Amebic liver abscess: An update
- PMID: 38577528
- PMCID: PMC10989314
- DOI: 10.4254/wjh.v16.i3.316
Amebic liver abscess: An update
Abstract
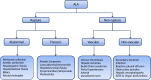
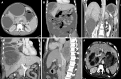
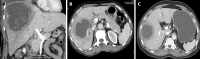
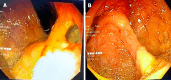
Amebic liver abscess (ALA) is still a common problem in the tropical world, where it affects over three-quarters of patients with liver abscess. It is caused by an anaerobic protozoan Entamoeba hystolytica, which primarily colonises the cecum. It is a non-suppurative infection of the liver consisting primarily of dead hepatocytes and cellular debris. People of the male gender, during their reproductive years, are most prone to ALA, and this appears to be due to a poorly mounted immune response linked to serum testosterone levels. ALA is more common in the right lobe of the liver, is strongly associated with alcohol consumption, and can heal without the need for drainage. While majority of ALA patients have an uncomplicated course, a number of complications have been described, including rupture into abdomino-thoracic structures, biliary fistula, vascular thrombosis, bilio-vascular compression, and secondary bacterial infection. Based on clinico-radiological findings, a classification system for ALA has emerged recently, which can assist clinicians in making treatment decisions. Recent research has revealed the role of venous thrombosis-related ischemia in the severity of ALA. Recent years have seen the development and refinement of newer molecular diagnostic techniques that can greatly aid in overcoming the diagnostic challenge in endemic area where serology-based tests have limited accuracy. Metronidazole has been the drug of choice for ALA patients for many years. However, concerns over the resistance and adverse effects necessitate the creation of new, safe, and potent antiamebic medications. Although the indication of the drainage of uncomplicated ALA has become more clear, high-quality randomised trials are still necessary for robust conclusions. Percutaneous drainage appears to be a viable option for patients with ruptured ALA and diffuse peritonitis, for whom surgery represents a significant risk of mortality. With regard to all of the aforementioned issues, this article intends to present an updated review of ALA.
Keywords: Amebiasis; Amebic liver abscess; Metronidazole; Percutaneous drainage; Ruptured liver abscess.
©The Author(s) 2024. Published by Baishideng Publishing Group Inc. All rights reserved.
Conflict of interest statement
Conflict-of-interest statement: All the authors report no relevant conflicts of interest for this article.
Figures

References
-
- Jackson-Akers JY, Prakash V, Oliver TI. Amebic Liver Abscess. 2023 Aug 8. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024. - PubMed
-
- Haque R, Huston CD, Hughes M, Houpt E, Petri WA Jr. Amebiasis. N Engl J Med. 2003;348:1565–1573. - PubMed
-
- Khairnar K, Parija SC, Palaniappan R. Diagnosis of intestinal amoebiasis by using nested polymerase chain reaction-restriction fragment length polymorphism assay. J Gastroenterol. 2007;42:631–640. - PubMed
Publication types
LinkOut - more resources
Full Text Sources

