Pre-existing Immunocompromising Conditions and Outcomes of Acute COVID-19 Patients Admitted for Pediatric Intensive Care
- PMID: 38465976
- PMCID: PMC11327788
- DOI: 10.1093/cid/ciae133
Pre-existing Immunocompromising Conditions and Outcomes of Acute COVID-19 Patients Admitted for Pediatric Intensive Care
Abstract
Background: We aimed to determine if pre-existing immunocompromising conditions (ICCs) were associated with the presentation or outcome of patients with acute coronavirus disease 2019 (COVID-19) admitted for pediatric intensive care.
Methods: Fifty-five hospitals in 30 US states reported cases through the Overcoming COVID-19 public health surveillance registry. Patients <21 years admitted 12 March 2020-30 December 2021 to the pediatric intensive care unit (PICU) or high-acuity unit for acute COVID-19 were included.
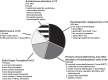
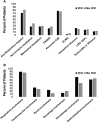
Results: Of 1274 patients, 105 (8.2%) had an ICC, including 33 (31.4%) hematologic malignancies, 24 (22.9%) primary immunodeficiencies and disorders of hematopoietic cells, 19 (18.1%) nonmalignant organ failure with solid-organ transplantation, 16 (15.2%) solid tumors, and 13 (12.4%) autoimmune disorders. Patients with ICCs were older, had more underlying renal conditions, and had lower white blood cell and platelet counts than those without ICCs, but had similar clinical disease severity upon admission. In-hospital mortality from COVID-19 was higher (11.4% vs 4.6%, P = .005) and hospitalization was longer (P = .01) in patients with ICCs. New major morbidities upon discharge were not different between those with and without ICC (10.5% vs 13.9%, P = .40). In patients with ICCs, bacterial coinfection was more common in those with life-threatening COVID-19.
Conclusions: In this national case series of patients <21 years of age with acute COVID-19 admitted for intensive care, existence of a prior ICCs were associated with worse clinical outcomes. Reassuringly, most patients with ICCs hospitalized in the PICU for severe acute COVID-19 survived and were discharged home without new severe morbidities.
Keywords: COVID-19; bacterial coinfection; critical care; immunocompromised host; pediatrics.
© The Author(s) 2024. Published by Oxford University Press on behalf of Infectious Diseases Society of America. All rights reserved. For commercial re-use, please contact reprints@oup.com for reprints and translation rights for reprints. All other permissions can be obtained through our RightsLink service via the Permissions link on the article page on our site—for further information please contact journals.permissions@oup.com.
Conflict of interest statement
Potential conflicts of interest. B. M. C. reports grants from NHLBI, American Lung Association, Doris Duke Foundation/Walder Foundation, and American Thoracic Society; payment for expert testimony from Tripplett Woolf Garretson; and participation on a multidisciplinary team for Sobi. N. B. H. reports grants from Sanofi, Quidel, and Merck. C. V. H. reports royalties, consulting fees, for Reviewer for Up To Date and Dynamed clinical databases; payment for presentations from Biofire; and expert consultation for the AstraZeneca FluMist Board. A. G. R. reports licenses as a Section Editor for Pediatric Critical Care Medicine, UpToDate, Inc; consulting fees from ThermoFisher, Inotrem; honoraria from a Grand Rounds presentation at St. Jude; support for meetings and/or travel from International Sepsis Forum, Institut Merieux, ThermoFisher; participation on an advisory board for the NIH Grace Study, REMAP-CAP, NIH-PREVENT-VILI; a medical advisory board member for Families Fighting Flu; chair member for International Sepsis Forum; and received reagents from Illumina, Inc. M. K. reports support for meetings and/or travel from the National Institute of Health (NIH) and a role on an advisory board for KultureCity. H. D. reports honoraria from Delex Pharma International, Inc. N. Z. C. reports grants from Cincinnati Children's Hospital Medical Center. J. C. F. reports grants from the National Institute of Diabetes and Digestive and Kidney Diseases (K23DK119463 and P50DK114786), and Pennsylvania CURE Grant. M. W. H. reports licenses from Kiadis, sub-board service for the American Board of Pediatrics, participation on a Data and Safety Monitoring Board (DSMB) for Abbvie, and receipt of drugs from Partner Therapeutics and Sobi. J. C. reports receipt of equipment from Illumina. B. L. reports receipt of an Immune Deficiency Foundation Research Grant. G. E. M. reports payment for expert testimony from Orlando Health, Bush Ross, Hall, Schiefflin & Smith, PA, Poole Brooks and Plumlee, PA, Hilltop Specialty Insurance, Smith, Hulsey, and Busey, PA. J. E. S. reports grants from the Food and Drug Administration (FDA), consulting fees from the Association for Professionals in Infection Control and Epidemiology (APIC), payment for presentations from the American Academy of Pediatrics, and participation on an advisory board for the American Association of Medical Colleges. All other authors report no potential conflicts. All authors have submitted the ICMJE Form for Disclosure of Potential Conflicts of Interest. Conflicts that the editors consider relevant to the content of the manuscript have been disclosed.
Figures
References
-
- Graff K, Smith C, Silveira L, et al. . Risk factors for severe COVID-19 in children. Pediatr Infect Dis J 2021; 40:e137–45. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

