Intraoperative fat embolism syndrome associated with implantation of titanium sacroiliac joint fusion implants: a report of two cases
- PMID: 38567009
- PMCID: PMC10982924
- DOI: 10.21037/jss-23-87
Intraoperative fat embolism syndrome associated with implantation of titanium sacroiliac joint fusion implants: a report of two cases
Abstract
Background: For patients undergoing long-construct fusion surgeries, simultaneous sacroiliac joint (SIJ) fusion is a growing trend in spine surgery. Some options for posterior SIJ fusion include 3D-printed triangular titanium implants or self-harvesting SIJ screws. Both implants require fixation within the sacrum and ileum. Fat embolism syndrome is a rare but known complication of lumbar pedicle instrumentation but has never been reported in association with SIJ fusion, regardless of implant type. We report the first two known cases of fat embolism associated with placement of SIJ fusion devices during long construct posterior spine fusion.
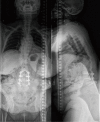
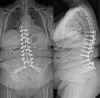
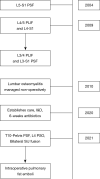
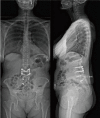
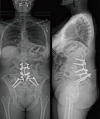
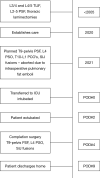
Case description: Case 1-a 50-year-old female with multiple previous spine surgeries complicated by osteomyelitis/diskitis that was successfully eradicated, underwent T10-pelvis posterior spinal fusion (PSF), L4 pedicle-subtracting-osteotomy, and bilateral SIJ fusion. During implantation of each SIJ fusion device, the patient's hemodynamic status deteriorated necessitating vasopressor support, intravenous fluid bolus, and hyperventilation, but quickly resolved. The case was completed without further issue, and she had an uneventful post-operative course. Case 2-a 71-year-old female with a past medical history of ankylosing spondylitis, previous L2-L5 PSF, rheumatoid arthritis on chronic steroids, underwent a T9-pelvis PSF, bilateral SIJ fusion, L4 pedicle subtraction osteotomy, T10-L1 Smith Peterson osteotomies. After implantation of the second SIJ fusion device, she became hypotensive and tachycardic, pulses were absent, and cardiopulmonary resuscitation was initiated. Pulses returned quickly, the index surgery was terminated, and she was transferred to the intensive care unit (ICU). In the ICU she was quickly weaned off the ventilator on post-operative day 1. On post-operative day 4, the patient returned to the operating room for completion of the surgery and had an extended, but uneventful, recovery afterwards.
Conclusions: We report on the first two known cases of fat embolism syndrome occurring immediately after implantation of SIJ fusion devices. Spine surgeons should be aware of this rare, but potentially fatal, complication. Collaboration with the anesthesia team and optimization of the patient's hemodynamic status prior to implantation may help prevent catastrophic complications.
Keywords: Fat embolism syndrome; case report; intraoperative fat embolism; sacroiliac joint fusion (SIJ fusion).
2024 Journal of Spine Surgery. All rights reserved.
Conflict of interest statement
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at https://jss.amegroups.com/article/view/10.21037/jss-23-87/coif). D.C.O.Y. reports the grants from Globus, Medtronic, SeaSpine; Royalties from SeaSpine; consulting fees from Medtronic, SeaSpine. He also received the payment from Medtronic Advisory Board for Participation on a Data Safety Monitoring Board or Advisory Board. C.J.K. reports the grants from Globus, Medtronic, SeaSpine, Medacta, Personalized Spine Study Group, Synergy, SI Bone and consulting fee from Medtronic, Allosource, SeaSpine Inc., Biocomposites. The other authors have no conflicts of interest to declare.
Figures
Similar articles
-
CT Scan and Clinical Outcomes of Novel Lateral-Oblique Percutaneous Sacroiliac Joint (SIJ) Fixation: Technique and Literature Review.Cureus. 2021 Jul 15;13(7):e16408. doi: 10.7759/cureus.16408. eCollection 2021 Jul. Cureus. 2021. PMID: 34277312 Free PMC article.
-
Multiple Points of Pelvic Fixation: Stacked S2-Alar-Iliac Screws (S2AI) or Concurrent S2AI and Open Sacroiliac Joint Fusion with Triangular Titanium Rod.JBJS Essent Surg Tech. 2022 Oct 7;12(4):e21.00044. doi: 10.2106/JBJS.ST.21.00044. eCollection 2022 Oct-Dec. JBJS Essent Surg Tech. 2022. PMID: 36743282 Free PMC article.
-
Lumbar fusion leads to increases in angular motion and stress across sacroiliac joint: a finite element study.Spine (Phila Pa 1976). 2009 Mar 1;34(5):E162-9. doi: 10.1097/BRS.0b013e3181978ea3. Spine (Phila Pa 1976). 2009. PMID: 19247155
-
Fatal fat embolism syndrome during posterior spinal fusion surgery: A case report and literature review.Medicine (Baltimore). 2021 Dec 23;100(51):e28381. doi: 10.1097/MD.0000000000028381. Medicine (Baltimore). 2021. PMID: 34941165 Free PMC article. Review.
-
[Minimally invasive arthrodesis of the sacroiliac joint (SIJ)].Oper Orthop Traumatol. 2022 Apr;34(2):98-108. doi: 10.1007/s00064-021-00738-3. Epub 2021 Oct 18. Oper Orthop Traumatol. 2022. PMID: 34661704 Review. German.
Cited by
-
Fatal Fat Embolism Syndrome After Posterior Spinal Fusion: A Case Report.Cureus. 2024 Oct 14;16(10):e71480. doi: 10.7759/cureus.71480. eCollection 2024 Oct. Cureus. 2024. PMID: 39539860 Free PMC article.
References
-
- Manzetti M, Ruffilli A, Barile F, et al. Sacroiliac Joint Degeneration and Pain After Spinal Arthrodesis: A Systematic Review. Clin Spine Surg 2023;36:169-82. - PubMed
-
- Anwar FN, Nie JW, Hartman TJ, et al. Presentation, diagnosis, and treatment of sacroiliac joint dysfunction. Contem Spine Surg 2023;24:1-5.
Publication types
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous
