Opportunistic dried blood spot sampling validates and optimizes a pediatric population pharmacokinetic model of metronidazole
- PMID: 38477706
- PMCID: PMC10994817
- DOI: 10.1128/aac.01533-23
Opportunistic dried blood spot sampling validates and optimizes a pediatric population pharmacokinetic model of metronidazole
Erratum in
-
Erratum for Randell et al., "Opportunistic dried blood spot sampling validates and optimizes a pediatric population pharmacokinetic model of metronidazole".Antimicrob Agents Chemother. 2025 Sep 3;69(9):e0097225. doi: 10.1128/aac.00972-25. Epub 2025 Jul 25. Antimicrob Agents Chemother. 2025. PMID: 40711453 Free PMC article. No abstract available.
Abstract
Pharmacokinetic models rarely undergo external validation in vulnerable populations such as critically ill infants, thereby limiting the accuracy, efficacy, and safety of model-informed dosing in real-world settings. Here, we describe an opportunistic approach using dried blood spots (DBS) to evaluate a population pharmacokinetic model of metronidazole in critically ill preterm infants of gestational age (GA) ≤31 weeks from the Metronidazole Pharmacokinetics in Premature Infants (PTN_METRO, NCT01222585) study. First, we used linear correlation to compare 42 paired DBS and plasma metronidazole concentrations from 21 preterm infants [mean (SD): post natal age 28.0 (21.7) days, GA 26.3 (2.4) weeks]. Using the resulting predictive equation, we estimated plasma metronidazole concentrations (ePlasma) from 399 DBS collected from 122 preterm and term infants [mean (SD): post natal age 16.7 (15.8) days, GA 31.4 (5.1) weeks] from the Antibiotic Safety in Infants with Complicated Intra-Abdominal Infections (SCAMP, NCT01994993) trial. When evaluating the PTN_METRO model using ePlasma from the SCAMP trial, we found that the model generally predicted ePlasma well in preterm infants with GA ≤31 weeks. When including ePlasma from term and preterm infants with GA >31 weeks, the model was optimized using a sigmoidal Emax maturation function of postmenstrual age on clearance and estimated the exponent of weight on volume of distribution. The optimized model supports existing dosing guidelines and adds new data to support a 6-hour dosing interval for infants with postmenstrual age >40 weeks. Using an opportunistic DBS to externally validate and optimize a metronidazole population pharmacokinetic model was feasible and useful in this vulnerable population.
Keywords: metronidazole; pediatric; pharmacokinetics.
Conflict of interest statement
R.L.R. and E.J.T. are supported by the NICHD under Award Number T32HD104576. The spouse of R.L.R. has financial relationships with Merck & Co, Inc. and Biogen. S.J.B. receives support from the National Institutes of Health, the US Food and Drug Administration, the Childhood Arthritis and Rheumatology Research Alliance, Purdue Pharma, consulting for UCB and Rutgers, and serves on an NIH Data Safety Monitoring Board. M.C.W. receives support for research from the NIH [1U24-MD016258], National Institute of Allergy and Infectious Diseases [HHSN272201500006I, 1K24-AI143971], FDA [5U18-FD006298], and industry for drug development in adults and children. M.J.S. reports research support from Pfizer and Merck. C.P.H. receives salary support for research from NIH, FDA, the Burroughs Wellcome Fund, and other sponsors for drug development in adults and children (https://dcri.org/about-us/conflict-of-interest/). R.G.G. has received support from the NIH, the FDA, the Centers for Disease Control, and industry for research services (https://dcri.org/about-us/conflict-of-interest/). C.B. receives research support from the NIH and Aerogen. J.M.B. receives research support from NICHD (R01HD097081). H.C. receives support for research from the NIH (1R01HD109784). M.M.L. receives support from grant K24 HL143283. G.M.S. receives research support from NIH, Thrasher Research Fund, Airway Therapeutics, and ICON Clinical Research. J.H.W. is consulting for Roche Diagnostics, Inc. R.C., L.C.D., N.H., A.L., F.M., M.S., A.T., S.V., C.E.L.D., and C.H. report no funding.
Figures

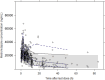
References
-
- Guo T, van Hest RM, Roggeveen LF, Fleuren LM, Thoral PJ, Bosman RJ, van der Voort PHJ, Girbes ARJ, Mathot RAA, Elbers PWG. 2019. External evaluation of population pharmacokinetic models of vancomycin in large cohorts of intensive care unit patients. Antimicrob Agents Chemother 63:e02543-18. doi: 10.1128/AAC.02543-18 - DOI - PMC - PubMed
-
- Hartman SJF, Orriëns LB, Zwaag SM, Poel T, de Hoop M, de Wildt SN. 2020. External validation of model-based dosing guidelines for vancomycin, gentamicin, and tobramycin in critically ill neonates and children: a pragmatic two-center study. Paediatr Drugs 22:433–444. doi: 10.1007/s40272-020-00400-8 - DOI - PMC - PubMed
-
- U.S. Food & Drug Administration, Issued by Center for Drug Evaluation and Research . 2022. General clinical pharmacology considerations for neonatal studies for drugs and biological products guidance for industry. Available from: https://www.fda.gov/regulatory-information/search-fda-guidance-documents.... Retrieved 1 Sep 2023.
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

