes in cerebrospinal fluid (CSF) progranulin levels during different pathophysiological stages of AD and investigate associated AD pathologic features.
Methods: We obtained the CSF and neuroimaging data of 1001 subjects from the ADNI database. The participants were classified into four groups based on the A/T/N framework: A + /TN + , A + /TN-, A-/TN + , and A-/TN-.
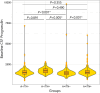
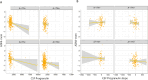
Results: Based on our analysis there was a significant difference in CSF progranulin (P = 0.001) between ATN groups. Further ANOVA analysis revealed that there was no significant difference in the rate of change of CSF-progranulin ATN groups. We found that the rate of change of CSF progranulin was associated with baseline Aβ-PET only in the A-/TN + group. A significant association was found between the rate of change of CSF progranulin and the Aβ-PET rate of change only in A-/TN + CONCLUSION: Our findings revealed that an increase in CSF progranulin over time is associated with faster formation of Aβ plaques in patients with only tau pathology based on the A/T/N classification (suspected non-Alzheimer's pathology). Together, our findings showed that the role of progranulin-related microglial activity on AD pathology can be stage-dependent, complicated, and more prominent in non-AD pathologic changes. Thus, there is a need for further studies to consider progranulin-based therapies for AD treatment.
Keywords: Alzheimer’s disease; Amyloid βeta; Microglia; Progranulin; Tau.
© 2024. The Author(s).
Conflict of interest statement
The author declares no conflict of interest regarding the publication of this paper.
Figures


Similar articles
-
Neuroimaging biomarkers and CSF sTREM2 levels in Alzheimer's disease: a longitudinal study.Sci Rep. 2024 Jul 3;14(1):15318. doi: 10.1038/s41598-024-66211-w. Sci Rep. 2024. PMID: 38961148 Free PMC article.
-
Cerebrospinal fluid progranulin is associated with increased cortical thickness in early stages of Alzheimer's disease.Neurobiol Aging. 2020 Apr;88:61-70. doi: 10.1016/j.neurobiolaging.2019.12.012. Epub 2019 Dec 20. Neurobiol Aging. 2020. PMID: 31980280
-
Early increase of CSF sTREM2 in Alzheimer's disease is associated with tau related-neurodegeneration but not with amyloid-β pathology.Mol Neurodegener. 2019 Jan 10;14(1):1. doi: 10.1186/s13024-018-0301-5. Mol Neurodegener. 2019. PMID: 30630532 Free PMC article.
-
Understanding disease progression and improving Alzheimer's disease clinical trials: Recent highlights from the Alzheimer's Disease Neuroimaging Initiative.Alzheimers Dement. 2019 Jan;15(1):106-152. doi: 10.1016/j.jalz.2018.08.005. Epub 2018 Oct 13. Alzheimers Dement. 2019. PMID: 30321505 Review.
-
The Alzheimer's Disease Neuroimaging Initiative: a review of papers published since its inception.Alzheimers Dement. 2013 Sep;9(5):e111-94. doi: 10.1016/j.jalz.2013.05.1769. Epub 2013 Aug 7. Alzheimers Dement. 2013. PMID: 23932184 Free PMC article. Review.
Cited by
-
Neuroimaging biomarkers and CSF sTREM2 levels in Alzheimer's disease: a longitudinal study.Sci Rep. 2024 Jul 3;14(1):15318. doi: 10.1038/s41598-024-66211-w. Sci Rep. 2024. PMID: 38961148 Free PMC article.
-
Neurovascular unit, neuroinflammation and neurodegeneration markers in brain disorders.Front Cell Neurosci. 2024 Oct 25;18:1491952. doi: 10.3389/fncel.2024.1491952. eCollection 2024. Front Cell Neurosci. 2024. PMID: 39526043 Free PMC article. Review.
References
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

