Arrhythmic Mitral Valve Prolapse and Sports Activity: Pathophysiology, Risk Stratification, and Sports Eligibility Assessment
- PMID: 38592178
- PMCID: PMC10932446
- DOI: 10.3390/jcm13051350
Arrhythmic Mitral Valve Prolapse and Sports Activity: Pathophysiology, Risk Stratification, and Sports Eligibility Assessment
Abstract
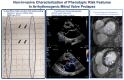
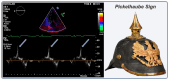
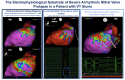
Although mitral valve prolapse (MVP) is the most prevalent valvular abnormality in Western countries and generally carries a good prognosis, a small subset of patients is exposed to a significant risk of malignant ventricular arrhythmias (VAs) and sudden cardiac death (SCD), the so-called arrhythmic MVP (AMVP) syndrome. Recent work has emphasized phenotypical risk features of severe AMVP and clarified its pathophysiology. However, the appropriate assessment and risk stratification of patients with suspected AMVP remains a clinical conundrum, with the possibility of both overestimating and underestimating the risk of malignant VAs, with the inappropriate use of advanced imaging and invasive electrophysiology study on one hand, and the catastrophic occurrence of SCD on the other. Furthermore, the sports eligibility assessment of athletes with AMVP remains ill defined, especially in the grey zone of intermediate arrhythmic risk. The definition, epidemiology, pathophysiology, risk stratification, and treatment of AMVP are covered in the present review. Considering recent guidelines and expert consensus statements, we propose a comprehensive pathway to facilitate appropriate counseling concerning the practice of competitive/leisure-time sports, envisioning shared decision making and the multidisciplinary "sports heart team" evaluation of borderline cases. Our final aim is to encourage an active lifestyle without compromising patients' safety.
Keywords: arrhythmic mitral valve prolapse; electroanatomical mapping; electrophysiology study; guidelines; mitral regurgitation; mitral valve prolapse; physical exercise; risk stratification; sports cardiology; ventricular arrhythmias.
Conflict of interest statement
Dr. Natale is a consultant for Biosense Webster, Stereotaxis, and Abbott Medical and has received speaker honoraria/travel from Medtronic, Atricure, Biotronik, and Janssen; Dr. Dello Russo is a consultant for Abbott Medical; Dr. Casella has received speaker honoraria from Biosense Webster. All other authors declared no conflicts of interest.
Figures


Similar articles
-
Arrhythmic mitral valve prolapse and mitral annular disjunction: pathophysiology, risk stratification, and management.Eur Heart J. 2023 Sep 1;44(33):3121-3135. doi: 10.1093/eurheartj/ehad491. Eur Heart J. 2023. PMID: 37561995 Review.
-
Arrhythmic Mitral Valve Prolapse Syndrome and Ventricular Arrhythmias: A Comprehensive Review and the Role of Catheter Ablation.J Cardiovasc Dev Dis. 2024 Jul 10;11(7):218. doi: 10.3390/jcdd11070218. J Cardiovasc Dev Dis. 2024. PMID: 39057638 Free PMC article. Review.
-
Arrhythmic Mitral Valve Prolapse: A Comprehensive Review.Diagnostics (Basel). 2023 Sep 6;13(18):2868. doi: 10.3390/diagnostics13182868. Diagnostics (Basel). 2023. PMID: 37761235 Free PMC article. Review.
-
Effectiveness of the risk stratification proposed by the 2022 European Heart Rhythm Association Expert Consensus statement on arrhythmic mitral valve prolapse.Am Heart J. 2023 Dec;266:48-60. doi: 10.1016/j.ahj.2023.08.004. Epub 2023 Aug 16. Am Heart J. 2023. PMID: 37595658
-
Arrhythmic Mitral Valve Prolapse: Risk Assessment and Management.Can J Cardiol. 2023 Oct;39(10):1397-1409. doi: 10.1016/j.cjca.2023.05.010. Epub 2023 May 20. Can J Cardiol. 2023. PMID: 37217162 Review.
References
-
- Theal M., Sleik K., Anand S., Yi Q., Yusuf S., Lonn E. Prevalence of mitral valve prolapse in ethnic groups. Can. J. Cardiol. 2004;20:511–515. - PubMed
-
- Sabbag A., Essayagh B., Barrera J.D.R., Basso C., Berni A., Cosyns B., Deharo J.C., Deneke T., Di Biase L., Enriquez-Sarano M., et al. EHRA expert consensus statement on arrhythmic mitral valve prolapse and mitral annular disjunction complex in collaboration with the ESC Council on valvular heart disease and the European Association of Cardiovascular Imaging endorsed by the Heart Rhythm Society, by the Asia Pacific Heart Rhythm Society, and by the Latin American Heart Rhythm Society. Europace. 2022;24:1981–2003. doi: 10.1093/europace/euac125. - DOI - PMC - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Miscellaneous

