Prophylactic corticosteroids for cardiopulmonary bypass in adult cardiac surgery
- PMID: 38506343
- PMCID: PMC10952358
- DOI: 10.1002/14651858.CD005566.pub4
Prophylactic corticosteroids for cardiopulmonary bypass in adult cardiac surgery
Abstract
Background: Cardiac surgery triggers a strong inflammatory reaction, which carries significant clinical consequences. Corticosteroids have been suggested as a potential perioperative strategy to reduce inflammation and help prevent postoperative complications. However, the safety and effectiveness of perioperative corticosteroid use in adult cardiac surgery is uncertain. This is an update of the 2011 review with 18 studies added.
Objectives: Primary objective: to estimate the effects of prophylactic corticosteroid use in adults undergoing cardiac surgery with cardiopulmonary bypass on the: - co-primary endpoints of mortality, myocardial complications, and pulmonary complications; and - secondary outcomes including atrial fibrillation, infection, organ injury, known complications of steroid therapy, prolonged mechanical ventilation, prolonged postoperative stay, and cost-effectiveness.
Secondary objective: to explore the role of characteristics of the study cohort and specific features of the intervention in determining the treatment effects via a series of prespecified subgroup analyses.
Search methods: We used standard, extensive Cochrane search methods to identify randomised studies assessing the effect of corticosteroids in adult cardiac surgery. The latest searches were performed on 14 October 2022.
Selection criteria: We included randomised controlled trials in adults (over 18 years, either with a diagnosis of coronary artery disease or cardiac valve disease, or who were candidates for cardiac surgery with the use of cardiopulmonary bypass), comparing corticosteroids with no treatments. There were no restrictions with respect to length of the follow-up period. All selected studies qualified for pooling of results for one or more endpoints.
Data collection and analysis: We used standard Cochrane methods. Our primary outcomes were all-cause mortality, and cardiac and pulmonary complications. Secondary outcomes were infectious complications, gastrointestinal bleeding, occurrence of new post-surgery atrial fibrillation, re-thoracotomy for bleeding, neurological complications, renal failure, inotropic support, postoperative bleeding, mechanical ventilation time, length of stays in the intensive care unit (ICU) and hospital, patient quality of life, and cost-effectiveness. We used GRADE to assess the certainty of evidence for each outcome.
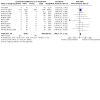
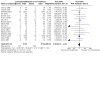
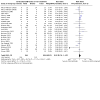
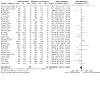
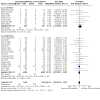
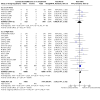
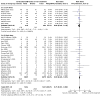
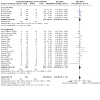
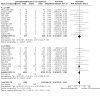
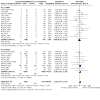
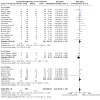
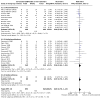
Main results: This updated review includes 72 randomised trials with 17,282 participants (all 72 trials with 16,962 participants were included in data synthesis). Four trials (6%) were considered at low risk of bias in all the domains. The median age of participants included in the studies was 62.9 years. Study populations consisted mainly (89%) of low-risk, first-time coronary artery bypass grafting (CABG) or valve surgery. The use of perioperative corticosteroids may result in little to no difference in all-cause mortality (risk with corticosteroids: 25 to 36 per 1000 versus 33 per 1000 with placebo or no treatment; risk ratio (RR) 0.90, 95% confidence interval (CI) 0.75 to 1.07; 25 studies, 14,940 participants; low-certainty evidence). Corticosteroids may increase the risk of myocardial complications (68 to 86 per 1000) compared with placebo or no treatment (66 per 1000; RR 1.16, 95% CI 1.04 to 1.31; 25 studies, 14,766 participants; low-certainty evidence), and may reduce the risk of pulmonary complications (risk with corticosteroids: 61 to 77 per 1000 versus 78 per 1000 with placebo/no treatment; RR 0.88, 0.78 to 0.99; 18 studies, 13,549 participants; low-certainty evidence). Analyses of secondary endpoints showed that corticosteroids may reduce the incidence of infectious complications (risk with corticosteroids: 94 to 113 per 1000 versus 123 per 1000 with placebo/no treatment; RR 0.84, 95% CI 0.76 to 0.92; 28 studies, 14,771 participants; low-certainty evidence). Corticosteroids may result in little to no difference in incidence of gastrointestinal bleeding (risk with corticosteroids: 9 to 17 per 1000 versus 10 per 1000 with placebo/no treatment; RR 1.21, 95% CI 0.87 to 1.67; 6 studies, 12,533 participants; low-certainty evidence) and renal failure (risk with corticosteroids: 23 to 35 per 1000 versus 34 per 1000 with placebo/no treatment; RR 0.84, 95% CI 0.69 to 1.02; 13 studies, 12,799; low-certainty evidence). Corticosteroids may reduce the length of hospital stay, but the evidence is very uncertain (-0.5 days, 0.97 to 0.04 fewer days of length of hospital stay compared with placebo/no treatment; 25 studies, 1841 participants; very low-certainty evidence). The results from the two largest trials included in the review possibly skew the overall findings from the meta-analysis.
Authors' conclusions: A systematic review of trials evaluating the organ protective effects of corticosteroids in cardiac surgery demonstrated little or no treatment effect on mortality, gastrointestinal bleeding, and renal failure. There were opposing treatment effects on cardiac and pulmonary complications, with evidence that corticosteroids may increase cardiac complications but reduce pulmonary complications; however, the level of certainty for these estimates was low. There were minor benefits from corticosteroid therapy for infectious complications, but the evidence on hospital length of stay was very uncertain. The inconsistent treatment effects across different outcomes and the limited data on high-risk groups reduced the applicability of the findings. Further research should explore the role of these drugs in specific, vulnerable cohorts.
Trial registration: ClinicalTrials.gov NCT03002259.
Copyright © 2024 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Conflict of interest statement
RGA: has declared that he has no conflict of interest. RGA was a content editor for Cochrane Heart but had no role in the editorial process for this review. Although working as a health professional as a Clinical Research Fellow in Cardiothoracic Surgery and as a cardiac surgeon for Imperial College Healthcare NHS Trust, he does not benefit from the positions expressed in this review.
GO: has declared that he has no conflict of interest. Despite working as a cardiothoracic surgeon at ASST G.O.M. Niguarda Hospital, he does not benefit from the positions expressed in this review.
RC: has declared that she has no conflict of interest. Despite working as a cardiothoracic surgeon with a National Training Number (NTN), she does not benefit from the positions expressed in this review.
FG: has declared that she has no conflict of interest. Despite working as a cardiothoracic surgeon NTN, she does not benefit from the positions expressed in this review.
NT: has declared that he has no conflict of interest. He currently holds an NTN in Cardiothoracic Surgery, and is a Higher Speciality Trainee at Health Education East Midlands. Despite working as a Cardiothoracic Surgery Registrar at Glenfield Hospital, he does not benefit from the positions expressed in this review.
KE: has declared that she has no conflict of interest. Despite working as a health professional, she does not benefit from the positions expressed in this review.
DF: has declared that he has no conflict of interest. Daniel Fudulu has published several papers on the use of prophylactic corticosteroids in paediatric heart surgery whilst employed at the University of Bristol. Despite working as a Clinical Lecturer in cardiac surgery at Bristol Royal Infirmary, he does not benefit from the positions expressed in this review.
