Infective Endocarditis and Antithrombotic Therapy
- PMID: 38574483
- PMCID: PMC11449188
- DOI: 10.1159/000538549
Infective Endocarditis and Antithrombotic Therapy
Abstract
Background: Incidence of infective endocarditis (IE) is progressively raising because of the increasing number of cardiovascular invasive procedures, support treatment and devices, awareness in the medical community, and improved diagnostic modalities. IE pathophysiology is a unique model of immunothrombosis, and the clinical course is often complicated by either embolic or hemorrhagic events. Managing antithrombotic treatment is challenging and the level of supporting evidence scant. The aim of this review was to discuss and present the embolic and bleeding complication associated with IE and review the available evidence on antithrombotic treatment in patients with IE with and without a previous indication to antithrombotic drugs.
Summary: Embolic events occur in 20-40% of patients with IE and are associated with high morbidity and mortality. Acute ischemic stroke is the most common neurological complication. A beneficial effect of antithrombotic therapy in preventing ischemic stroke for patients with IE has never been formally tested in adequately powered randomized clinical trials. Atrial fibrillation is a common complication associated with severe infections, requiring anticoagulation. Furthermore, patients with IE have a high risk of unprovoked and anticoagulation treatment-related bleeding. In particular, intracerebral bleeding is the most severe complication in about 5% of patients with IE. Single antiplatelet therapy with low-dose aspirin after hospitalization for IE has been shown to reduce causes mortality within 90 days without an increase of hemorrhagic strokes. In the absence of bleeding complications, recent guidelines recommend to maintain low-dose aspirin. No data are available on the management of patients with IE while on dual antiplatelet therapy.
Key messages: Several gaps in knowledge remain about antithrombotic management in patients with IE and most of the evidence relies on observational studies. Individualized strategies based on clinical evaluation, comorbidities, patient engagement, and shared decisions strategies are encouraged.
Keywords: Anticoagulant; Antiplatelet drugs; Bleeding complications; Infective endocarditis.
© 2024 The Author(s). Published by S. Karger AG, Basel.
Conflict of interest statement
The authors have no conflicts of interest to declare.
Figures
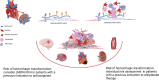
References
-
- Sipilä PN, Lindbohm JV, Batty GD, Heikkilä N, Vahtera J, Suominen S, et al. . Severe infection and risk of cardiovascular disease: a multicohort study. Circulation. 2023;147(21):1582–93. - PubMed
-
- Shah BR, Hux JE. Quantifying the risk of infectious diseases for people with diabetes. Diabetes Care. 2003;26(2):510–3. - PubMed
-
- Gigante B, Levy JH, van Gorp E, Bartoloni A, Bochaton-Piallat M-L, Bäck M, et al. . Management of patients on antithrombotic therapy with severe infections: a joint clinical consensus statement of the ESC working group on thrombosis, the ESC working group on atherosclerosis and vascular biology, and the international society on thrombosis and haemostasis. Eur Heart J. 2023;44(32):3040–58. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

