Metformin and feeding increase levels of the appetite-suppressing metabolite Lac-Phe in humans
- PMID: 38499765
- PMCID: PMC11052712
- DOI: 10.1038/s42255-024-01018-7
Metformin and feeding increase levels of the appetite-suppressing metabolite Lac-Phe in humans
Abstract
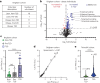
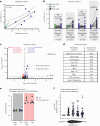
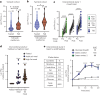
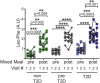
Metformin, a widely used first-line treatment for type 2 diabetes (T2D), is known to reduce blood glucose levels and suppress appetite. Here we report a significant elevation of the appetite-suppressing metabolite N-lactoyl phenylalanine (Lac-Phe) in the blood of individuals treated with metformin across seven observational and interventional studies. Furthermore, Lac-Phe levels were found to rise in response to acute metformin administration and post-prandially in patients with T2D or in metabolically healthy volunteers.
© 2024. The Author(s).
Conflict of interest statement
B.S. is due to undertake a 3-month internship at Metabolon as part of his PhD. L.L. is a member of the scientific advisory board for MiNK Therapeutics and Faeth Therapeutics. The other authors declare no competing interests.
Figures

References
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