RM: has declared that he has no conflict of interest. Despite working as a health professional, he does not benefit from the positions expressed in this review.
MK: has declared that he has no conflict of interest. Despite working as a consultant of cardiothoracic and vascular surgery at the Deutsches Herzzentrum der Charité in Berlin, he does not benefit from the positions expressed in this review.
GE: has declared that he has no conflict of interest. Despite working as a health professional, he does not benefit from the positions expressed in this review.
FL: has declared that she has no conflict of interest.
ML: declares that he has received personal payments for expert testimony, consulting fees, honoraria for lectures/presentations from Baxter, 3M, Nordic and Medtronic, unrelated to the current work. Despite working as a health professional, he does not benefit from the positions expressed in this review.
SK: has declared that he has no conflict of interest. Despite working as a consultant cardiothoracic surgeon at South Tees Hospital, he does not benefit from the positions expressed in this review.
MZ: has declared that he has no conflict of interest. Despite working as a health professional, he does not benefit from the positions expressed in this review.
GJM: undertakes unpaid work as a grant committee member for the British Heart Foundation. He also receives a grant for the British Heart Foundation that is paid to the University of Leicester and his salary was part funded by this grant until 2022. GJM also declares a grant from NIHR (health technology assessment grant, programme development grants), which is paid to his institution, though he can direct these resources to fund research in line with the grant specifications. Despite working as a cardiac surgeon, University Hospitals, Leicester, he does not benefit from the positions expressed in this review.
Figures































Update of
-
Prophylactic corticosteroids for cardiopulmonary bypass in adults.Cochrane Database Syst Rev. 2011 May 11;(5):CD005566. doi: 10.1002/14651858.CD005566.pub3. Cochrane Database Syst Rev. 2011. Update in: Cochrane Database Syst Rev. 2024 Mar 20;3:CD005566. doi: 10.1002/14651858.CD005566.pub4. PMID: 21563145 Updated.
References
References to studies included in this review
Abbaszadeh 2012 {published data only}
-
- Abbaszadeh M, Khan ZH, Mehrani F, Jahanmehr H. Perioperative intravenous corticosteroids reduce incidence of atrial fibrillation following cardiac surgery: a randomized study. Brazilian Journal of Cardiovascular Surgery 2012 ;27(1):18-23. [DOI: ] - PubMed
Abd El‐Hakeem 2003a {published data only}
-
- Abd El-Hakeem JJ, Zareh ZE. Effects of dexamethasone on the incidence of shivering and recovery in patients undergoing valve replacement surgery. Egyptian Journal of Anaesthesia 2003;19:361-70. [EMBASE: 37369829]
Abd El‐Hakeem 2003b {published data only}
-
- Abd El-Hakeem EE, Ashry MA, El-Minshawy A, Maghraby EA. Influence of dexamethasone on cytokine balance in patients undergoing valve replacement surgery. Egyptian Journal of Anaesthesia 2003;3:205-14. [RESEARCHGATE: www.researchgate.net/publication/288809174_Influence_of_dexamethasone_on...
Al‐Shawabkeh 2017 {published data only}
Amr 2009 {published data only}
-
- Amr YM, Elmisekawy E, El-serogy H. Effects of dexamethasone on pulmonary and renal functions in patients undergoing CABG with cardiopulmonary bypass. Seminars in Cardiothoracic and Vascular Anesthesia 2009;13(4):231-7. [DOI: ] - PubMed
Andersen 1989 {published data only}
-
- Andersen LW, Baek L, Thomsen BS, Rasmussen JP. Effect of methylprednisolone on endotoxemia and complement activation during cardiac surgery. Journal of Cardiothoracic Anesthesia 1989;3(5):544-9. [PMID: ] - PubMed
Bingol 2005 {published data only}
-
- Bingol H, Cingoz F, Balkan A, Kilic S, Bolcal C, Demirkilic U, et al. The effect of oral prednisolone with chronic obstructive pulmonary disease undergoing coronary artery bypass surgery. Journal of Cardiac Surgery 2005;20:252-6. [DOI: ] - PubMed
Boscoe 1983 {published data only}
Bourbon 2004 {published data only}
-
- Bourbon A, Vionnet M, Leprince P, Vaissier E, Copeland J, McDonagh P, et al. The effect of methylprednisolone treatment on the cardiopulmonary bypass-induced systemic inflammatory response. European Journal of Cardio-Thoracic Surgery 2004;26(5):932-8. [PMID: ] - PubMed
Cavarocchi 1986 {published data only}
-
- Cavarocchi NC, Pluth JR, Schaff HV, Orszulak TA, Homburger HA, Solis E, et al. Complement activation during cardiopulmonary bypass: comparison of bubble and membrane oxygenators. Journal of Thoracic and Cardiovascular Surgery 1986;91(2):252-8. [PMID: ] - PubMed
Celik 2004 {published data only}
-
- Celik JB, Gormus N, Okesli S, Gormus ZI, Solak H. Methylprednisolone prevents inflammatory reaction occurring during cardiopulmonary bypass: effects on TNF-alpha, IL-6, IL-8, IL-10. Perfusion 2004;19(3):185-91. [PMID: ] - PubMed
Chaney 1998 {published data only}
-
- Chaney MA, Nikolov MP, Blakeman B, Bakhos M, Slogoff S. Pulmonary effects of methylprednisolone in patients undergoing coronary artery bypass grafting and early tracheal extubation. Anesthesia and Analgesia 1998;87(1):27-33. [PMID: ] - PubMed
-
- Chaney MA, Nikolov MP, Blakeman BP, Bakhos M, Slogoff S. Hemodynamic effects of methylprednisolone in patients undergoing cardiac operation and early extubation. Annals of Thoracic Surgery 1999;67(4):1006-11. [PMID: ] - PubMed
Chaney 2001 {published data only}
-
- Chaney MA, Durazo-Arvizu RA, Nikolov MP, Blakeman BP, Bakhos M. Methylprednisolone does not benefit patients undergoing coronary artery bypass grafting and early tracheal extubation. Journal of Thoracic and Cardiovascular Surgery 2001;121(3):561-9. [PMID: ] - PubMed
Codd 1977 {published data only}
-
- Codd JE, Wiens RD, Barner HB, Kaiser GC, Willman VL. Steroids and myocardial preservation. Journal of Thoracic and Cardiovascular Surgery 1977;74(3):418-22. [PMID: ] - PubMed
Coetzer 1996 {published data only}
-
- Coetzer M, Coetzee A, Rossouw G. The effect of methylprednisolone, given prior to cardiopulmonary bypass, on indices of gas exchange. Cardiovascular Journal of South Africa 1996;86:C188-92. [DOI: 10.10520/AJA10159657_484] - DOI
Demir 2009 {published data only}
-
- Demir T, Demir H, Tansel T, Kalko Y, Tireli E, Dayioglu E, et al. Influence of methylprednisolone on levels of neuron-specific enolase in cardiac surgery: a corticosteroid derivative to decrease possible neuronal damage. Journal of Cardiac Surgery 2009;24:397-403. [DOI: ] - PubMed
