Safety and timing of early therapeutic anticoagulation therapy after craniotomy
- PMID: 38468647
- PMCID: PMC10927226
- DOI: 10.25259/SNI_887_2023
Safety and timing of early therapeutic anticoagulation therapy after craniotomy
Abstract
Background: To date, there are few guidelines and studies to guide the timing of initiation of therapeutic anticoagulation (AC) after craniotomy. The goal of this study was to assess the timing, safety, and outcomes of patients following the administration of therapeutic AC after craniotomy.
Methods: A retrospective case-control study was performed evaluating all craniotomy patients from August 2017 to July 2021. Cases were selected if they received therapeutic AC within ten days of craniotomy. Nineteen out of 1013 craniotomy patients met the inclusion criteria. Indications for therapeutic AC were diverse, including deep venous thrombosis, pulmonary embolism, dural venous sinus thrombosis, mechanical heart valve, and left ventricular thrombus.
Results: The mean and median time to therapeutic AC were 5.35 and 5 days, respectively. Three patients developed intracerebral hemorrhage (ICH) that was stable on repeat imaging and did not require any surgical intervention or result in new neurologic deficits. There was no significant association between therapeutic AC and postoperative ICH (P = 0.067).
Conclusion: This study demonstrated that the initiation of therapeutic AC in postoperative craniotomy patients from postoperative days 2 to 10 did not result in any major complications. A prospective study is warranted to clarify the indications and safety of therapeutic AC after craniotomy.
Keywords: Anticoagulation therapy; Craniotomy; Intracranial hemorrhage; Mechanical heart valves; Venous thromboembolism.
Copyright: © 2024 Surgical Neurology International.
Conflict of interest statement
There are no conflicts of interest.
Figures
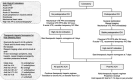

References
-
- Algattas H, Kimmell KT, Vates GE, Jahromi BS. Analysis of venous thromboembolism risk in patients undergoing craniotomy. World Neurosurg. 2015;84:1372–9. - PubMed
-
- Algattas H, Kimmell KT, Vates GE. Risk of reoperation for hemorrhage in patients after craniotomy. World Neurosurg. 2016;87:531–9. - PubMed
-
- Briggs RG, Lin YH, Dadario NB, Young IM, Conner AK, Xu W, et al. Optimal timing of post-operative enoxaparin after neurosurgery: A single institution experience. Clin Neurol Neurosurg. 2021;207:106792. - PubMed
-
- Carrier M, Le Gal G, Wells PS, Rodger MA. Systematic review: Case-fatality rates of recurrent venous thromboembolism and major bleeding events among patients treated for venous thromboembolism. Ann Intern Med. 2010;152:578–89. - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous
