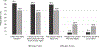Ninety Percent of Patients Are Satisfied With Their Decision to Undergo Spine Surgery for Degenerative Conditions
- PMID: 38533908
- PMCID: PMC11844801
- DOI: 10.1097/BRS.0000000000004714
Ninety Percent of Patients Are Satisfied With Their Decision to Undergo Spine Surgery for Degenerative Conditions
Abstract
Study design: Cross-sectional survey and retrospective review of prospectively collected data.
Objective: To explore how patients perceive their decision to pursue spine surgery for degenerative conditions and evaluate factors correlated with decisional regret.
Summary of background data: Prior research shows that one-in-five older adults regret their decision to undergo spinal deformity surgery. However, no studies have investigated decisional regret in patients with degenerative conditions.
Methods: Patients who underwent cervical or lumbar spine surgery for degenerative conditions (decompression, fusion, or disk replacement) between April 2017 and December 2020 were included. The Ottawa Decisional Regret Questionnaire was implemented to assess prevalence of decisional regret. Questionnaire scores were used to categorize patients into low (<40) or medium/high (≥40) decisional regret cohorts. Patient-reported outcome measures (PROMs) included the Oswestry Disability Index, Patient-reported Outcomes Measurement Information System, Visual Analog Scale (VAS) Back/Leg/Arm, and Neck Disability Index at preoperative, early postoperative (<6 mo), and late postoperative (≥6 mo) timepoints. Differences in demographics, operative variables, and PROMs between low and medium/high decisional regret groups were evaluated.
Results: A total of 295 patients were included (mean follow-up: 18.2 mo). Overall, 92% of patients agreed that having surgery was the right decision, and 90% would make the same decision again. In contrast, 6% of patients regretted the decision to undergo surgery, and 7% noted that surgery caused them harm. In-hospital complications (P=0.02) and revision fusion (P=0.026) were significantly associated with higher regret. The medium/high decisional regret group also exhibited significantly worse PROMs at long-term follow-up for all metrics except VAS-Arm, and worse achievement of minimum clinically important difference for Oswestry Disability Index (P=0.007), Patient-Reported Outcomes Measurement Information System (P<0.0001), and VAS-Leg (P<0.0001).
Conclusions: Higher decisional regret was encountered in the setting of need for revision fusion, increased in-hospital complications, and worse PROMs. However, 90% of patients overall were satisfied with their decision to undergo spine surgery for degenerative conditions. Current tools for assessing patient improvement postoperatively may not adequately capture the psychosocial values and patient expectations implicated in decisional regret.
Copyright © 2023 Wolters Kluwer Health, Inc. All rights reserved.
Conflict of interest statement
The authors report no conflicts of interest.
Figures
References
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous