Disparities Exist in the Experience of Financial Burden Among Orthopedic Trauma Patients: A Systematic Review
- PMID: 38491251
- PMCID: PMC11068702
- DOI: 10.1007/s12178-024-09890-2
Disparities Exist in the Experience of Financial Burden Among Orthopedic Trauma Patients: A Systematic Review
Abstract
Purpose of review: There are substantial costs associated with orthopedic injury and management. These costs are likely not experienced equally among patients. At the level of the healthcare and hospital systems, disparities in financial burden and patient demographics have already been identified among orthopedic trauma patients. Accordingly, disparities may also arise at the level of the patient and how they experience the cost of their care. We sought to determine (1) how patient demographics are associated with financial burden/toxicity and (2) if patients experience disproportionate financial burden/toxicity and social support secondary to their economic standing.
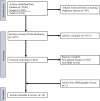
Recent findings: It has been described that there is an inequitable experience in clinical and economic outcomes in certain socioeconomic demographics leading to disparities in financial burden. It has been further reported that orthopedic injury, management, and outcomes are not experienced equitably among all demographic and socioeconomic groups. Ten articles met inclusion criteria, among which financial burden was disproportionately experienced amid orthopedic trauma patients across age, gender, race, education, and marital status. Financial hardship was also unequally distributed among different levels of income, employment, insurance status, and social deprivation. Younger, female, non-White, and unmarried patients experience increased financial burden. Patients with less education, lower income, limited or no insurance, and greater social deprivation disproportionately experienced financial toxicity compared to patients of improved economic standing. Further investigation into policy changes, social support, and barriers to appropriate care should be addressed to prevent unnecessary financial burden and promote greater patient welfare.
Keywords: Demographic disparity; Financial burden; Financial toxicity; Orthopedic trauma; Socioeconomic disparity.
© 2024. The Author(s), under exclusive licence to Springer Science+Business Media, LLC, part of Springer Nature.
Conflict of interest statement
Stephen DeMartini, Daniel Pereira, and Christopher Dy declare that they have no conflict of interest.
Figures
Similar articles
-
What Is the Financial Impact of Orthopaedic Sequelae of Intravenous Drug Use on Urban Tertiary-care Centers?Clin Orthop Relat Res. 2020 Oct;478(10):2202-2212. doi: 10.1097/CORR.0000000000001330. Clin Orthop Relat Res. 2020. PMID: 32667752 Free PMC article.
-
Financial Toxicity in Diabetes: The State of What We Know.Curr Diab Rep. 2025 May 13;25(1):32. doi: 10.1007/s11892-025-01588-0. Curr Diab Rep. 2025. PMID: 40358737 Free PMC article. Review.
-
Out-of-Pocket Annual Health Expenditures and Financial Toxicity From Healthcare Costs in Patients With Heart Failure in the United States.J Am Heart Assoc. 2021 Jul 20;10(14):e022164. doi: 10.1161/JAHA.121.022164. Epub 2021 May 16. J Am Heart Assoc. 2021. PMID: 33998273 Free PMC article.
-
Financial and employment impacts of serious injury: a qualitative study.Injury. 2014 Sep;45(9):1445-51. doi: 10.1016/j.injury.2014.01.019. Epub 2014 Jan 30. Injury. 2014. PMID: 24560090
-
Financial toxicity and employment status in cancer survivors. A systematic literature review.Support Care Cancer. 2020 Dec;28(12):5693-5708. doi: 10.1007/s00520-020-05719-z. Epub 2020 Aug 31. Support Care Cancer. 2020. PMID: 32865673 Free PMC article.
Cited by
-
Insurance Payor Status and Outcomes in Pediatric Sports-Related Injuries: A Rapid Review.Clin Pract. 2025 Mar 4;15(3):52. doi: 10.3390/clinpract15030052. Clin Pract. 2025. PMID: 40136588 Free PMC article. Review.
-
Psychological and social aspects in orthopaedics and trauma surgery, challenges and solutions in trauma: a didactic overview.EFORT Open Rev. 2025 Jun 2;10(6):431-438. doi: 10.1530/EOR-2025-0054. EFORT Open Rev. 2025. PMID: 40459162 Free PMC article.
References
-
- Liu C, Tsugawa Y, Weiser TG, Scott JW, Spain DA, Maggard-Gibbons M. Association of the US Affordable Care Act with out-of-pocket spending and catastrophic health expenditures among adult patients with traumatic injury. JAMA Netw Open. 2020;3(2):e200157. doi: 10.1001/jamanetworkopen.2020.0157. - DOI - PMC - PubMed
-
- Johnson CT, Tran A, Preslar J, Bussey-Jones J, Schenker ML. Racial disparities in the operative management of orthopedic trauma: a systematic review and meta-analysis. Am Surg. 2022:0(0):1–10. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous