Associations of fasting plasma glucose with all-cause mortality and cardiovascular events in older Chinese diabetes patients: A population-based cohort study
- PMID: 38593274
- PMCID: PMC11292386
- DOI: 10.1111/jdi.14196
Associations of fasting plasma glucose with all-cause mortality and cardiovascular events in older Chinese diabetes patients: A population-based cohort study
Abstract
Aims/introduction: Our aim was to investigate the optimal fasting glucose (FPG) range in Chinese older adults with type 2 diabetes, and to clarify whether the optimal range varies according to the control of risk factors.
Materials and methods: The baseline survey for the cohort study began in 2018, with follow up ending in 2022. Our study enrolled 59,030 older diabetes patients with no history of cardiovascular disease (CVD). Participants were divided into nine groups based on their baseline glycemic status. The association between FPG and the risk of adverse outcomes was mainly estimated by multivariate Cox proportional risk models and restricted spline analysis.
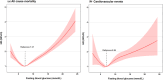
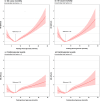
Results: During the 4-year follow-up period, a total of 5,637 deaths and 4,904 CVD events occurred. The associations of FPG with mortality and CVD events showed J-shaped curves. Among all-cause deaths, the hazard ratios for FPG ≤4.50 and >11.50 mmol/L were 1.50 (95% confidence interval [CI] 1.31-1.71) and 1.84 (95% CI 1.67-2.02). Among CVD, the hazard ratios for FPG ≤4.50 and >11.50 mmol/L were 1.31 (95% CI 1.13-1.53) and 1.71 (95% CI 1.54-1.89), respectively. The optimal FPG ranges of all-cause mortality and CVD were 5.50-7.50 and 4.50-7.50 mmol/L, respectively. For participants with at least two risk factors, the optimal FPG levels were higher than those with fewer risk factors.
Conclusions: In older Chinese diabetes patients, the FPG ranges related to the minimum death and CVD event rates were 5.50-7.50 and 4.50-7.50 mmol/L, respectively. Patients with more cardiovascular risk factors had higher optimal blood glucose ranges than those with fewer risk factors.
Keywords: Cardiovascular disease; Diabetes patient; Fasting plasma glucose.
© 2024 The Authors. Journal of Diabetes Investigation published by Asian Association for the Study of Diabetes (AASD) and John Wiley & Sons Australia, Ltd.
Conflict of interest statement
The authors declare no conflict of interest.
Approval of the research protocol: This study was approved by the Ethics Committee of the Wuhan Centers for Disease Control and Prevention (protocol code WHCDCIRB‐K‐2018023).
Informed consent: The written informed consent was obtained from all participants.
Registry and the registration no. of the study/trial: N/A.
Animal studies: N/A.
Figures
Similar articles
-
Visit-to-Visit Variability of Fasting Plasma Glucose and the Risk of Cardiovascular Disease and All-Cause Mortality in the General Population.J Am Heart Assoc. 2017 Nov 29;6(12):e006757. doi: 10.1161/JAHA.117.006757. J Am Heart Assoc. 2017. PMID: 29187392 Free PMC article.
-
The association between fasting plasma glucose and all-cause and cause-specific mortality by gender: The rural Chinese cohort study.Diabetes Metab Res Rev. 2019 May;35(4):e3129. doi: 10.1002/dmrr.3129. Epub 2019 Feb 27. Diabetes Metab Res Rev. 2019. PMID: 30657630
-
Predictive Value of Fasting Glucose, Postload Glucose, and Hemoglobin A1c on Risk of Diabetes and Complications in Chinese Adults.Diabetes Care. 2019 Aug;42(8):1539-1548. doi: 10.2337/dc18-1390. Epub 2019 May 31. Diabetes Care. 2019. PMID: 31152120
-
Development of type 2 diabetes mellitus in people with intermediate hyperglycaemia.Cochrane Database Syst Rev. 2018 Oct 29;10(10):CD012661. doi: 10.1002/14651858.CD012661.pub2. Cochrane Database Syst Rev. 2018. PMID: 30371961 Free PMC article.
-
Postprandial peaks as a risk factor for cardiovascular disease: epidemiological perspectives.Int J Clin Pract Suppl. 2002 Jul;(129):5-11. Int J Clin Pract Suppl. 2002. PMID: 12166607 Review.
Cited by
-
Association of glucose to lymphocyte ratio with all-cause and cardio-cerebrovascular mortality in diabetic population.Sci Rep. 2025 Jul 1;15(1):20530. doi: 10.1038/s41598-025-04727-5. Sci Rep. 2025. PMID: 40594197 Free PMC article.
-
The modified role including mediating and synergistic interactive effects of glucose tolerance status in the associations between relative fat mass and the risks of cardiovascular disease and all-cause mortality from the 4C cohort study.Diabetol Metab Syndr. 2024 Dec 26;16(1):313. doi: 10.1186/s13098-024-01558-8. Diabetol Metab Syndr. 2024. PMID: 39726036 Free PMC article.
References
-
- Morrish NJ, Wang SL, Stevens LK, et al. Mortality and causes of death in the WHO Multinational Study of Vascular Disease in Diabetes. Diabetologia 2001; 44: S14–S21. - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