Demir 2015 {published data only}
-
- Demir T, Ergenoglu MU, Demir HB, Tanrikulu N, Sahin M, Gok E, et al. Pretreatment with methylprednisolone improves myocardial protection during on-pump coronary artery bypass surgery. Heart Surgery Forum 2015;18(4):E171-7. [DOI: ] - PubMed
Dieleman 2012 {published data only}
-
- Bunge JJ, Osch D, Dieleman JM, Jacob KA, Kluin J, Van Dijk D, et al. Dexamethasone for the prevention of postpericardiotomy syndrome: a DExamethasone for Cardiac Surgery substudy. American Heart Journal 2014;168(1):126-31. [DOI: ] - PubMed
-
- Dieleman JM, Nierich AP, Rosseel PM, Maaten JM, Hofland J, Diephuis JC, et al. Intraoperative high-dose dexamethasone for cardiac surgery: a randomized controlled trial. JAMA 2012;308(17):1761-7. [DOI: ] - PubMed
-
- Dieleman JM, Wit GA, Nierich AP, Rosseel PM, Maaten JM, Hofland J, et al. Long‐term outcomes and cost effectiveness of high‐dose dexamethasone for cardiac surgery: a randomised trial. Anaesthesia 2017;72(6):704-13. [DOI: ] - PubMed
El Azab 2002 {published data only}
-
- El Azab SR, Rosseel PM, Lange JJ, Groeneveld AB, Strik R, Wijk EM, et al. Dexamethasone decreases the pro- to anti-inflammatory cytokine ratio during cardiac surgery. British Journal of Anaesthesia 2002;88(4):496-501. [PMID: ] - PubMed
Enc 2006 {published data only}
-
- Enc Y, Karaca P, Ayoglu U, Camur G, Kurc E, Cicek S. The acute cardioprotective effect of glucocorticoid in myocardial ischemia-reperfusion injury occurring during cardiopulmonary bypass. Heart and Vessels 2006;21(3):152-6. [PMID: ] - PubMed
Engelman 1995 {published data only}
-
- Engelman RM, Rousou JA, Flack JE 3rd, Deaton DW, Kalfin R, Das DK. Influence of steroids on complement and cytokine generation after cardiopulmonary bypass. Annals of Thoracic Surgery 1995;60(3):801-4. [PMID: ] - PubMed
Ferries 1984 {published data only}
-
- Ferries LH, Marx JJ, Ray JF. The effect of methylprednisolone on complement activation during cardiopulmonary bypass. Journal of Extracorporeal Technology 1984;16:83-8. [DOI: ]
Fillinger 2002 {published data only}
-
- Fillinger MP, Rassias AJ, Guyre PM, Sanders JH, Beach M, Pahl J, et al. Glucocorticoid effects on the inflammatory and clinical responses to cardiac surgery. Journal of Cardiothoracic and Vascular Anesthesia 2002;16(2):163-9. [PMID: ] - PubMed
Giomarelli 2003 {published and unpublished data}
-
- Giomarelli P, Scolletta S, Borrelli E, Biagioli B. Myocardial and lung injury after cardiopulmonary bypass: role of interleukin (IL)-10. Annals of Thoracic Surgery 2003;76(1):117-23. [PMID: ] - PubMed
Glumac 2017 {published data only}
-
- Glumac S, Kardum G, Sodic L, Supe-Domic D, Karanovic N. Effects of dexamethasone on early cognitive decline after cardiac surgery. European Journal of Anaesthesiology 2017;34(11):776-84. [DOI: ] - PubMed
Gomez Polo 2018 {published data only}
-
- Gomez Polo JC, Vilacosta I, Gomez-Alvarez Z, Vivas D, Martin-Garcia AG, Fortuny-Frau E, et al. Short term use of corticosteroids in the prophylaxis of atrial fibrillation after cardiac surgery and impact on the levels of acute phase proteins in this context. European Heart Journal 2018 ;39 Suppl 1:ehy563-3275. [DOI: ]
Halonen 2007 {published data only}
-
- Halonen J, Halonen P, Jarvinen O, Taskinen P, Auvinen T, Tarkka M, et al. Corticosteroids for the prevention of atrial fibrillation after cardiac surgery: a randomized controlled trial. JAMA 2007;297(14):1562-7. [PMID: ] - PubMed
Halvorsen 2003 {published data only}
-
- Halvorsen P, Raeder J, White PF, Almdahl SM, Nordstrand K, Saatvedt K, et al. The effect of dexamethasone on side effects after coronary revascularization procedures. Anesthesia and Analgesia 2003;96(6):1578-83. [PMID: ] - PubMed
Hao 2019 {published data only}
-
- Hao X, Han J, Zeng H, Wang H, Li G, Jiang C, et al. The effect of methylprednisolone prophylaxis on inflammatory monocyte subsets and suppressive regulatory T cells of patients undergoing cardiopulmonary bypass. Perfusion 2019;34(5):364-74. [DOI: ] - PubMed
Harig 1999 {published data only}
-
- Harig F, Feyrer R, Mahmoud FO, Blum U, Emde J. Reducing the post-pump syndrome by using heparin-coated circuits, steroids, or aprotinin. Thoracic and Cardiovascular Surgeon 1999;47(2):111-8. [PMID: ] - PubMed
-
- Harig F, Hohenstein B, Emde J, Weyand M. Modulating IL-6 and IL-10 levels by pharmacologic strategies and the impact of different extracorporeal circulation parameters during cardiac surgery. Shock 2001;16 Suppl 1:33-8. [PMID: ] - PubMed
Hauer 2012 {published data only}
-
- Hauer D, Weis F, Campolongo P, Schopp M, Beiras-Fernandez A, Strewe C, et al. Glucocorticoid-endocannabinoid interaction in cardiac surgical patients. Relationship to early cognitive dysfunction and late depression. Reviews in the Neurosciences 2012;23(5-6):681–90. [DOI: ] - PubMed
-
- NCT00490828. Influence of hydrocortisone on immunologic markers and health care related quality of life in patients after cardiac surgery [Influence of hydrocortisone on humoral and cellular immunologic markers in high risk patients after cardiac surgery]. clinicaltrials.gov/ct2/show/NCT00490828 (first received 25 June 2007). [CLINICALTRIALS.GOV: NCT00490828]
Jansen 1991 {published data only}
-
- Jansen NJ, Oeveren W, den Broek L, Oudemans-van Straaten HM, Stoutenbeek CP, Joen MC, et al. Inhibition by dexamethasone of the reperfusion phenomena in cardiopulmonary bypass. Journal of Thoracic and Cardiovascular Surgery 1991;102(4):515-25. [PMID: ] - PubMed
Kerr 2012 {published data only}
Kilger 2003a {published data only}
-
- Kilger E, Weis F, Briegel J, Frey L, Goetz AE, Reuter D, et al. Stress doses of hydrocortisone reduce severe systemic inflammatory response syndrome and improve early outcome in a risk group of patients after cardiac surgery. Critical Care Medicine 2003;31(4):1068-74. [PMID: ] - PubMed
-
- Schelling G, Kilger E, Roozendaal B, Quervain DJ, Briegel J, Dagge A, et al. Stress doses of hydrocortisone, traumatic memories, and symptoms of posttraumatic stress disorder in patients after cardiac surgery: a randomized study. Biological Psychiatry 2004;55(6):627-33. [PMID: ] - PubMed
Kilger 2003b {published data only}
-
- Kilger E, Weis F, Briegel J. Einfluss von Hydrocortison auf die Klinische Entwicklung bei Operationen mit Herz-Lung-Maschine. Journal für Anästhesie 2003;10:135-6. [URL: https://scholar.google.com/scholar_lookup?title=Einfluss+von+Hydrocortis...]
