Strategies for Overcoming Immune Evasion in Bladder Cancer
- PMID: 38542078
- PMCID: PMC10970137
- DOI: 10.3390/ijms25063105
Strategies for Overcoming Immune Evasion in Bladder Cancer
Abstract
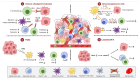
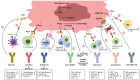
Tumors intricately shape a highly immunosuppressive microenvironment, hampering effective antitumor immune responses through diverse mechanisms. Consequently, achieving optimal efficacy in cancer immunotherapy necessitates the reorganization of the tumor microenvironment and restoration of immune responses. Bladder cancer, ranking as the second most prevalent malignant tumor of the urinary tract, presents a formidable challenge. Immunotherapeutic interventions including intravesical BCG and immune checkpoint inhibitors such as atezolizumab, avelumab, and pembrolizumab have been implemented. However, a substantial unmet need persists as a majority of bladder cancer patients across all stages do not respond adequately to immunotherapy. Bladder cancer establishes a microenvironment that can actively hinder an efficient anti-tumor immune response. A deeper understanding of immune evasion mechanisms in bladder cancer will aid in suppressing recurrence and identifying viable therapeutic targets. This review seeks to elucidate mechanisms of immune evasion specific to bladder cancer and explore novel pathways and molecular targets that might circumvent resistance to immunotherapy.
Keywords: bladder cancer; immune checkpoint inhibitor; immune evasion; immunoregulatory cell; tumor microenvironment.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
Similar articles
-
Mechanisms of immune evasion in bladder cancer.Cancer Immunol Immunother. 2020 Jan;69(1):3-14. doi: 10.1007/s00262-019-02443-4. Epub 2019 Dec 6. Cancer Immunol Immunother. 2020. PMID: 31811337 Free PMC article. Review.
-
Redefining bladder cancer treatment: innovations in overcoming drug resistance and immune evasion.Front Immunol. 2025 Jan 22;16:1537808. doi: 10.3389/fimmu.2025.1537808. eCollection 2025. Front Immunol. 2025. PMID: 39911393 Free PMC article. Review.
-
Bladder cancer, a unique model to understand cancer immunity and develop immunotherapy approaches.J Pathol. 2019 Oct;249(2):151-165. doi: 10.1002/path.5306. Epub 2019 Jun 24. J Pathol. 2019. PMID: 31102277 Free PMC article. Review.
-
Checkpoint inhibitors in BCG-unresponsive nonmuscle invasive bladder cancer: can they help spare the bladder?Immunotherapy. 2021 Sep;13(13):1105-1111. doi: 10.2217/imt-2021-0030. Epub 2021 Jun 29. Immunotherapy. 2021. PMID: 34184569 Review.
-
Rationale and Outcomes for Neoadjuvant Immunotherapy in Urothelial Carcinoma of the Bladder.Eur Urol Oncol. 2020 Dec;3(6):728-738. doi: 10.1016/j.euo.2020.06.009. Epub 2020 Nov 8. Eur Urol Oncol. 2020. PMID: 33177001
Cited by
-
HDL cholesterol esters mediate the genetic link between sedentary behavior and urological cancers: Insights from mediation and validation analyses.Medicine (Baltimore). 2025 May 2;104(18):e42369. doi: 10.1097/MD.0000000000042369. Medicine (Baltimore). 2025. PMID: 40324228 Free PMC article.
References
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

