Overt Hypothyroidism and Severe Growth Retardation in a Preschool Girl with Poorly Controlled Nephrotic Syndrome: Case Report and Literature Review
- PMID: 38516512
- PMCID: PMC10952417
- DOI: 10.15388/Amed.2023.30.2.4
Overt Hypothyroidism and Severe Growth Retardation in a Preschool Girl with Poorly Controlled Nephrotic Syndrome: Case Report and Literature Review
Abstract
Background: Nephrotic children may develop thyroid hormone dysfunction due to urinary excretion of thyroid hormones. In contrast to the subclinical hypothyroidism that affects around 30% of children with nephrotic syndrome (NS), the patient in this case had overt hypothyroidism and severe growth retardation.
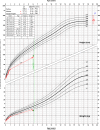
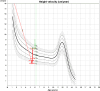
Clinical case: A 5 years and 8 months old girl with steroid-dependent NS was referred from another center due to persistent edema and decreased diuresis, being treated with mycophenolate mofetil (MMF) 250 mg once a day and L-thyroxine 50 mcg daily since 4 months of NS onset because of hypothyroidism. Her albumin was 12.64 g/l, cholesterol 25.64 mmol/l and proteinuria 5 g/l. Severe growth retardation was observed: patient's height was 93.5 cm (-13 cm <3 percentile), weighted 17.2 kg (15-25 percentile). Her disease vintage was over 3 years. Girl's growth velocity has slowed down from 3.5 months. The patient received a high cumulative dose of prednisolone (approx. 7800 mg in 1 year and 8 months). Thyroid-stimulating hormone was higher (18.04 mU/L) with reduced FT4 11.43 pmol/l and IGF-1 < 15 µg/L. Kidney biopsy revealed minimal change disease, and genetic testing was negative. Intensive NS treatment with methylprednisolone pulse therapy, enlarged doses of MMF and albumin infusion were started and L-thyroxine dose was increased to 75 mcg. TPOAb was in normal range (12.65 IU/ml). After 3 weeks she was discharged with no edema and after stopping methylprednisolone treatment thyroid function normalized and L-thyroxin was discontinued. Two weeks later standard growth hormone stimulation test with clonidine showed partially insufficient growth hormone secretion. During NS remission with normalization of thyroid function (TSH 6.680 mU/l, FT4 13.85 pmol/l) and normalization of IGF-1 level (132 mcg/l) partial catch-up growth was observed (height velocity increased from 3.5 cm/year to 7.3 cm/year, based on 4-month calculation period).
Conclusions: Clinicians should be aware of a risk of developing hypothyroidism and consider thyroid function testing during the treatment of children with NS, as well as actively treat hypothyroidism and evaluate growth.
Apžvalga: Vaikams, sergantiems nefroziniu sindromu (NS), gali sutrikti skydliaukės funkcija dėl skydliaukės hormonᶙ netekimo su šlapimu. Skirtingai nuo subklinikinės hipotirozės, kuri nustatoma apie 30 % vaikᶙ, sergančiᶙ NS, šiuo atveju pacientei nustatyta kliniškai reikšminga hipotirozė ir ryškus augimo sulėtėjimas.