Kilickan 2008 {published data only}
-
- Kilickan L, Yumuk Z, Bayindir O. The effect of combined preinduction thoracic epidural anaesthesia and glucocorticoid administration on perioperative interleukin-10 levels and hyperglycemia. A randomized controlled trial. Journal of Cardiovascular Surgery 2008;49(1):87-93. [PMID: ] - PubMed
Liakopoulos 2007 {published data only}
-
- Liakopoulos OJ, Schmitto JD, Kazmaier S, Brauer A, Quintel M, Schoendube FA, et al. Cardiopulmonary and systemic effects of methylprednisolone in patients undergoing cardiac surgery. Annals of Thoracic Surgery 2007;84(1):110-8; discussion 118-9. [PMID: ] - PubMed
Loef 2004 {published data only}
-
- Loef BG, Henning RH, Epema AH, Rietman GW, Oeveren W, Navis GJ, et al. Effect of dexamethasone on perioperative renal function impairment during cardiac surgery with cardiopulmonary bypass. British Journal of Anaesthesia 2004;93(6):793-8. [PMID: ] - PubMed
-
- Morariu AM, Loef BG, Aarts LP, Rietman GW, Rakhorst G, Oeveren W, et al. Dexamethasone: benefit and prejudice for patients undergoing on-pump coronary artery bypass grafting: a study on myocardial, pulmonary, renal, intestinal, and hepatic injury. Chest 2005;128(4):2677-87. [PMID: ] - PubMed
Lomirovotov 2013 {published data only}
-
- Lomivorotov VV, Efremov SM, Kalinichenko AP, Kornilov IA, Knazkova LG, Chernyavskiy AM, et al. Methylprednisolone use is associated with endothelial cell activation following cardiac surgery. Heart, Lung and Circulation 2013 ;22(1):25-30. [DOI: ] - PubMed
Maddalli 2019 {published data only}
Mahrose 2019 {published data only}
-
- Mahrose R, Elsayed AM, Elshorbagy MS. Bisoprolol versus corticosteroid and bisoprolol combination for prevention of atrial fibrillation after on-pump coronary artery bypass graft surgery. Open Anesthesia Journal 2019;13(1):18-24. [DOI: ]
Mardani 2012 {published data only}
-
- Mardani D, Bigdelian H. The effect of dexamethasone prophylaxis on postoperative delirium after cardiac surgery: a randomized trial. Journal of Research in Medical Sciences 2012 ;17:S113-19. [URL: www.researchgate.net/profile/Davoud-Mardani/publication/227859160_The_ef...] - PMC - PubMed
Mayumi 1997 {published data only}
-
- Mayumi H, Zhang QW, Nakashima A, Masuda M, Kohno H, Kawachi Y, et al. Synergistic immunosuppression caused by high-dose methylprednisolone and cardiopulmonary bypass. Annals of Thoracic Surgery 1997;63(1):129-37. [PMID: ] - PubMed
McBride 2004 {published data only}
-
- McBride WT, Allen S, Gormley SM, Young IS, McClean E, MacGowan SW, et al. Methylprednisolone favourably alters plasma and urinary cytokine homeostasis and subclinical renal injury at cardiac surgery. Cytokine 2004;27(2-3):81-9. [PMID: ] - PubMed
Morton 1976 {published data only}
-
- Morton JR, Hiebert CA, Lutes CA, White RL. Effect of methylprednisolone on myocardial preservation during coronary artery surgery. American Journal of Surgery 1976;131(4):419-22. [PMID: ] - PubMed
Murphy 2011 {published data only}
-
- Murphy GS, Sherwani SS, Szokol JW, Avram MJ, Greenberg SB, Patel KM, et al. Small-dose dexamethasone improves quality of recovery scores after elective cardiac surgery: a randomized, double-blind, placebo-controlled study. Journal of Cardiothoracic and Vascular Anesthesia 2011;25(6):950-60. [DOI: ] - PubMed
Oliver 2004 {published data only}
-
- Oliver WC Jr, Nuttall GA, Orszulak TA, Bamlet WR, Abel MD, Ereth MH, et al. Hemofiltration but not steroids results in earlier tracheal extubation following cardiopulmonary bypass: a prospective, randomized double-blind trial. Anesthesiology 2004;101(2):327-39. [PMID: ] - PubMed
Prasongsukarn 2005 {published data only}
-
- Prasongsukarn K, Abel JG, Jamieson WR, Cheung A, Russell JA, Walley KR, et al. The effects of steroids on the occurrence of postoperative atrial fibrillation after coronary artery bypass grafting surgery: a prospective randomized trial. Journal of Thoracic and Cardiovascular Surgery 2005;130(1):93-8. [PMID: ] - PubMed
Rao 1977 {published data only}
-
- Rao G, King J, Ford W, King G. The effects of methylprednisolone on the complications of coronary artery surgery. Vascular Surgery 1977;11(1):1-7. [PMID: ] - PubMed
Rubens 2005 {published data only}
-
- Rubens FD, Nathan H, Labow R, Williams KS, Wozny D, Karsh J, et al. Effects of methylprednisolone and a biocompatible copolymer circuit on blood activation during cardiopulmonary bypass. Annals of Thoracic Surgery 2005;79(2):655-65. [PMID: ] - PubMed
Rumalla 2001 {published data only}
-
- Rumalla V, Calvano SE, Spotnitz AJ, Krause TJ, Lin E, Lowry SF. The effects of glucocorticoid therapy on inflammatory responses to coronary artery bypass graft surgery. Archives of Surgery 2001;136(9):1039-44. [PMID: ] - PubMed
Sano 2003 {published data only}
-
- Sano T, Morita S, Masuda M, Tomita Y, Nishida T, Tatewaki H, et al. Cardiopulmonary bypass, steroid administration, and surgical injury synergistically impair memory T cell function and antigen presentation. Interactive Cardiovascular and Thoracic Surgery 2003;2(4):598-602. [PMID: ] - PubMed
Sano 2006 {published data only}
-
- Sano T, Morita S, Masuda M, Yasui H. Minor infection encouraged by steroid administration during cardiac surgery. Asian Cardiovascular & Thoracic Annals 2006;14(6):505-10. [PMID: ] - PubMed
Schurr 2001 {published data only}
-
- Schurr UP, Zund G, Hoerstrup SP, Grunenfelder J, Maly FE, Vogt PR, et al. Preoperative administration of steroids: influence on adhesion molecules and cytokines after cardiopulmonary bypass. Annals of Thoracic Surgery 2001;72(4):1316-20. [PMID: ] - PubMed
Sobieski 2008 {published data only}
Starobin 2007 {published data only}
Taleska Stupica 2020 {published data only}
-
- Taleska Stupica G, Sostaric M, Bozhinovska M, Rupert L, Bosnic Z, Jerin A, et al. Extracorporeal hemadsorption versus glucocorticoids during cardiopulmonary bypass: a prospective, randomized, controlled trial. Cardiovascular Therapeutics 2020;2020:15. [DOI: 10.1155/2020/7834173] - DOI - PMC - PubMed
Tassani 1999 {published data only}
-
- Tassani P, Richter JA, Barankay A, Braun SL, Haehnel C, Spaeth P, et al. Does high-dose methylprednisolone in aprotinin-treated patients attenuate the systemic inflammatory response during coronary artery bypass grafting procedures? Journal of Cardiothoracic and Vascular Anesthesia 1999;13(2):165-72. [PMID: ] - PubMed
Toft 1997 {published data only}
-
