Plasmodium falciparum remains the dominant parasite affecting children despite decades of implementing vector control in two villages of Wolaita Zone, Southwest Ethiopia
- PMID: 38455893
- PMCID: PMC10911012
- DOI: 10.3389/fepid.2023.1305074
Plasmodium falciparum remains the dominant parasite affecting children despite decades of implementing vector control in two villages of Wolaita Zone, Southwest Ethiopia
Abstract
Background: Malaria is still a significant public health concern, and its prevention and control measures have different impacts in different areas. This study assesses the prevalence of malaria and the effectiveness of routine malaria control programmes such as indoor residual spray (IRS) in two Ethiopian villages.
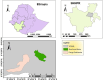
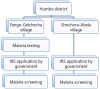
Methods: The Kebeles (villages) were purposefully selected based on their malaria prevalence rates. A parasitology survey was conducted in Fango-Gelchecha pre- and post-IRS implementation, whereas in Shochora-Abela it was only conducted post-IRS implementation. The IRS was implemented as part of the routine malaria control programme in August 2017. Every fourth house from the village registration list was systematically selected, resulting in a sample of 300 households per village. A total of 3,075 individuals were enrolled for malaria testing using microscopy.
Results: After three to four months of application of IRS in August 2017, 59 malaria cases were confirmed, resulting in an overall prevalence of 1.9% (95% CI: 1.5-2.5). Of the positive cases, 18 cases (0.59%: 95% CI: 1.3-1.8) were from Shochora-Abela village, and 41 cases (1.33%: 95% CI: 1.1-1.3) were from Fango-Gelchecha. About age categories, the prevalence of malaria was 10.1% (95% CI: 5.9-15.9) among children under five, 4.7% (95% CI: 3.3-6.4) in children aged 5-14, and only 0.32% (95% CI: 0.13-0.67) in the age group 15 and above. Overall, P. falciparum was the dominant malaria parasite, accounting for 69.5% (95% CI: 56.1-80.8), while P. vivax malaria accounted for 30.5% (95% CI: 19.2-43.8). The malaria prevalence in Fango-Gelchecha village was 3.1% (95% CI: 2.3-4.0) before IRS and 2.6% (95% CI: 1.8-3.5) after IRS application. In the village of Shochora-Abela, the prevalence of malaria post-IRS was 1.2% (95% CI: 0.7-1.9), but the prevalence prior to IRS was not evaluated.
Conclusions: Plasmodium falciparum is the predominant parasite in the villages, mainly affecting children under five. Therefore, protecting young children should be the top priority for reducing infection burdens.
Keywords: Humbo district; IRS; Plasmodium falciprum; Wolaita Zone; malaria prevalence.
© 2024 Elias and Massebo.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
Similar articles
-
The changing malaria trend and control efforts in Oromia Special zone, Amhara Regional State, North-East Ethiopia.Malar J. 2022 Apr 22;21(1):128. doi: 10.1186/s12936-022-04149-y. Malar J. 2022. PMID: 35459176 Free PMC article.
-
The Effect of Indoor Residual Spraying on the Prevalence of Malaria Parasite Infection, Clinical Malaria and Anemia in an Area of Perennial Transmission and Moderate Coverage of Insecticide Treated Nets in Western Kenya.PLoS One. 2016 Jan 5;11(1):e0145282. doi: 10.1371/journal.pone.0145282. eCollection 2016. PLoS One. 2016. PMID: 26731524 Free PMC article.
-
Differential contribution of Anopheles coustani and Anopheles arabiensis to the transmission of Plasmodium falciparum and Plasmodium vivax in two neighbouring villages of Madagascar.Parasit Vectors. 2020 Aug 26;13(1):430. doi: 10.1186/s13071-020-04282-0. Parasit Vectors. 2020. PMID: 32843082 Free PMC article.
-
Variation in species composition and infection rates of Anopheles mosquitoes at different altitudinal transects, and the risk of malaria in the highland of Dirashe Woreda, south Ethiopia.Parasit Vectors. 2017 Jul 19;10(1):343. doi: 10.1186/s13071-017-2288-0. Parasit Vectors. 2017. PMID: 28724450 Free PMC article.
-
Malaria epidemiology and interventions in Ethiopia from 2001 to 2016.Infect Dis Poverty. 2018 Nov 5;7(1):103. doi: 10.1186/s40249-018-0487-3. Infect Dis Poverty. 2018. PMID: 30392470 Free PMC article. Review.
References
-
- WHO. World malaria report: 20 years of global progress and challenges. Geneva: World Health Organization; (2020)
-
- WHO. World malaria report 2016. Geneva: World Health Organization; (2016)
LinkOut - more resources
Full Text Sources