Characterisation and Expression of Osteogenic and Periodontal Markers of Bone Marrow Mesenchymal Stem Cells (BM-MSCs) from Diabetic Knee Joints
- PMID: 38474098
- PMCID: PMC10931945
- DOI: 10.3390/ijms25052851
Characterisation and Expression of Osteogenic and Periodontal Markers of Bone Marrow Mesenchymal Stem Cells (BM-MSCs) from Diabetic Knee Joints
Abstract
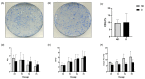
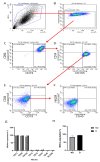
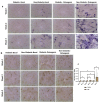
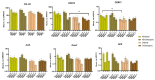
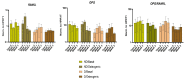
Type 2 diabetes mellitus (T2DM) represents a significant health problem globally and is linked to a number of complications such as cardiovascular disease, bone fragility and periodontitis. Autologous bone marrow mesenchymal stem cells (BM-MSCs) are a promising therapeutic approach for bone and periodontal regeneration; however, the effect of T2DM on the expression of osteogenic and periodontal markers in BM-MSCs is not fully established. Furthermore, the effect of the presence of comorbidities such as diabetes and osteoarthritis on BM-MSCs is also yet to be investigated. In the present study, BM-MSCs were isolated from osteoarthritic knee joints of diabetic and nondiabetic donors. Both cell groups were compared for their clonogenicity, proliferation rates, MSC enumeration and expression of surface markers. Formation of calcified deposits and expression of osteogenic and periodontal markers were assessed after 1, 2 and 3 weeks of basal and osteogenic culture. Diabetic and nondiabetic BM-MSCs showed similar clonogenic and growth potentials along with comparable numbers of MSCs. However, diabetic BM-MSCs displayed lower expression of periostin (POSTN) and cementum protein 1 (CEMP-1) at Wk3 osteogenic and Wk1 basal cultures, respectively. BM-MSCs from T2DM patients might be suitable candidates for stem cell-based therapeutics. However, further investigations into these cells' behaviours in vitro and in vivo under inflammatory environments and hyperglycaemic conditions are still required.
Keywords: bone marrow mesenchymal stem cells; bone regeneration; diabetes.
Conflict of interest statement
The authors declare no conflicts of interest. The authors declare that the funders had no role in the design of the study; in the collection, analyses or interpretation of data; in the writing of the manuscript; or in the decision to publish the results.
Figures
Similar articles
-
Bone marrow-derived dedifferentiated fat cells exhibit similar phenotype as bone marrow mesenchymal stem cells with high osteogenic differentiation and bone regeneration ability.J Orthop Surg Res. 2023 Mar 11;18(1):191. doi: 10.1186/s13018-023-03678-9. J Orthop Surg Res. 2023. PMID: 36906634 Free PMC article.
-
Bone marrow from periacetabular osteotomies as a novel source for human mesenchymal stromal cells.Stem Cell Res Ther. 2023 Nov 3;14(1):315. doi: 10.1186/s13287-023-03552-9. Stem Cell Res Ther. 2023. PMID: 37924114 Free PMC article.
-
Regulation of osteogenesis in bone marrow-derived mesenchymal stem cells via histone deacetylase 1 and 2 co-cultured with human gingival fibroblasts and periodontal ligament cells.J Periodontal Res. 2023 Feb;58(1):83-96. doi: 10.1111/jre.13070. Epub 2022 Nov 8. J Periodontal Res. 2023. PMID: 36346011
-
Rejuvenation of Bone Marrow Mesenchymal Stem Cells: Mechanisms and Their Application in Senile Osteoporosis Treatment.Biomolecules. 2025 Feb 13;15(2):276. doi: 10.3390/biom15020276. Biomolecules. 2025. PMID: 40001580 Free PMC article.
-
Different Sources of Mesenchymal Stem Cells for Tissue Regeneration: A Guide to Identifying the Most Favorable One in Orthopedics and Dentistry Applications.Int J Mol Sci. 2022 Jun 6;23(11):6356. doi: 10.3390/ijms23116356. Int J Mol Sci. 2022. PMID: 35683035 Free PMC article. Review.
References
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