- Toft P, Christiansen K, Tonnesen E, Nielsen CH, Lillevang S. Effect of methylprednisolone on the oxidative burst activity, adhesion molecules and clinical outcome following open heart surgery. Scandinavian Cardiovascular Journal 1997;31(5):283-8. [PMID: ] - PubMed
Turkoz 2001 {published data only}
-
- Turkoz A, Cigli A, But K, Sezgin N, Turkoz R, Gulcan O, et al. The effects of aprotinin and steroids on generation of cytokines during coronary artery surgery. Journal of Cardiothoracic and Vascular Anesthesia 2001;15(5):603-10. [PMID: ] - PubMed
Volk 2001 {published data only}
-
- Volk T, Schmutzler M, Engelhardt L, Docke WD, Volk HD, Konertz W, et al. Influence of aminosteroid and glucocorticoid treatment on inflammation and immune function during cardiopulmonary bypass. Critical Care Medicine 2001;29(11):2137-42. [PMID: ] - PubMed
Volk 2003 {published data only}
-
- Volk T, Schmutzler M, Engelhardt L, Pantke U, Laule M, Stangl K, et al. Effects of different steroid treatment on reperfusion-associated production of reactive oxygen species and arrhythmias during coronary surgery. Acta Anaesthesiologica Scandinavica 2003;47(6):667-74. [PMID: ] - PubMed
Von Spiegel 2001 {published data only}
-
- Von Spiegel T, Giannaris S, Wietasch GJ, Schroeder S, Buhre W, Schorn B, et al. Effects of dexamethasone on intravascular and extravascular fluid balance in patients undergoing coronary bypass surgery with cardiopulmonary bypass. Anesthesiology 2002;96(4):827-34. [PMID: ] - PubMed
-
- Von Spiegel T, Giannaris S, Wrigge H, Schorn B, Hoeft A. Effects of dexamethasone on extravascular lung water and pulmonary haemodynamics in patients undergoing coronary artery bypass surgery [Einfluss einer präoperativen dexamethasongabe auf das extravaskulare lungenwasser und die pulmonale hämodynamik bei koronarchirurgischen patienten]. Anasthesiologie, Intensivmedizin, Notfallmedizin, Schmerztherapie 2001;36(9):545-51. [PMID: ] - PubMed
Vukovic 2011 {published data only}
-
- Vukovic PM, Maravic-Stojkovic VR, Peric MS, Jovic MD, Cirkovic MV, Gradinac SD, et al. Steroids and statins: an old and a new anti-inflammatory strategy compared. Perfusion 2011;26(1):31-7. [DOI: ] - PubMed
Wan 1999 {published data only}
-
- Wan S, LeClerc JL, Huynh CH, Schmartz D, DeSmet JM, Yim AP, et al. Does steroid pretreatment increase endotoxin release during clinical cardiopulmonary bypass? Journal of Thoracic and Cardiovascular Surgery 1999;117(5):1004-8. [PMID: ] - PubMed
Weis 2006 {published data only}
-
- Weis F, Kilger E, Roozendaal B, Quervain DJ, Lamm P, Schmidt M, et al. Stress doses of hydrocortisone reduce chronic stress symptoms and improve health-related quality of life in high-risk patients after cardiac surgery: a randomized study. Journal of Thoracic and Cardiovascular Surgery 2006;131(2):277-82. [PMID: ] - PubMed
Weis 2009 {published data only}
-
- Weis F, Beiras-Fernandez A, Schelling G, Briegel J, Lang P, Hauer D, et al. Stress doses of hydrocortisone in high-risk patients undergoing cardiac surgery: effects on interleukin-6 to interleukin-10 ratio and early outcome. Critical Care Medicine 2009;37(5):1685-90. [DOI: ] - PubMed
Whitlock 2006 {published data only}
-
- Whitlock RP, Young E, Noora J, Farrokhyar F, Blackall M, Teoh KH. Pulse low dose steroids attenuate post-cardiopulmonary bypass SIRS; SIRS I. Journal of Surgical Research 2006;132(2):188-94. [PMID: ] - PubMed
Whitlock 2015 {published data only}
-
- McClure G, Belley-Cote E, Tong W, Xie F, Vincent J, Lamy A, et al. Steroids in cardiac surgery (SIRS): economics substudy. Canadian Journal of Cardiology 2017;33(10):S93-4. [DOI: ]
-
- McClure GR, Belley-Cote EP, Harlock J, Lamy A, Stacey M, Devereaux PJ, et al. Steroids in cardiac surgery trial: a substudy of surgical site infections. Canadian Journal of Anesthesia 2019;66(2):182-92. [DOI: ] - PubMed
-
- Paparella D, Parolari A, Rotunno C, Vincent J, Myasoedova V, Guida P, et al. The effects of steroids on coagulation dysfunction induced by cardiopulmonary bypass: a steroids in cardiac surgery (SIRS) trial substudy. Seminars in Thoracic and Cardiovascular Surgery 2017;29(1):35-44. [DOI: ] - PubMed
-
- Royse CF, Saager L, Whitlock R, Ou-Young J, Royse A, Vincent J, et al. Impact of methylprednisolone on postoperative quality of recovery and delirium in the steroids in cardiac surgery trial: a randomized, double-blind, placebo-controlled substudy. Anesthesiology 2017;126(2):223-33. [DOI: ] - PubMed
Yared 1998 {published data only}
-
- Yared JP, Starr NJ, Hoffmann-Hogg L, Bashour CA, Insler SR, O'Connor M, et al. Dexamethasone decreases the incidence of shivering after cardiac surgery: a randomized, double-blind, placebo-controlled study. Anesthesia and Analgesia 1998;87(4):795-9. [PMID: ] - PubMed
-
- Yared JP, Starr NJ, Torres FK, Bashour CA, Bourdakos G, Piedmonte M, et al. Effects of single dose, postinduction dexamethasone on recovery after cardiac surgery. Annals of Thoracic Surgery 2000;69(5):1420-4. [PMID: ] - PubMed
Yared 2007 {published data only}
-
- Yared JP, Bakri MH, Erzurum SC, Moravec CS, Laskowski DM, Van Wagoner DR, et al. Effect of dexamethasone on atrial fibrillation after cardiac surgery: prospective, randomized, double-blind, placebo-controlled trial. Journal of Cardiothoracic and Vascular Anesthesia 2007;21(1):68-75. [PMID: ] - PubMed
Yilmaz 1999 {published data only}
-
- Yilmaz M, Ener S, Akalin H, Sagdic K, Serdar OA, Cengiz M. Effect of low-dose methyl prednisolone on serum cytokine levels following extracorporeal circulation. Perfusion 1999;14(3):201-6. [PMID: ] - PubMed
References to studies excluded from this review
Anic 2004 {published data only}
-
- Anic D, Gašparovic H, Ivanèan H, Batinic D. Effects of corticosteroids on inflammatory response following cardiopulmonary bypass. Croatian Medical Journal 2004;45:158-61. [RESEARCHGATE: www.researchgate.net/profile/Drago-Batinic-2/publication/8600654_Effects... - PubMed
Biagioli 1981 {published data only}
-
- Biagioli B, Rossi C, Giomarelli PP, Pescatori G, Barbini P, Grossi A. Correlations between membrane and bubble oxygenators in patients treated with or without methylprednisolone. Haemodynamic and metabolic parameters. Giornale Italiano di Cardiologia 1981;11(9):1288-300. [PMID: ] - PubMed
Boldt 1986 {published data only}
-
- Boldt J, Bormann B, Kling D, Jooss D, Moosdorf R, Hempelmann G. Effect of glucocorticoids on extravascular lung water following extra-corporeal circulation. Anaesthesist 1986;35(4):238-44. [PMID: ] - PubMed
