Impact of preoperative carbohydrate loading on postoperative course and morbidity in debulking surgery for epithelial ovarian cancer
- PMID: 38515650
- PMCID: PMC10952341
- DOI: 10.3892/etm.2024.12469
Impact of preoperative carbohydrate loading on postoperative course and morbidity in debulking surgery for epithelial ovarian cancer
Abstract
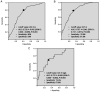
Despite the theoretical benefits, the favorable effect of preoperative carbohydrate loading on postoperative morbidity remains controversial. Most of the outcomes reported in the literature are derived from non-gynecologic surgery data, with only one study involving a limited number of patients specifically in gynecological oncology. The present study aimed to investigate the impact of carbohydrate loading, as a single element of enhanced recovery after surgery protocols, on postoperative course and morbidity in patients undergoing debulking surgery for epithelial ovarian cancer (EOC). The present study was a non-randomized, prospective cohort trial enrolling patients with EOC who underwent surgery between June 2018 and December 2021. An oral carbohydrate supplement with a dose of 50 g was given to patients 2-3 h before anesthesia. Data on postoperative course and morbidity were collected and compared with data of a historical cohort including consecutive patients who underwent surgery without a carbohydrate loading between January 2015 and June 2018. Analyses were performed on a total of 162 patients, including 72 patients in the carbohydrate loading group and 90 patients in the control group. Median length of hospital stay (11 days vs. 11 days; P=0.555), postoperative days 1-7 serum c-reactive protein levels (P=0.213), 30-day readmission (11.6% vs. 11.5%, P=0.985), 30-day relaparotomy (2.8% vs. 3.4%, P=0.809) and 30-day morbidity (48.6% vs. 46.7%; P=0.805) were comparable between the cohorts. No significant differences in grades of morbidities were identified between the cohorts (P=0.511). Multivariate analysis revealed that the sole independent risk factor for any postoperative morbidity was operative time. In conclusion, based on the results of the present study, postoperative course and morbidity seemed to be unaffected by carbohydrate loading in patients undergoing debulking surgery for EOC.
Keywords: carbohydrate loading; debulking surgery; epithelial ovarian cancer; morbidity.
Copyright: © 2024 Toptas et al.
Conflict of interest statement
The authors declare that they have no competing interests.
Figures
Similar articles
-
A Single Centre Randomised Control Study to Assess the Impact of Pre-Operative Carbohydrate Loading on Women Undergoing Major Surgery for Epithelial Ovarian Cancer.Cureus. 2020 Aug 31;12(8):e10169. doi: 10.7759/cureus.10169. Cureus. 2020. PMID: 33014663 Free PMC article.
-
Impact of Enhanced Recovery after Surgery with Preoperative Whey Protein-Infused Carbohydrate Loading and Postoperative Early Oral Feeding among Surgical Gynecologic Cancer Patients: An Open-Labelled Randomized Controlled Trial.Nutrients. 2020 Jan 20;12(1):264. doi: 10.3390/nu12010264. Nutrients. 2020. PMID: 31968595 Free PMC article. Clinical Trial.
-
A Full Enhanced Recovery after Surgery Program in Gynecologic Laparoscopic Procedures: A Randomized Controlled Trial.J Minim Invasive Gynecol. 2021 Sep;28(9):1610-1617.e6. doi: 10.1016/j.jmig.2021.01.024. Epub 2021 Mar 4. J Minim Invasive Gynecol. 2021. PMID: 33676007 Clinical Trial.
-
Perioperative carbohydrate loading in patients undergoing one-day surgery. A systematic review of randomized controlled trials.Wideochir Inne Tech Maloinwazyjne. 2022 Sep;17(3):457-466. doi: 10.5114/wiitm.2022.116750. Epub 2022 Jun 19. Wideochir Inne Tech Maloinwazyjne. 2022. PMID: 36187066 Free PMC article. Review.
-
Primary debulking surgery vs. interval debulking surgery for advanced ovarian cancer: review of the literature and meta-analysis.Minerva Med. 2019 Aug;110(4):330-340. doi: 10.23736/S0026-4806.19.06078-6. Epub 2019 May 6. Minerva Med. 2019. PMID: 31081304 Review.
References
LinkOut - more resources
Full Text Sources
Research Materials
