Safety of low weight gain or weight loss in pregnancies with class 1, 2, and 3 obesity: a population-based cohort study
- PMID: 38555927
- PMCID: PMC11097195
- DOI: 10.1016/S0140-6736(24)00255-1
Safety of low weight gain or weight loss in pregnancies with class 1, 2, and 3 obesity: a population-based cohort study
Abstract
Background: There are concerns that current gestational weight gain recommendations for women with obesity are too high and that guidelines should differ on the basis of severity of obesity. In this study we investigated the safety of gestational weight gain below current recommendations or weight loss in pregnancies with obesity, and evaluated whether separate guidelines are needed for different obesity classes.
Methods: In this population-based cohort study, we used electronic medical records from the Stockholm-Gotland Perinatal Cohort study to identify pregnancies with obesity (early pregnancy BMI before 14 weeks' gestation ≥30 kg/m2) among singleton pregnancies that delivered between Jan 1, 2008, and Dec 31, 2015. The pregnancy records were linked with Swedish national health-care register data up to Dec 31, 2019. Gestational weight gain was calculated as the last measured weight before or at delivery minus early pregnancy weight (at <14 weeks' gestation), and standardised for gestational age into z-scores. We used Poisson regression to assess the association of gestational weight gain z-score with a composite outcome of: stillbirth, infant death, large for gestational age and small for gestational age at birth, preterm birth, unplanned caesarean delivery, gestational diabetes, pre-eclampsia, excess postpartum weight retention, and new-onset longer-term maternal cardiometabolic disease after pregnancy, weighted to account for event severity. We calculated rate ratios (RRs) for our composite adverse outcome along the weight gain z-score continuum, compared with a reference of the current lower limit for gestational weight gain recommended by the US Institute of Medicine (IOM; 5 kg at term). RRs were adjusted for confounding factors (maternal age, height, parity, early pregnancy BMI, early pregnancy smoking status, prepregnancy cardiovascular disease or diabetes, education, cohabitation status, and Nordic country of birth).
Findings: Our cohort comprised 15 760 pregnancies with obesity, followed up for a median of 7·9 years (IQR 5·8-9·4). 11 667 (74·0%) pregnancies had class 1 obesity, 3160 (20·1%) had class 2 obesity, and 933 (5·9%) had class 3 obesity. Among these pregnancies, 1623 (13·9%), 786 (24·9%), and 310 (33·2%), respectively, had weight gain during pregnancy below the lower limit of the IOM recommendation (5 kg). In pregnancies with class 1 or 2 obesity, gestational weight gain values below the lower limit of the IOM recommendation or weight loss did not increase risk of the adverse composite outcome (eg, at weight gain z-score -2·4, corresponding to 0 kg at 40 weeks: adjusted RR 0·97 [95% CI 0·89-1·06] in obesity class 1 and 0·96 [0·86-1·08] in obesity class 2). In pregnancies with class 3 obesity, weight gain values below the IOM limit or weight loss were associated with reduced risk of the adverse composite outcome (eg, adjusted RR 0·81 [0·71-0·89] at weight gain z-score -2·4, or 0 kg).
Interpretation: Our findings support calls to lower or remove the lower limit of current IOM recommendations for pregnant women with obesity, and suggest that separate guidelines for class 3 obesity might be warranted.
Funding: Karolinska Institutet and the Eunice Kennedy Shriver National Institute of Child Health and Human Development.
Copyright © 2024 Elsevier Ltd. All rights reserved.
Conflict of interest statement
Declaration of interests OS declares that he is the co-founder and co-owner of a Swedish pregnancy app, One Million Babies. KJ, LMB, and JAH are advising on a WHO initiative to create global pregnancy weight gain standards, for which KJ and JAH have received financial support for meeting attendance or travel, and JAH has received consulting fees. The views expressed in this study do not reflect the views of WHO. BA declares no competing interests.
Figures


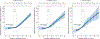
Comment in
-
Optimising gestational weight gain among pregnant women with obesity.Lancet. 2024 Apr 13;403(10435):1423-1425. doi: 10.1016/S0140-6736(24)00470-7. Epub 2024 Mar 28. Lancet. 2024. PMID: 38555926 No abstract available.
References
-
- Institute of Medicine (IOM). Weight gain during pregnancy: reexamining the guidelines. . Washington, DC National Research Council; 2009.
-
- American College of O, Gynecologists. ACOG Committee opinion no. 548: weight gain during pregnancy. Obstetrics and gynecology 2013. (Reaffirmed 2023); 121(1): 210–2. - PubMed
-
- Artal R, Lockwood CJ, Brown HL. Weight gain recommendations in pregnancy and the obesity epidemic. Obstetrics and gynecology 2010; 115(1): 152–5. - PubMed
Publication types
MeSH terms
Grants and funding
- U10 HL120006/HL/NHLBI NIH HHS/United States
- U10 HL119991/HL/NHLBI NIH HHS/United States
- U10 HD063072/HD/NICHD NIH HHS/United States
- U10 HL120018/HL/NHLBI NIH HHS/United States
- U10 HD063037/HD/NICHD NIH HHS/United States
- R01 HD094777/HD/NICHD NIH HHS/United States
- U10 HL119990/HL/NHLBI NIH HHS/United States
- U10 HL119993/HL/NHLBI NIH HHS/United States
- U10 HL119992/HL/NHLBI NIH HHS/United States
- U10 HD063053/HD/NICHD NIH HHS/United States
- U10 HL120034/HL/NHLBI NIH HHS/United States
- U10 HL120019/HL/NHLBI NIH HHS/United States
- U10 HD063036/HD/NICHD NIH HHS/United States
- U10 HL119989/HL/NHLBI NIH HHS/United States
- U10 HD063048/HD/NICHD NIH HHS/United States
- U10 HD063047/HD/NICHD NIH HHS/United States
- U10 HD063041/HD/NICHD NIH HHS/United States
- U10 HD063020/HD/NICHD NIH HHS/United States
LinkOut - more resources
Full Text Sources
Research Materials