Jansen 1991b {published data only}
-
- Jansen NJ, Oeveren W, Vliet M, Stoutenbeek CP, Eysman L, Wildevuur CR. The role of different types of corticosteroids on the inflammatory mediators in cardiopulmonary bypass. European Journal of Cardio-thoracic Surgery 1991;5(4):211-7. [PMID: ] - PubMed
Jorens 1993 {published data only}
-
- Jorens PG, De Jongh R, De Backer W, Van Damme J, Van Overveld F, Bossaert L, et al. Interleukin-8 production in patients undergoing cardiopulmonary bypass. The influence of pretreatment with methylprednisolone. American Review of Respiratory Disease 1993;148(4 Pt 1):890-5. [PMID: ] - PubMed
Karlstad 1993 {published data only}
-
- Karlstad MD, Patteson SK, Guszcza JA, Langdon R, Chesney JT. Methylprednisolone does not influence endotoxin translocation during cardiopulmonary bypass. Journal of Cardiothoracic and Vascular Anesthesia 1993;7(1):23-7. [PMID: ] - PubMed
Kawamura 1995 {published data only}
-
- Kawamura T, Inada K, Okada H, Okada K, Wakusawa R. Methylprednisolone inhibits increase of interleukin 8 and 6 during open heart surgery. Canadian Journal of Anaesthesia 1995;42(5 pt 1):399-403. [PMID: ] - PubMed
Kawamura 1999 {published data only}
-
- Kawamura T, Inada K, Nara N, Wakusawa R, Endo S. Influence of methylprednisolone on cytokine balance during cardiac surgery. Critical Care Medicine 1999;27(3):545-8. [PMID: ] - PubMed
Kirsh 1979 {published data only}
-
- Kirsh MM, Behrendt DM, Jochim KE. Effects of methylprednisolone in cardioplegic solution during coronary bypass grafting. Journal of Thoracic and Cardiovascular Surgery 1979;77(6):896-9. [PMID: ] - PubMed
Kito 1980 {published data only}
-
- Kito Y, Fujita T, Naito Y, Koyanagi H, Obara K, Kosakai Y, et al. The effects of methylprednisolone on myocardial protection during open heart surgery. Kyobu Geka 1980;33(8):587-91. [PMID: ] - PubMed
Kobayashi 1996 {published data only}
-
- Kobayashi N. The circulatory and respiratory effects of methylprednisolone associated with catecholamine undergoing open heart surgery. Tokyo Joshi Ikadaigaku Zasshi 1996;66:1-10. [PMID: ] - PubMed
Launo 1990 {published data only}
-
- Launo C, Palermo S, Gobbi GC, Fumagalli C, Federici E, Moroni G. Methylprednisolone sodium succinate in the profile of respiratory complications after thoracic surgical intervention. Minerva Anestesiologica 1990;56(6):219-23. [PMID: ] - PubMed
Lee 2005 {published data only}
-
- Lee HS, Lee JM, Kim MS, Kim HY, Hwangbo B, Zo JI. Low-dose steroid therapy at an early phase of postoperative acute respiratory distress syndrome. Annals of Thoracic Surgery 2005;79:405-10. [PMID: ] - PubMed
Levinsky 1979 {published data only}
Loubser 1997 {published data only}
-
- Loubser PG. Effect of methylprednisolone on complement activation during heparin neutralization. Journal of Cardiovascular Pharmacology 1997;29(1):23-7. [PMID: ] - PubMed
Ming 2001 {published data only}
-
- Ming W, Yun-Bi L, Bo Y, Shi-Wei X, Ru-Kun C, Han-Liang Z. Effects of methylprednisolone and aprotinin on phospholipase D activity of leukocytes in systemic inflammatory response induced by cardiopulmonary bypass. Acta Pharmacologica Sinica 2001;22:913-17. [PMID: ] - PubMed
Miranda 1982 {published data only}
-
- Miranda DR, Stoutenbeek C, Karliczek G, Rating W. Effects of dexamethason on the early postoperative course after coronary artery bypass surgery. Thoracic & Cardiovascular Surgeon 1982;30(1):21-7. [PMID: ] - PubMed
Raff 1987 {published data only}
-
- Raff H, Norton AJ, Flemma RJ, Findling JW. Inhibition of the adrenocorticotropin response to surgery in humans: interaction between dexamethasone and fentanyl. Journal of Clinical Endocrinology and Metabolism 1987;65(2):295-8. [PMID: ] - PubMed
Ranucci 1994 {published data only}
-
- Ranucci M, Pavesi M, Conti D, Soro G, Ceocopieri M, Ghanem G, et al. High-dose steroids during cardiopulmonary bypass: comparison between two therapeutic approaches. Journal of Cardiothoracic and Vascular Anesthesia 1994;8(3 Suppl 2):134. [DOI: 10.1016/1053-0770(94)90537-1] - DOI
Santarpino 2009a {published data only}
-
- Santarpino G, Caroleo S, Onorati F, Rubino AD, Dardano A, Gulletta E, et al. Inflammatory response after cardiopulmonary bypass: a randomized comparison between conventional hemofiltration and steroids. Journal of Cardiovascular Surgery 2009;50(4):555-64. [PMID: ] - PubMed
Santarpino 2009b {published data only}
-
- Santarpino G, Caroleo S, Onorati F, Dimastromatteo G, Abdalla K, Amantea B, et al. Inflammatory response to cardiopulmonary bypass with enoximone or steroids in patients undergoing myocardial revascularization: a preliminary report study. International Journal of Clinical Pharmacology and Therapeutics 2009;47(2):78-88. [PMID: ] - PubMed
Schmartz 1996 {published data only}
-
- Schmartz D, Tabardel Y, Duchateau J, Barvais L, Hollander A. Corticosteroid effects on cytokine production in cardiac surgery: dose-effect relationship. British Journal of Anaesthesia 1996;76(Suppl 1):53. [ABSTRACT NUMBER: A167]
Tabardel 1996 {published data only}
-
- Taberdel Y, Duchateau J, Schmartz D, Marecaux G, Shahla M, Barvais L, et al. Corticosteroids increase blood interleukin-10 levels during cardiopulmonary bypass in men. Surgery 1996;119:76-80. [PMID: ] - PubMed
Thompson 1980 {published data only}
-
- Thompson MA, Broadbent MP. Methylprednisolone prior to cardiopulmonary bypass. Anaesthesia 1980;35(4):345-53. [PMID: ] - PubMed
Thompson 1982 {published data only}
-
- Thompson MA, Broadbent MP, English J. Plasma levels of methylprednisolone following administration during cardiac surgery. Anaesthesia 1982;37(4):405-7. [PMID: ] - PubMed
Toledo‐Pereyra 1980 {published data only}
-
- Toledo-Pereyra LH, Lin CY, Kundler H, Replogle RL. Steroids in heart surgery: a clinical double-blind and randomized study. American Surgeon 1980;46(3):155-60. [PMID: ] - PubMed
Turkoz 2000 {published data only}
-
- Turkoz A, Cigli A, But K, Sezgin N, Turkoz R, Gulcan O, et al. The effect of aprotinin and methylprednisolone during coronary artery surgery induced cytokines. Türk Anesteziyoloji ve Reanimasyon Cemiyeti Mecmuasi 2000;28:247-54. [PMID: ] - PubMed
Us 2001 {published data only}
-
- Us MH, Ege T, Cakir O, Ozkan S, Duran E, Ozturk OY. Effect of methylprednisolone in post-pump syndrome. Gulhane Tip Dergisi 2001;43(2):197-203. [CENTRAL: https://www.cochranelibrary.com/central/doi/10.1002/central/CN-00442345/...]