Klinikinis atvejis: 5 metᶙ ir 8 mėnesiᶙ pacientė, kuriai prieš trejus metus diagnozuotas nuo steroidᶙ priklausomas NS, buvo atsiᶙsta iš kito centro dėl išliekančiᶙ edemᶙ ir sumažėjusios diurezės. Pacientė buvo gydoma mikofenolato mofetiliu (MMF) 250 mg 1 k/d. ir L-tiroksinu 50 mcg 1 k/d., nes praėjus 4 mėnesiams nuo NS pradžios jai buvo diagnozuotas hipotiroidizmas. Atvykus albuminas buvo 12,64 g/l, cholesterolis 25,64 mmol/l ir proteinurija 5 g/l. Hospitalizacijos metu taip pat buvo ryškus augimo atsilikimas: pacientės ūgis buvo 93,5 cm (-13 cm < 3 procentilio), svoris 17,2 kg (15–25 procentilio). Mergaitės ūgio atsilikimas pastebėtas nuo 3,5 mėnesio amžiaus. Ji yra gavusi didelę suminę prednizolono dozę (apie 7800 mg per vienus metus ir 8 mėnesius). Hospitalizuojant skydliaukę stimuliuojantis hormonas (TTH/TSH) buvo padidėjęs (18,04 mU/L), o sumažėję FT4 (11,43 pmol/l) ir IGF-1 < 15 µg/L. Atlikus inkstᶙ biopsiją nustatyta minimaliᶙ pokyčiᶙ liga, o genetiniu ištyrimu pokyčiᶙ nerasta. Pacientė dėl NS pradėta intensyviai gydyti metilprednizolono pulsine terapija, padidinta MMF dozė, taip pat skirtos albumino infuzijos ir padidinta L-tiroksino dozė iki 75 mcg. Po 3 savaičiᶙ išnykus edemoms mergaitė išleista į namus, o remiantis dinamika nutrauktas gydymas metilprednizolonu, normalizavusis skydliaukės funkcijai nutrauktas ir L-tiroksino vartojimas. Praėjus 2 savaitėms atliktas standartinis augimo hormono stimuliacijos mėginys su klonidinu parodė iš dalies nepakankamą augimo hormono sekreciją. Pasiekus NS remisiją, kurios metu normalizavosi skydliaukės funkcija (TSH 6,680 mU/l, FT4 13,85 pmol/l) ir IGF-1 koncentracija (132 mcg/l), buvo matomas dalinis augimo greičio prisivijimas (augimo greitis padidėjo nuo 3,5 cm/m iki 7,3 cm/m, remiantis 4 mėnesiᶙ skaičiavimais).
Išvados: Gydytojams būtina žinoti hipotirozės išsivystymo riziką ir apsvarstyti skydliaukės funkcijos tyrimᶙ skyrimo vaikams, sergantiems NS, būtinumą bei aktyviai gydyti hipotirozę ir stebėti vaikᶙ augimo greitį.
Keywords: Hypothyroidism; children; growth retardation; nephrotic syndrome.
Copyright © 2023 Joana Mikulevič, Karolina Tumelienė, Robertas Kemežys, Augustina Jankauskienė. Published by Vilnius University Press.
Figures
Similar articles
-
A case of minimal change nephrotic syndrome with hypothyroidism deterioration.CEN Case Rep. 2016 May;5(1):95-98. doi: 10.1007/s13730-015-0201-2. Epub 2015 Oct 26. CEN Case Rep. 2016. PMID: 28509173 Free PMC article.
-
Hypothyroidism among children and adolescents with nephrotic syndrome in Mulago National Referral Hospital, Kampala, Uganda; a cross-sectional study.BMC Pediatr. 2024 Feb 19;24(1):132. doi: 10.1186/s12887-024-04610-8. BMC Pediatr. 2024. PMID: 38373933 Free PMC article.
-
Endemic infantile hypothyroidism in a severe endemic goitre area of central Africa.Clin Endocrinol (Oxf). 1984 Mar;20(3):327-40. doi: 10.1111/j.1365-2265.1984.tb00089.x. Clin Endocrinol (Oxf). 1984. PMID: 6723080
-
Hypothyroidism and Nephrotic Syndrome: Why, When and How to Treat.Curr Vasc Pharmacol. 2017;15(5):398-403. doi: 10.2174/1570161115999170207114706. Curr Vasc Pharmacol. 2017. PMID: 28176633 Review.
-
Overt and subclinical hypothyroidism: who to treat and how.Drugs. 2012 Jan 1;72(1):17-33. doi: 10.2165/11598070-000000000-00000. Drugs. 2012. PMID: 22191793 Review.
References
-
- Noone DG, Iijima K, Parekh R. Idiopathic nephrotic syndrome in children. Lancet. 2018;392(10141):61–74. - PubMed
-
- Leung AM, Brent GA. The Influence of Thyroid Hormone on Growth Hormone Secretion and Action. In: Cohen L, editor. Growth Hormone Deficiency. Cham: Springer; 2016. pp. 29–46. - DOI
-
- Hajizadeh N, Marashi SM, Nabavizadeh B, Elhami E, Mohammadi T, Nobandegani NM, et al. Examine of thyroid function in pediatric nephrotic syndrome: Tehran-Iran. Int J Pediatr. 2015;3:59–65. doi: 10.22038/IJP.2015.4051. - DOI
Publication types
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous