A Short Fully Covered Self-Expandable Metal Stent for Management of Benign Biliary Stricture Not Caused by Living-Donor Liver Transplantation
- PMID: 38592022
- PMCID: PMC10931574
- DOI: 10.3390/jcm13051186
A Short Fully Covered Self-Expandable Metal Stent for Management of Benign Biliary Stricture Not Caused by Living-Donor Liver Transplantation
Abstract
Background: This study evaluated the effectiveness of short fully covered self-expanding metal stents (FCSEMS) with an anti-migration design in treating benign biliary strictures (BBS) not related to living donor liver transplantation (LDLT). Methods: A retrospective analysis was conducted on 75 patients who underwent FCSEMS insertion for BBS management. Stents were initially kept for 3 months and exchanged every 3 months until stricture resolution. Adverse events and stricture recurrence after FCSEMS removal were assessed during follow-up. Results: The study outcomes were technical success, stenosis resolution, and treatment failure. Technical success was 100%, with stricture resolution in 99% of patients. The mean onset time of BBS post-surgery was 4.4 years, with an average stent indwelling period of 5.5 months. Stricture recurrence occurred in 20% of patients, mostly approximately 18.8 months after stent removal. Early cholangitis and stent migration were noted in 3% and 4% of patients, respectively. Conclusions: This study concludes that short FCSEMS demonstrate high efficacy in the treatment of non-LDLT-related BBS, with a low incidence of interventions and complications. Although this is a single-center, retrospective study with a limited sample size, the findings provide preliminary evidence supporting the use of short FCSEMS as a primary treatment modality for BBS. To substantiate these findings, further research involving multicenter studies is recommended to provide additional validation and a broader perspective.
Keywords: benign biliary stricture; endoscopic retrograde cholangiopancreatography; fully covered self-expanding metal stent.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures

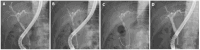
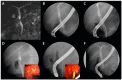

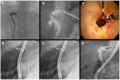
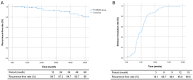
Similar articles
-
Short fully covered self-expandable metal stent for treatment of proximal anastomotic benign biliary stricture after living-donor liver transplantation.Dig Endosc. 2021 Jul;33(5):840-848. doi: 10.1111/den.13871. Epub 2020 Nov 24. Dig Endosc. 2021. PMID: 33043522
-
Evaluation of the Feasibility and Effectiveness of Placement of Fully Covered Self-Expandable Metallic Stents via Various Insertion Routes for Benign Biliary Strictures.J Clin Med. 2021 May 28;10(11):2397. doi: 10.3390/jcm10112397. J Clin Med. 2021. PMID: 34071678 Free PMC article.
-
A prospective group sequential study evaluating a new type of fully covered self-expandable metal stent for the treatment of benign biliary strictures (with video).Gastrointest Endosc. 2012 Apr;75(4):783-9. doi: 10.1016/j.gie.2011.10.022. Epub 2012 Feb 10. Gastrointest Endosc. 2012. PMID: 22325806 Clinical Trial.
-
Covered Self-Expanding Metal Stents Versus Multiple Plastic Stents for Benign Biliary Strictures: An Updated Meta-Analysis of Randomized Controlled Trials.Cureus. 2022 Apr 29;14(4):e24588. doi: 10.7759/cureus.24588. eCollection 2022 Apr. Cureus. 2022. PMID: 35651420 Free PMC article. Review.
-
Efficacy of Different Endoscopic Stents in the Management of Postoperative Biliary Strictures: A Systematic Review and Meta-analysis.J Clin Gastroenterol. 2019 Jul;53(6):418-426. doi: 10.1097/MCG.0000000000001193. J Clin Gastroenterol. 2019. PMID: 30807403
References
LinkOut - more resources
Full Text Sources