Vallejo 1977 {published data only}
-
- Vallejo JL, Gemenez-Fernandez R, Mainer JL, Rivera R. Clinical analysis of the protective effect of methylprednisolone on the heart in anoxic arrest (random study). Revista Espanola de Cardiologia 1977;30:705-9. [PMID: ] - PubMed
Van Overveld 1994 {published data only}
-
- Van Overveld FJ, De Jongh RF, Jorens PG, Walter P, Bossaert L, De Backer WA. Pretreatment with methylprednisolone in coronary artery bypass grafting influences the levels of histamine and tryptase in serum but not in bronchoalveolar lavage fluid. Clinical Science 1994;86(1):49-53. [DOI: 10.1042/cs0860049] - DOI - PubMed
Vogelzang 2007 {published data only}
Wan 1997b {published data only}
-
- Wan S, LeClerc JL, Schmartz D, Barvais L, Huynh CH, Deviere J, et al. Hepatic release of interleukin-10 during cardiopulmonary bypass in steroid-pretreated patients. American Heart Journal 1997;133(3):335-9. [PMID: ] - PubMed
Yaeger 2005 {published data only}
-
- Yeager MP, Rassias AJ, Fillinger MP, DiScipio AW, Gloor KE, Gregory JA, et al. Cortisol antiinflammatory effects are maximal at postoperative plasma concentrations. Critical Care Medicine 2005;33:1507-12. [PMID: ] - PubMed
Yasuura 1977 {published data only}
-
- Yasuura K, Nishitani Y, Tanimoto K, Hashimoto A, Hayashi H. Administration of steroid during open-heart surgery. Nippon Kyobu Geka Gakkai Zasshi 1977;25(12):1587-91. [PMID: ] - PubMed
References to ongoing studies
DECS‐II {published data only}
NCT00807521 {published data only}
-
- NCT00807521. Steroid-induced Reduction of Surgical Stress Study (STRESS) [Reduction of the cardiac proapoptotic stress response by dexamethasone in patients undergoing coronary artery bypass grafting]. clinicaltrials.gov/ct2/show/NCT00807521 (first received 12 December 2008).
NCT00879931 {unpublished data only}
-
- NCT00879931. Influence of corticoids on renal function in cardiac surgery. clinicaltrials.gov/ct2/show/NCT00879931 (first received 13 April 2009).
Additional references
Abbasciano 2021
-
- Abbasciano RG, Lai FY, Roman MA, Rizzello A, Pathak S, Ramzi J, et al. Activation of the innate immune response and organ injury after cardiac surgery: a systematic review and meta-analysis of randomised trials and analysis of individual patient data from randomised and non-randomised studies. British Journal of Anaesthesia 2021;127(3):365-75. [PMID: ] - PubMed
Alba 2016
-
- Alba AC, Alexander PE, Chang J, MacIsaac J, DeFry S, Guyatt GH. High statistical heterogeneity is more frequent in meta-analysis of continuous than binary outcomes. Journal of clinical epidemiology 2016 Feb 1;70:129-35. [PMID: ] - PubMed
Barnes 2006
Chaney 2002
-
- Chaney MA. Corticosteroids and cardiopulmonary bypass: a review of clinical investigations. Chest 2002;121(3):921-31. [PMID: ] - PubMed
Deeks 2023
-
- Deeks JJ, Higgins JPT, Altman DG, editor(s). Chapter 10: Analysing data and undertaking meta-analyses. In: Higgins JP, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, Welch VA, editor(s). Cochrane Handbook for Systematic Reviews of Interventions Version 6.4 (updated August 2023). Cochrane, 2023. Available from www.training.cochrane.org/handbook.
Devereaux 2022
Dieleman 2016
-
- Dieleman JM, Van Dijk D. Corticosteroids for cardiac surgery: a summary of two large randomised trials. Netherlands Journal of Critical Care 2016;24(5):6-10. [CORPUS ID: 53074542]
Dieleman 2017
-
- Dieleman JM, Wit GA, Nierich AP, Rosseel PM, Maaten JM, Hofland J, et al. Long‐term outcomes and cost effectiveness of high‐dose dexamethasone for cardiac surgery: a randomised trial. Anaesthesia 2017;72(6):704-13. [PMID: ] - PubMed
Dvirnik 2018
-
- Dvirnik N, Belley-Cote EP, Hanif H, Devereaux PJ, Lamy A, Dieleman JM, et al. Steroids in cardiac surgery: a systematic review and meta-analysis. British Journal of Anaesthesia 2018;120(4):657-67. [PMID: ] - PubMed
Egger 1997
Engelman 2019
-
- Engelman DT, Ali WB, Williams JB, Perrault LP, Reddy VS, Arora RC, et al. Guidelines for perioperative care in cardiac surgery: enhanced recovery after surgery society recommendations. JAMA Surgery 2019;154(8):755-66. [PMID: ] - PubMed
Gillinov 2016
Gregory 2021
-
- Gregory AJ, Arora RC, Chatterjee S, Grant MC, Lobdell KW, Morton V, et al. Selecting elements for a cardiac enhanced recovery protocol. Journal of cardiothoracic and vascular anesthesia 2021;35(12):3847-8. [PMID: ] - PubMed
Guyatt 2011
-
- Guyatt GH, Oxman AD, Schünemann HJ, Tugwell P, Knottnerus A. GRADE guidelines: a new series of articles in the Journal of Clinical Epidemiology. Journal of Clinical Epidemiology 2011 ;64(4):380-2. [PMID: ] - PubMed
Herdman 2011
Higgins 2011
-
- Higgins JP, Altman DG, Sterne JA, editor(s). Chapter 8: Assessing risk of bias in included studies. In: Higgins JP, Green S, editor(s). Cochrane Handbook for Systematic Reviews of Interventions Version 5.1.0 (updated March 2011). The Cochrane Collaboration, 2011. Available from training.cochrane.org/handbook/archive/v5.1/. [PMID: ] - PubMed
Higgins 2023a
-
- Higgins JP, Eldridge S, Li T (editors). Chapter 23: Including variants on randomized trials. In: Higgins JP, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, Welch VA (editors). Cochrane Handbook for Systematic Reviews of Interventions version 6.4 (updated August 2023). Cochrane, 2023. Available from www.training.cochrane.org/handbook.
