Classification of anatomical morphology of cystic duct and its association with gallstone
- PMID: 38463380
- PMCID: PMC10921219
- DOI: 10.4240/wjgs.v16.i2.307
Classification of anatomical morphology of cystic duct and its association with gallstone
Abstract
Background: Gallstones are common lesions that often require surgical intervention. Laparoscopic cholecystectomy is the treatment of choice for symptomatic gallstones. Preoperatively, the anatomical morphology of the cystic duct (CD), needs to be accurately recognized, especially when anatomical variations occur in the CD, which is otherwise prone to bile duct injury. However, at present, there is no optimal classification system for CD morphology applicable in clinical practice, and the relationship between anatomical variations in CDs and gallstones remains to be explored.
Aim: To create a more comprehensive clinically applicable classification of the morphology of CD and to explore the correlations between anatomic variants of CD and gallstones.
Methods: A total of 300 patients were retrospectively enrolled from October 2021 to January 2022. The patients were divided into two groups: The gallstone group and the nongallstone group. Relevant clinical data and anatomical data of the CD based on magnetic resonance cholangiopancreatography (MRCP) were collected and analyzed to propose a morphological classification system of the CD and to explore its relationship with gallstones. Multivariate analysis was performed using logistic regression analyses to identify the independent risk factors using variables that were significant in the univariate analysis.
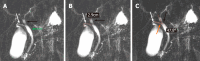
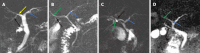
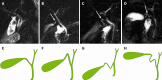
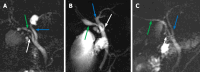
Results: Of the 300 patients enrolled in this study, 200 (66.7%) had gallstones. The mean age was 48.10 ± 13.30 years, 142 (47.3%) were male, and 158 (52.7%) were female. A total of 55.7% of the patients had a body mass index (BMI) ≥ 24 kg/m2. Based on the MRCP, the CD anatomical typology is divided into four types: Type I: Linear, type II: n-shaped, type III: S-shaped, and type IV: W-shaped. Univariate analysis revealed differences between the gallstone and nongallstone groups in relation to sex, BMI, cholesterol, triglycerides, morphology of CD, site of CD insertion into the extrahepatic bile duct, length of CD, and angle between the common hepatic duct and CD. According to the multivariate analysis, female, BMI (≥ 24 kg/m2), and CD morphology [n-shaped: Odds ratio (OR) = 10.97, 95% confidence interval (95%CI): 5.22-23.07, P < 0.001; S-shaped: OR = 4.43, 95%CI: 1.64-11.95, P = 0.003; W-shaped: OR = 7.74, 95%CI: 1.88-31.78, P = 0.005] were significantly associated with gallstones.
Conclusion: The present study details the morphological variation in the CD and confirms that CD tortuosity is an independent risk factor for gallstones.
Keywords: Anatomy; Classification; Cystic duct; Gallstone; Magnetic resonance cholangiopancreatography; Risk factor.
©The Author(s) 2024. Published by Baishideng Publishing Group Inc. All rights reserved.
Conflict of interest statement
Conflict-of-interest statement: The authors declare that they have no conflicts of interest.
Figures
References
-
- Russo MW, Wei JT, Thiny MT, Gangarosa LM, Brown A, Ringel Y, Shaheen NJ, Sandler RS. Digestive and liver diseases statistics, 2004. Gastroenterology. 2004;126:1448–1453. - PubMed
-
- Shabanzadeh DM, Sørensen LT, Jørgensen T. Determinants for gallstone formation - a new data cohort study and a systematic review with meta-analysis. Scand J Gastroenterol. 2016;51:1239–1248. - PubMed
-
- Portincasa P, Moschetta A, Palasciano G. Cholesterol gallstone disease. Lancet. 2006;368:230–239. - PubMed
-
- Marschall HU, Einarsson C. Gallstone disease. J Intern Med. 2007;261:529–542. - PubMed
LinkOut - more resources
Full Text Sources

