Germinoma of basal ganglia
- PMID: 38523694
- PMCID: PMC10958132
- DOI: 10.1016/j.radcr.2024.02.047
Germinoma of basal ganglia
Abstract
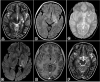
Basal ganglia germinomas (BGGs) are rare lesions. Because of the atypical features of early-stage clinical symptoms and imaging characteristics, BGGs are easily misdiagnosed with non-tumorous conditions. This article presented cases of 2 young male patients who came to the hospital due to right arm weakness. Brain Magnetic Resonance Imaging (MRI) images in the first case revealed a lobulated mixed component mass on the left basal ganglia. The solid part showed restricted diffusion on diffusion-weighted imaging, heterogeneous strong enhancement, and no signal of calcification or bleeding. The second case in the left putamen showed hypointensity on T2*, mild enhancement, and atrophy of the ipsilateral cerebral peduncle, increased choline, and decreased n-acetyl-aspartate (NAA) on spectroscopy. Follow-up MRI after 6 months showed a mass increase in size and hypointensity part on T2*. BGGs have been confirmed on biopsy in both cases. With isolated chemotherapy application, there is no sign of remission in the first patient. The second patient was treated with chemotherapy and radiotherapy, and MRI images after treatment showed a complete response.
Keywords: Basal ganglia; Germinoma; MRI.
© 2024 The Authors. Published by Elsevier Inc. on behalf of University of Washington.
Figures







References
-
- Kleinschmidt-DeMasters BK, Bette K, Tihan T. Diagnostic Pathology: Neuropathology E-Book. Elsevier Health Sciences; 2022.
Publication types
LinkOut - more resources
Full Text Sources