Higgins 2023b
-
- Higgins JP, Savović J, Page MJ, Elbers RG, Sterne JAC. Chapter 8: Assessing risk of bias in a randomized trial. In: Higgins JP, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, Welch VA, editor(s). Cochrane Handbook for Systematic Reviews of Interventions Version 6.4 (updated August 2023). Cochrane, 2023. Available from www.training.cochrane.org/handbook.
Higgins 2023c
-
- Higgins JP, Li T, Deeks JJ, editor(s). Chapter 6: Choosing effect measures and computing estimates of effect. In: Higgins JP, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, Welch VA, editor(s). Cochrane Handbook for Systematic Reviews of Interventions Version 6.4 (updated August 2023). Cochrane, 2023. Available from www.training.cochrane.org/handbook.
Hill 1998
-
- Hill GE. Cardiopulmonary bypass-induced inflammation: is it important? Journal of Cardiothoracic & Vascular Anesthesia 1998;12(2 Suppl 1):21-5. [PMID: ] - PubMed
Katzung 2014
-
- Katzung B, Trevor A. Adrenocorticosteroids and adrenocortical antagonists. In: Basic and Clinical Pharmacology. 13th edition. New York (NY): McGraw-Hill, 2014:686. [GOOGLE SCHOLAR URL: scholar.google.com/scholar?q=Basic+%26+Clinical+Pharmacology,+Thirteenth...
Kirklin 1983
-
- Kirklin JK, Westaby S, Blackstone EH, Kirklin JW, Chenowerh DE, Pacifico AD. Complement and damaging effects of cardiopulmonary bypass. Journal of Thoracic & Cardiovascular Surgery 1983;86(6):845-57. [PMID: ] - PubMed
Lefebvre 2021
-
- Lefebvre C, Glanville J, Briscoe S, Littlewood A, Marshall C, Metzendorf M-I, et al. Chapter 4: Searching for and selecting studies. In: Higgins JP, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, Welch VA, editor(s). Cochrane Handbook for Systematic Reviews of Interventions Version 6.2 (updated February 2021). Cochrane, 2021. Available from training.cochrane.org/handbook . [PMID: ] - PubMed
Liberati 2009
Murphy 2004
-
- Murphy GJ, Angelini GD. Side effects of cardiopulmonary bypass: what is the reality? Journal of Cardiac Surgery 2004;19(6):481-8. [PMID: ] - PubMed
Ng 2020
-
- Ng KT, Van Paassen J, Langan C, Sarode DP, Arbous MS, Alston RP, et al. The efficacy and safety of prophylactic corticosteroids for the prevention of adverse outcomes in patients undergoing heart surgery using cardiopulmonary bypass: a systematic review and meta-analysis of randomized controlled trials. European Journal of Cardio-Thoracic Surgery 2020;57(4):620-7. [PMID: ] - PubMed
Page 2023
-
- Page MJ, Higgins JP, Sterne JAC. Chapter 13: Assessing risk of bias due to missing results in a synthesis. In: Higgins JP, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, Welch VA, editor(s). Cochrane Handbook for Systematic Reviews of Interventions Version 6.4 (updated August 2023). Cochrane, 2023. Available from www.training.cochrane.org/handbook.
Plot Digitizer [Computer program]
-
- Plot Digitizer. Version 2.6.8. Joseph A. Huwaldt, 27 October 2015. Available at plotdigitizer.sourceforge.net/History.html.
Quatrini 2021
R [Computer program]
-
- R. Version 4.0. Vienna, Austria: R Foundation for Statistical Computing, 2022. Available at cran.r-project.org.
RECOVERY 2020
RevMan 2023 [Computer program]
-
- Review Manager (RevMan). Version 6.1.0. The Cochrane Collaboration, 2023. Available at revman.cochrane.org.
Schünemann 2023
-
- Schünemann HJ, Higgins JP, Vist GE, Glasziou P, Akl EA, Skoetz N, et al. Chapter 14: Completing ‘Summary of findings’ tables and grading the certainty of the evidence. In: Higgins JP, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, Welch VA, editor(s). Cochrane Handbook for Systematic Reviews of Interventions Version 6.4 (updated August 2023). Cochrane, 2023. Available from www.training.cochrane.org/handbook.
Sousa‐Uva 2017
-
- Sousa-Uva M, Head SJ, Milojevic M, Collet JP, Landoni G, Castella M, et al. 2017 EACTS Guidelines on perioperative medication in adult cardiac surgery. European Journal of Cardio-Thoracic Surgery 2018;53(1):5-33. [PMID: ] - PubMed
Steroid Conversion Calculator
-
- Steroid Conversion Calculator. mdcalc.com. [URL: www.mdcalc.com/calc/2040/steroid-conversion-calculator]
Veervort 2020
-
- Vervoort D, Meuris B, Meyns B, Verbrugghe P. Global cardiac surgery: access to cardiac surgical care around the world. Journal of Thoracic and Cardiovascular Surgery 2020;159(3):987-96. [PMID: ] - PubMed
Viechtbauer 2010
-
- Viechtbauer W. Conducting meta-analyses in R with the metafor package. Journal of Statistical Software 2010;36(3):1-48. [DOI: 10.18637/jss.v036.i03] - DOI
Wahba 2019
-
- Wahba A, Milojevic M, Boer C, De Somer FM, Gudbjartsson T, den Goor J, et al. EACTS/EACTA/EBCP guidelines on cardiopulmonary bypass in adult cardiac surgery. European Journal of Cardio-Thoracic Surgery 2020 ;57(2):210-51. [PMID: ] - PubMed
Wan 1997a
-
- Wan S, LeClerc JL, Vincent JL. Inflammatory response to cardiopulmonary bypass: mechanisms involved and possible therapeutic strategies. Chest 1997;112(3):676-92. [PMID: ] - PubMed
Warltier 2002
-
- Warltier DC, Laffey JG, Boylan JF, Cheng DC. The systemic inflammatory response to cardiac surgery: implications for the anesthesiologist. Journal of the American Society of Anesthesiologists 2002 ;97(1):215-52. [PMID: ] - PubMed
Whitlock 2008
-
- Whitlock RP, Chan S, Devereaux PJ, Sun J, Rubens FD, Thorlund K, et al. Clinical benefit of steroids use in patients undergoing cardiopulmonary bypass: a meta-analysis of randomized trials. European Heart Journal 2008;29:2592-600. [PMID: ] - PubMed
Whitlock 2020
-
- Whitlock RP, Dieleman JM, Belley-Cote E, Vincent J, Zhang M, Devereaux PJ, et al. The effect of steroids in patients undergoing cardiopulmonary bypass: an individual patient meta-analysis of two randomized trials. Journal of Cardiothoracic and Vascular Anesthesia 2020 Jan 1;34(1):99-105. [PMID: ] - PubMed
Zacharias 2005
-
- Zacharias A, Schwann TA, Riordan CJ, Durham SJ, Shah AS, Habib RH. Obesity and risk of new-onset atrial fibrillation after cardiac surgery. Circulation 2005 ;112(21):3247-55. [PMID: ] - PubMed
References to other published versions of this review
Dieleman 2010
Publication types
MeSH terms
Substances
Associated data
LinkOut - more resources
Full Text Sources
Medical

