Patient Portal Enrollment for Discharged Pediatric Emergency Department Patients: A Multidisciplinary Quality Improvement Project
- PMID: 38576887
- PMCID: PMC10990375
- DOI: 10.1097/pq9.0000000000000718
Patient Portal Enrollment for Discharged Pediatric Emergency Department Patients: A Multidisciplinary Quality Improvement Project
Abstract
Introduction: Patient portal enrollment following pediatric emergency department (ED) visits allows access to critical results, physician documentation, and telehealth follow-up options. Despite these advantages, there are many challenges to portal invitation and enrollment. Our primary objective was to improve patient portal enrollment rates for discharged pediatric ED patients.
Methods: A multidisciplinary team of staff from two ED sites developed successful portal enrollment interventions through sequential Plan-Do-Study-Act cycles from October 2020 to October 2021. Interventions included a new invitation process, changes to patient paperwork on ED arrival, staff portal education, and changes to discharge paperwork and the portal website. The team utilized statistical process control charts to track the percentage of eligible discharged patients who received a portal invitation (process measure) and enrolled in the patient portal.
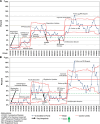
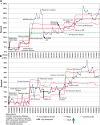
Results: Before the study's initiation, less than 1% of eligible patients received patient portal invites or enrolled in the patient portal. Statistical process control charts revealed significant changes in enrollment and baseline shift at both a large academic ED campus and a satellite ED site by May 2021. Improvements in invitation rates were also observed at both campuses. Changes were sustained for over 6 months at both locations.
Conclusions: High-reliability interventions and a multidisciplinary approach allowed for significant and sustained improvement in patient portal invitation and enrollment rates in eligible pediatric ED patients. Future study will examine enrollment patterns across patient demographics and further high-reliability interventions.
Copyright © 2024 the Author(s). Published by Wolters Kluwer Health, Inc.
Figures

Similar articles
-
Adult emergency department patients with sickle cell pain crisis: a learning collaborative model to improve analgesic management.Acad Emerg Med. 2010 Apr;17(4):399-407. doi: 10.1111/j.1553-2712.2010.00693.x. Acad Emerg Med. 2010. PMID: 20370779
-
Telehealth Pharmacist Approach to Comprehensive Medication Management in Post-Discharge High-Risk Patients: A Quality Improvement Initiative.Telemed J E Health. 2024 Apr;30(4):976-986. doi: 10.1089/tmj.2023.0239. Epub 2023 Nov 17. Telemed J E Health. 2024. PMID: 37976134
-
Seventy-two-hour Return Initiative: Improving Emergency Department Discharge to Decrease Returns.Pediatr Qual Saf. 2020 Sep 25;5(5):e342. doi: 10.1097/pq9.0000000000000342. eCollection 2020 Sep-Oct. Pediatr Qual Saf. 2020. PMID: 34616961 Free PMC article.
-
COPD Care Bundle in Emergency Department Observation Unit Reduces Emergency Department Revisits.Respir Care. 2020 Jan;65(1):1-10. doi: 10.4187/respcare.07088. Respir Care. 2020. PMID: 31882412
-
Improving Documentation of Firearm Access During Pediatric Emergency Visits for Suicidal Ideation.Pediatrics. 2024 Apr 1;153(4):e2023063447. doi: 10.1542/peds.2023-063447. Pediatrics. 2024. PMID: 38426287 Review.
Cited by
-
Pediatric Emergency Department Burn Discharge and Clinic Readiness: A Quality Improvement Project.Pediatr Qual Saf. 2025 Apr 16;10(3):e806. doi: 10.1097/pq9.0000000000000806. eCollection 2025 May-Jun. Pediatr Qual Saf. 2025. PMID: 40248386 Free PMC article.
References
-
- Sebelius K. HIPAA administrative simplification: enforcement. Fed Regist. 2009;74:56123–56131. - PubMed
-
- Azar II AM. 21st Century Cures Act: Interoperability, Information Blocking, and the ONC Health IT Certification Program. In: Office of the National Coordinator for Health Information Technology (ONC), ed. Federal Registrar, Department of Health and Human Services; 2020:25642–25961.
LinkOut - more resources
Full Text Sources
