Telephone triage and dispatch of ambulances to patients with suspected and verified acute stroke - a descriptive study
- PMID: 38486156
- PMCID: PMC10941420
- DOI: 10.1186/s12873-024-00962-7
Telephone triage and dispatch of ambulances to patients with suspected and verified acute stroke - a descriptive study
Abstract
Objectives: In this study we aimed to explore EMCC triage of suspected and confirmed stroke patients to gain more knowledge about the initial phase of the acute stroke response chain. Accurate dispatch at the Emergency Medical Communication Center (EMCC) is crucial for optimal resource utilization in the prehospital service, and early identification of acute stroke is known to improve patient outcome.
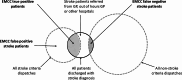
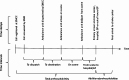
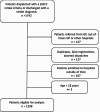
Materials and methods: We conducted a descriptive retrospective study based on data from the Emergency Department and EMCC records at a comprehensive stroke center in Oslo, Norway, during a six-month period (2019-2020). Patients dispatched with EMCC stroke criteria and/or discharged with a stroke diagnosis were included. We identified EMCC true positive, false positive and false negative stroke patients and estimated EMCC stroke sensitivity and positive predictive value (PPV). Furthermore, we analyzed prehospital time intervals and identified patient destinations to gain knowledge on ambulance services assessments.
Results: We included 1298 patients. EMCC stroke sensitivity was 77% (95% CI: 72 - 82%), and PPV was 16% (95% CI: 14 - 18%). EMCC false negative stroke patients experienced an increased median prehospital delay of 11 min (p < 0.001). Upon arrival at the scene, 68% of the EMCC false negative patients were identified as suspected stroke cases by the ambulance services. Similarly, 68% of the false positive stroke patients were either referred to a GP, out-of-hours GP acute clinic, local hospitals or left at the scene by the ambulance services, indicating that no obvious stroke symptoms were identified by ambulance personnel upon arrival at the scene.
Conclusions: This study reveals a high EMCC stroke sensitivity and an extensive number of false positive stroke dispatches. By comparing the assessments made by both the EMCC and the ambulance service, we have identified specific patient groups that should be the focus for future research efforts aimed at improving the sensitivity and specificity of stroke recognition in the EMCC.
Keywords: Emergency calls; Emergency medical communication center; Emergency medical dispatch; Emergency medical services; Prehospital care; Prehospital stroke management; Stroke pathway; Triage.
© 2024. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures


Similar articles
-
Community First Responders' role in the current and future rural health and care workforce: a mixed-methods study.Health Soc Care Deliv Res. 2024 Jul;12(18):1-101. doi: 10.3310/JYRT8674. Health Soc Care Deliv Res. 2024. PMID: 39054745
-
Emergency Medical Services Streaming Enabled Evaluation In Trauma: The SEE-IT Feasibility RCT.Health Soc Care Deliv Res. 2025 May;13(26):1-38. doi: 10.3310/EUFS2314. Health Soc Care Deliv Res. 2025. PMID: 40445854 Clinical Trial.
-
Reducing time delays and enhancing reperfusion eligibility related to stroke suspicion by the Emergency Medical Dispatch Centre: a registry-based observational study.Emerg Med J. 2025 Aug 19;42(9):599-605. doi: 10.1136/emermed-2024-214294. Emerg Med J. 2025. PMID: 40050006
-
Signs and symptoms to determine if a patient presenting in primary care or hospital outpatient settings has COVID-19.Cochrane Database Syst Rev. 2022 May 20;5(5):CD013665. doi: 10.1002/14651858.CD013665.pub3. Cochrane Database Syst Rev. 2022. PMID: 35593186 Free PMC article.
-
Rapid, point-of-care antigen tests for diagnosis of SARS-CoV-2 infection.Cochrane Database Syst Rev. 2022 Jul 22;7(7):CD013705. doi: 10.1002/14651858.CD013705.pub3. Cochrane Database Syst Rev. 2022. PMID: 35866452 Free PMC article.
Cited by
-
Factors affecting emergency medical dispatchers decision making in stroke calls - a qualitative study.BMC Emerg Med. 2024 Nov 15;24(1):214. doi: 10.1186/s12873-024-01129-0. BMC Emerg Med. 2024. PMID: 39548378 Free PMC article.
-
Frequent contacts to Emergency Medical Services (EMS): more than frequent callers.BMC Emerg Med. 2024 Oct 12;24(1):190. doi: 10.1186/s12873-024-01104-9. BMC Emerg Med. 2024. PMID: 39395931 Free PMC article.
-
Disparities between two possible thresholds for frequent contacts to a Norwegian emergency medical communication centre: ≥5 contacts in one month vs. ≥12 contacts in three months.BMC Emerg Med. 2025 Aug 29;25(1):173. doi: 10.1186/s12873-025-01333-6. BMC Emerg Med. 2025. PMID: 40877776 Free PMC article.
-
Methods for improving the identification of acute stroke during ambulance calls: A scoping review.PLoS One. 2025 Aug 13;20(8):e0327653. doi: 10.1371/journal.pone.0327653. eCollection 2025. PLoS One. 2025. PMID: 40802682 Free PMC article.
References
-
- Kim JT, Fonarow GC, Smith EE, Reeves MJ, Navalkele DD, Grotta JC, et al. Treatment with tissue plasminogen activator in the Golden Hour and the shape of the 4.5-Hour time-benefit curve in the National United States get with the guidelines-Stroke Population. Circulation. 2017;135(2):128–39. doi: 10.1161/CIRCULATIONAHA.116.023336. - DOI - PubMed
-
- Hemphill JC 3rd, Greenberg SM, Anderson CS, Becker K, Bendok BR, Cushman M, et al. Guidelines for the management of spontaneous intracerebral hemorrhage: a Guideline for Healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 2015;46(7):2032–60. - PubMed
-
- Faiz KW, Sundseth A, Thommessen B, Ronning OM. Prehospital path in acute stroke. Tidsskr nor Laegeforen. 2017;137(11):798–802. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

