Laparoscopic-Assisted Transvaginal Cholecystectomy - the US Military Experience With Long-Term Follow Up
- PMID: 38562949
- PMCID: PMC10984372
- DOI: 10.4293/JSLS.2023.00059
Laparoscopic-Assisted Transvaginal Cholecystectomy - the US Military Experience With Long-Term Follow Up
Abstract
Objectives: We present our initial clinical experience applying Natural Orifice Transluminal Endoscopic Surgical (NOTES) technique to perform cholecystectomy in ten patients at a military institution.
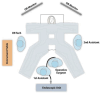
Methods: A posterior colpotomy was created to accommodate a single site working port used to facilitate dissection and gallbladder mobilization under direct visualization via an infraumbilical port. The specimen was retrieved through the vagina and the colpotomy was closed with absorbable suture under direct visualization. Long-term follow up was performed over the phone to assess quality of life with 2 widely used health-related quality of life (HRQoL) surveys including RAND-36 Health Item Survey (Version 1.0),1 and the Female Sexual Function Index (FSFI).2.
Results: Ten women underwent a laparoscopic-assisted transvaginal cholecystectomy (TVC) with 7 available for long-term follow-up. The average age was 28.9 years (20-37) and the indications for surgery included symptomatic cholelithiasis (9) and biliary dyskinesia (1). The mean operative time was 129 mins (95-180), and median blood loss was 34 ml (5-400). There were no conversions and the average length of stay was 9.98 hours (2.4-28.8). Pain (analogue scale 1-10) on postoperative day three was minimal (mean 2.3) and was limited to the infraumbilical incision. On average patients returned to work by postoperative day six and resumed normal daily activities at seven days. Immediate postoperative complications included one incident of postoperative urinary retention requiring bladder catheterization. One intra-operative cholangiogram was successfully performed due to elevated preoperative liver enzymes without significant findings. Long-term complications included one asymptomatic incisional hernia repair at the infraumbilical port site. The RAND-36 survey demonstrated an average physical and mental health summary score of 82.2 and 63.7 with an average general health score of 63.6. The average FSFI total score was 21.8.
Conclusion: TVC is safe and effective. Implementation may improve operational readiness by returning service members to normal activities more expeditiously than conventional laparoscopy.
Keywords: Endoscopic surgery; NOTES; Natural orifice transluminal endoscopic surgery; Transvaginal cholecystectomy.
© 2024 by SLS, Society of Laparoscopic & Robotic Surgeons.
Figures
References
-
- Hays RD, Morales LS. The RAND-36 measure of health-related quality of life. Ann Med. 2001;33(5):350–357. - PubMed
-
- Meston CM, Freihart BK, Handy AB, Kilimnik CD, Rosen RC. Scoring and interpretation of the FSFI: what can be learned from 20 years of use? J Sex Med. 2020;17(1):17–25. - PubMed
-
- Rattner DW, Hawes R, Schwaitzberg S, Kochman M, Swanstrom L. The second SAGES/ASGE white paper on natural orifice transluminal endoscopic surgery: 5 years of progress. Surg Endosc. 2011;25(8):2441–2448. - PubMed
-
- Kalloo AN, Singh VK, Jagannath SB, et al. . Flexible transgastric peritoneoscopy: a novel approach to diagnostic and therapeutic interventions in the peritoneal cavity. Gastrointest Endosc. 2004;60(1):114–117. - PubMed
-
- Zornig C, Emmermann A, Von Waldenfels HA, Mofid H. Laparoscopic cholecystectomy without visible scar: combined transvaginal and transumbilical approach. Endoscopy. 2007;39(10):913–915. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical