Primary Cutaneous Melanoma-Management in 2024
- PMID: 38541831
- PMCID: PMC10971470
- DOI: 10.3390/jcm13061607
Primary Cutaneous Melanoma-Management in 2024
Abstract
Background: Maximizing survival for patients with primary cutaneous melanomas (melanomas) depends on an early diagnosis and appropriate management. Several new drugs have been shown to improve survival in high-risk melanoma patients. Despite well-documented guidelines, many patients do not receive optimal management, particularly when considering patient age. Objective: to provide an update on melanoma management from the time of the decision to biopsy a suspicious skin lesion. Methods: We reviewed melanoma-management research published between 2018 and 2023 and identified where such findings impact and update the management of confirmed melanomas. Pubmed, Google Scholar, Ovid and Cochrane Library were used as search tools. Results: We identified 81 publications since 2017 that have changed melanoma management; 11 in 2018, 12 in 2019, 10 in 2020, 12 in 2021, 17 in 2022 and 18 in 2023. Discussion: Delayed or inaccurate diagnosis is more likely to occur when a partial shave or punch biopsy is used to obtain the histopathology. Wherever feasible, a local excision with a narrow margin should be the biopsy method of choice for a suspected melanoma. The Breslow thickness of the melanoma remains the single most important predictor of outcome, followed by patient age and then ulceration. The BAUSSS biomarker, (Breslow thickness, Age, Ulceration, Subtype, Sex and Site) provides a more accurate method of determining mortality risk than older currently employed approaches, including sentinel lymph node biopsy. Patients with metastatic melanomas and/or nodal disease should be considered for adjuvant drug therapy (ADT). Further, high-risk melanoma patients are increasingly considered for ADT, even without disease spread. Invasive melanomas less than 1 mm thick are usually managed with a radial excision margin of 10 mms of normal skin. If the thickness is 1 to 2 mm, select a radial margin of 10 to 20 mm. When the Breslow thickness is over 2 mm, a 20 mm clinical margin is usually undertaken. In situ melanomas are usually managed with a 5 to 10 mm margin or Mohs margin control surgery. Such wide excisions around a given melanoma is the only surgery that can be regarded as therapeutic and required. Patients who have had one melanoma are at increased risk of another melanoma. Ideal ongoing management includes regular lifelong skin checks. Total body photography should be considered if the patient has many naevi, especially when atypical/dysplastic naevi are identified. Targeted approaches to improve occupational or lifestyle exposure to ultraviolet light are important. Management also needs to include the consideration of vitamin D supplementary therapy.
Keywords: BAUSSS; management; melanoma; treatment.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
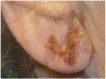
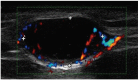

References
-
- Kok Y., Scott K., Pham A., Liu W., Roberts H., Pan Y., McLean C., Chamberlain A., Kelly J.W., Mar V.J. The impact of incomplete clinical information and initial biopsy technique on the histopathological diagnosis of cutaneous melanoma. Australas. J. Dermatol. 2021;62:e524–e531. doi: 10.1111/ajd.13697. - DOI - PubMed
LinkOut - more resources
Full Text Sources

