Interim analyses of a first-in-human phase 1/2 mRNA trial for propionic acidaemia
- PMID: 38570682
- PMCID: PMC11156579
- DOI: 10.1038/s41586-024-07266-7
Interim analyses of a first-in-human phase 1/2 mRNA trial for propionic acidaemia
Erratum in
-
Author Correction: Interim analyses of a first-in-human phase 1/2 mRNA trial for propionic acidaemia.Nature. 2024 May;629(8011):E10. doi: 10.1038/s41586-024-07413-0. Nature. 2024. PMID: 38649490 No abstract available.
-
Publisher Correction: Interim analyses of a first-in-human phase 1/2 mRNA trial for propionic acidaemia.Nature. 2024 Jun;630(8017):E13. doi: 10.1038/s41586-024-07646-z. Nature. 2024. PMID: 38844679 Free PMC article. No abstract available.
Abstract
Propionic acidaemia is a rare disorder caused by defects in the propionyl-coenzyme A carboxylase α or β (PCCA or PCCB) subunits that leads to an accumulation of toxic metabolites and to recurrent, life-threatening metabolic decompensation events. Here we report interim analyses of a first-in-human, phase 1/2, open-label, dose-optimization study and an extension study evaluating the safety and efficacy of mRNA-3927, a dual mRNA therapy encoding PCCA and PCCB. As of 31 May 2023, 16 participants were enrolled across 5 dose cohorts. Twelve of the 16 participants completed the dose-optimization study and enrolled in the extension study. A total of 346 intravenous doses of mRNA-3927 were administered over a total of 15.69 person-years of treatment. No dose-limiting toxicities occurred. Treatment-emergent adverse events were reported in 15 out of the 16 (93.8%) participants. Preliminary analysis suggests an increase in the exposure to mRNA-3927 with dose escalation, and a 70% reduction in the risk of metabolic decompensation events among 8 participants who reported them in the 12-month pretreatment period.
© 2024. The Author(s), under exclusive licence to Springer Nature Limited.
Conflict of interest statement
D.K. is a consultant for Amicus, Genzyme Sanofi, Sangamo Therapeutics, Takeda and Vertex; is a grant support recipient from Amicus, Genzyme Sanofi, Roivant Rare Diseases and Viking Therapeutics; and has equity in AskBio–Bayer. A.S. is an investigator and consultant for Moderna, Ultragenyx and iEcure; and is a consultant and/or advisory board member for Aeglea, Beam, Ceres Brain, Horizon, iEcure, MTPharma, Recordati and Satellite Bio. N.S. was an investigator and consultant for Moderna at the time of the study and is a current employee of Synlogic. G.S.L. has research grants from Moderna and has served as a consultant for Audentes Therapuetics, Taysha Therapeutics and Tenaya Therapeutics. T.G. is an investigator for Moderna. L.L., R.S., J.L., V.S., L.J. and M. Liang are employees of Moderna and hold stock or stock options in the company. At the time of the study, M. Leuchars was an employee of Moderna and held stock or stock options in the company. S.G. is an investigator, consultant, advisory board member and recipient of travel reimbursements for Moderna, and consults for BridgeBio, Glycomine, Jaguar, Orphazyme and Ultragenyx.
Figures
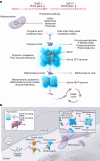



Comment in
-
mRNA therapy shows promise for metabolic disorder.Nat Rev Drug Discov. 2024 Jun;23(6):416. doi: 10.1038/d41573-024-00071-x. Nat Rev Drug Discov. 2024. PMID: 38654137 No abstract available.
References
-
- Shchelochkov, O. A., Carrillo, N. & Venditti, C. Propionic acidemia. In GeneReviews (eds Adam, M. P. et al.) (Univ. Washington, 1993).
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Molecular Biology Databases
Research Materials

