Access to Specialty Care for Commercially Insured Youths With Type 1 and Type 2 Diabetes
- PMID: 38578636
- PMCID: PMC10998152
- DOI: 10.1001/jamanetworkopen.2024.5656
Access to Specialty Care for Commercially Insured Youths With Type 1 and Type 2 Diabetes
Abstract
Importance: Youths with type 2 diabetes are at higher risk for complications compared with peers with type 1 diabetes, though few studies have evaluated differences in access to specialty care.
Objective: To compare claims with diabetes specialists for youths with type 1 vs type 2 diabetes and the association between specialist claims with multidisciplinary and acute care utilization.
Design, setting, and participants: This cross-sectional study used Optum Clinformatics Data Mart commercial claims. Individuals included in the study were youths younger than 19 years with type 1 or 2 diabetes as determined by a validated algorithm and prescription claims. Data were collected for youths with at least 80% enrollment in a commercial health plan from December 1, 2018, to December 31, 2019. Statistical analysis was performed from September 2022 to January 2024.
Main outcomes and measures: The primary outcome was the number of ambulatory claims from an endocrine and/or diabetes physician or advanced practice clinician associated with a diabetes diagnosis code; secondary outcomes included multidisciplinary and acute care claims.
Results: Claims were analyzed for 4772 youths (mean [SD] age, 13.6 [3.7] years; 4300 [90.1%] type 1 diabetes; 472 [9.9%] type 2 diabetes; 2465 [51.7%] male; 128 [2.7%] Asian, 303 [6.4] Black or African American, 429 [9.0%] Hispanic or Latino, 3366 [70.5%] non-Hispanic White, and 546 [11.4%] unknown race and ethnicity). Specialist claims were lower in type 2 compared with type 1 diabetes (incidence rate ratio [IRR], 0.61 [95% CI, 0.52-0.72]; P < .001) in propensity score-weighted analyses. The presence of a comorbidity was associated with increased specialist claims for type 1 diabetes (IRR, 1.07 [95% CI, 1.03-1.10]) and decreased claims for type 2 diabetes (IRR, 0.77 [95% CI, 0.67-0.87]). Pooling diagnosis groups and adjusted for covariates, each additional specialist claim was associated with increased odds of a claim with a diabetes care and education specialist (odds ratio [OR], 1.31 [95% CI, 1.25-1.36]), dietitian (OR, 1.14 [95% CI, 1.09-1.19]), and behavioral health clinician (OR, 1.16 [95% CI, 1.12-1.20]). For acute care claims, each additional specialist claim was associated with increased odds of admission (OR, 1.17 [95% CI, 1.11-1.24]) but not for emergency claims (OR, 1.03 [95% CI, 0.98-1.82]).
Conclusions and relevance: This cross-sectional study found that youths with type 2 diabetes were significantly less likely to have specialist claims despite insurance coverage, indicating other barriers to care, which may include medical complexity. Access to diabetes specialists influences engagement with multidisciplinary services. The association between increasing ambulatory clinician services and admissions suggests high utilization by a subgroup of patients at greater risk for poor outcomes.
Conflict of interest statement
Figures
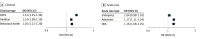
Similar articles
-
Association Between Race/Ethnicity and Disparities in Health Care Use Before First-Episode Psychosis Among Privately Insured Young Patients.JAMA Psychiatry. 2021 Mar 1;78(3):311-319. doi: 10.1001/jamapsychiatry.2020.3995. JAMA Psychiatry. 2021. PMID: 33355626 Free PMC article.
-
Sociodemographic, Clinical, and Treatment-Related Factors Associated With Hyperglycemic Crises Among Adults With Type 1 or Type 2 Diabetes in the US From 2014 to 2020.JAMA Netw Open. 2021 Sep 1;4(9):e2123471. doi: 10.1001/jamanetworkopen.2021.23471. JAMA Netw Open. 2021. PMID: 34468753 Free PMC article.
-
Clinical and Demographic Factors Associated With Diabetic Retinopathy Among Young Patients With Diabetes.JAMA Netw Open. 2021 Sep 1;4(9):e2126126. doi: 10.1001/jamanetworkopen.2021.26126. JAMA Netw Open. 2021. PMID: 34570208 Free PMC article.
-
Prediabetes Prevalence by Adverse Social Determinants of Health in Adolescents.JAMA Netw Open. 2024 Jun 3;7(6):e2416088. doi: 10.1001/jamanetworkopen.2024.16088. JAMA Netw Open. 2024. PMID: 38861258 Free PMC article.
-
Relationship between glycemic control and diabetes-related hospital costs in patients with type 1 or type 2 diabetes mellitus.J Manag Care Pharm. 2010 May;16(4):264-75. doi: 10.18553/jmcp.2010.16.4.264. J Manag Care Pharm. 2010. PMID: 20433217 Free PMC article.
Cited by
-
Diabetes visits in paediatric versus adult clinics for young adults (YA) with T1D: Pre-pandemic and pandemic care.Diabet Med. 2025 May;42(5):e15509. doi: 10.1111/dme.15509. Epub 2025 Jan 18. Diabet Med. 2025. PMID: 39826105
-
Pharmacoequity measurement framework: A tool to reduce health disparities.J Manag Care Spec Pharm. 2025 Feb 1;31(2):214-224. doi: 10.18553/jmcp.2025.31.2.214. Epub 2024 Dec 20. J Manag Care Spec Pharm. 2025. PMID: 39912813 Free PMC article.
-
Patient Characteristics Associated With Annual Nutrition Visits in Children With Type 1 Diabetes.Pediatr Diabetes. 2025;2025:4108685. doi: 10.1155/pedi/4108685. Epub 2025 Mar 28. Pediatr Diabetes. 2025. PMID: 40322222 Free PMC article.
References
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

