Influence of Alcohol on Intracerebral Hemorrhage: From Oxidative Stress to Glial Cell Activation
- PMID: 38541637
- PMCID: PMC10971394
- DOI: 10.3390/life14030311
Influence of Alcohol on Intracerebral Hemorrhage: From Oxidative Stress to Glial Cell Activation
Abstract
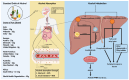
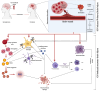
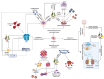
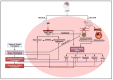
The intricate relationship between alcohol consumption and intracerebral hemorrhage (ICH) presents a nuanced field of study, especially concerning the dose-dependent impact on secondary brain injury (SBI). Recognizing the established risks associated with heavy drinking, this review delves deeper into the less understood territories of low to moderate alcohol consumption. By systematically analyzing recent studies, we uncover critical insights into how varying alcohol intake levels modulate ICH risk through mechanisms such as microglial activation, oxidative stress, and the protective potential of polyphenols. This analysis extends beyond the hypertensive effects of heavy alcohol use to explore the complex molecular pathophysiology involved in alcohol-related ICH. Our findings indicate that while heavy alcohol use unequivocally exacerbates ICH risk, moderate consumption and its associated polyphenols may offer neuroprotective effects against SBI, albeit within a finely balanced threshold. This review highlights the significant gaps in current understanding and underscores the urgent need for targeted research to elucidate these complex interactions. Through this comprehensive examination, we aim to inform more nuanced public health policies and intervention strategies, taking into account the diverse effects of alcohol consumption on ICH risk.
Keywords: alcohol consumption; alcohol intoxication; alcoholism; intracerebral hemorrhage.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
Similar articles
-
Alcohol use and risk of intracerebral hemorrhage.Neurology. 2017 May 23;88(21):2043-2051. doi: 10.1212/WNL.0000000000003952. Epub 2017 Apr 26. Neurology. 2017. PMID: 28446657 Free PMC article.
-
Cerebral Hemorrhage and Alcohol Exposure: A Review.Alcohol Alcohol. 2020 Feb 7;55(1):20-27. doi: 10.1093/alcalc/agz087. Alcohol Alcohol. 2020. PMID: 31845978 Review.
-
Heavy alcohol intake and intracerebral hemorrhage: characteristics and effect on outcome.Neurology. 2012 Sep 11;79(11):1109-15. doi: 10.1212/WNL.0b013e3182698d00. Neurology. 2012. PMID: 22965674
-
Microglial pyroptosis: Therapeutic target in secondary brain injury following intracerebral hemorrhage.Front Cell Neurosci. 2022 Sep 9;16:971469. doi: 10.3389/fncel.2022.971469. eCollection 2022. Front Cell Neurosci. 2022. PMID: 36159393 Free PMC article. Review.
-
Exploration of MST1-Mediated Secondary Brain Injury Induced by Intracerebral Hemorrhage in Rats via Hippo Signaling Pathway.Transl Stroke Res. 2019 Dec;10(6):729-743. doi: 10.1007/s12975-019-00702-1. Epub 2019 Apr 2. Transl Stroke Res. 2019. PMID: 30941717
Cited by
-
Impact of acute alcohol intoxication and alcohol dependence on outcomes after subarachnoid hemorrhage.Acta Neurochir (Wien). 2025 Aug 27;167(1):231. doi: 10.1007/s00701-025-06639-9. Acta Neurochir (Wien). 2025. PMID: 40864201 Free PMC article.
-
The relationship between hypomagnesemia and ICU mortality in severe hemorrhagic stroke patients: an observational multicentre study on eICU database.BMC Cardiovasc Disord. 2025 Feb 1;25(1):73. doi: 10.1186/s12872-025-04525-x. BMC Cardiovasc Disord. 2025. PMID: 39893408 Free PMC article.
References
-
- Rosso A.M. Beer and wine in antiquity: Beneficial remedy or punishment imposed by the Gods? Acta Med. Hist. Adriat. 2012;10:237–262. - PubMed
Publication types
Grants and funding
LinkOut - more resources
Full Text Sources

