Nurses' Attitudes, Practices, and Barriers to Assessing Symptoms of Discomfort in Mechanically Ventilated Patients: A Cross-Sectional Study
- PMID: 38596509
- PMCID: PMC11003335
- DOI: 10.1177/23779608241245209
Nurses' Attitudes, Practices, and Barriers to Assessing Symptoms of Discomfort in Mechanically Ventilated Patients: A Cross-Sectional Study
Abstract
Introduction: Critically ill patients experience various stressful symptoms of discomfort, including dyspnea, pain, and sleep disruption. Notably, ventilated patients have difficulty self-reporting discomfort symptoms. Nurses need to assess discomfort symptoms to alleviate them, but limited research exists on discomfort symptom assessment and management in critically ill patients.
Objective: To identify the practices, attitudes, and barriers among nurses related to the assessment of discomfort symptoms in mechanically ventilated patients.
Methods: Using a cross-sectional, descriptive study design, a web-based survey was conducted between May and June 2022 with critical care nurses sampled through Japanese academic societies and social networking services. The survey contained questions relative to the above-stated objective. Descriptive statistical analysis was performed without sample size calculation because of the descriptive and exploratory nature of this study.
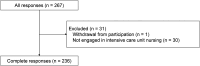
Results: There were 267 respondents to the questionnaire. The discomfort symptoms that nurses perceived as important to assess were pain (median 100 [interquartile range, IQR 90-100]), insomnia (99 [80-100]), and dyspnea (96.5 [75-100]). Most participants (89.8%) routinely assessed pain in mechanically ventilated patients using a scale; however, other discomfort symptoms were assessed by less than 40% (dyspnea [28.4%], fatigue [8.1%], thirst [13.1%], insomnia [37.3%], and anxiety [13.6%]). Two major barriers to assessing discomfort symptoms were lack of assessment culture within the intensive care unit and lack of knowledge of the relevant evaluation scales.
Conclusions: Nurses were aware of the importance of using scales to assess the discomfort symptoms experienced by mechanically ventilated patients. However, except for pain, most nurses did not routinely use scales to assess discomfort symptoms. Barriers to routine discomfort symptom assessment included the lack of an assessment culture and the lack of knowledge of the assessment scales. Clinicians should be educated regarding the existence of validated rating scales and develop additional rating scales utilizable for minor discomforts in mechanically ventilated patients.
Keywords: Discomfort symptoms; attitudes; barriers; mechanically ventilated patients; practices.
© The Author(s) 2024.
Conflict of interest statement
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Figures

Similar articles
-
Nurses' perceptions of pain management adequacy in mechanically ventilated patients.J Clin Nurs. 2019 Aug;28(15-16):2946-2952. doi: 10.1111/jocn.14896. Epub 2019 May 9. J Clin Nurs. 2019. PMID: 31013381
-
Perceptions of registered and enrolled nurses on thirst in mechanically ventilated adult patients in intensive care units-a phenomenographic study.Intensive Crit Care Nurs. 2009 Jun;25(3):133-9. doi: 10.1016/j.iccn.2009.03.001. Epub 2009 Apr 24. Intensive Crit Care Nurs. 2009. PMID: 19394226
-
Pain assessment and interventions by nurses in the emergency department: A national survey.J Clin Nurs. 2020 Jul;29(13-14):2352-2362. doi: 10.1111/jocn.15247. Epub 2020 Apr 30. J Clin Nurs. 2020. PMID: 32221999
-
Nurses' Perceived Barriers to and Facilitators of Pain Assessment and Management in Critical Care Patients: A Systematic Review.J Pain Res. 2021 Nov 5;14:3475-3491. doi: 10.2147/JPR.S332423. eCollection 2021. J Pain Res. 2021. PMID: 34764688 Free PMC article. Review.
-
Detection and management of dyspnea in mechanically ventilated patients.Curr Opin Crit Care. 2019 Feb;25(1):86-94. doi: 10.1097/MCC.0000000000000574. Curr Opin Crit Care. 2019. PMID: 30531366 Review.
Cited by
-
Development of safety protocols for managing thirst in post-extubated and tracheostomized patients.Rev Lat Am Enfermagem. 2025 May 2;33:e4497. doi: 10.1590/1518-8345.7376.4497. eCollection 2025. Rev Lat Am Enfermagem. 2025. PMID: 40332192 Free PMC article.
-
Challenges in Thirst Management for Intubated Patients in the ICU: A Qualitative Study of Healthcare Provider and Patient Perspectives.J Multidiscip Healthc. 2025 Aug 9;18:4919-4932. doi: 10.2147/JMDH.S519753. eCollection 2025. J Multidiscip Healthc. 2025. PMID: 40823480 Free PMC article.
References
-
- Alnajar M. K., Shudifat R., Mosleh S. M., Ismaile S., N’erat M., Amro K. (2021). Pain assessment and management in intensive care unit: Nurses’ practices, perceived influencing factors, and educational needs. The Open Nursing Journal, 15(1), 170–178. 10.2174/1874434602115010170 - DOI
-
- Baumstarck K., Boucekine M., Estagnasie P., Geantot M. A., Berric A., Simon G., Floccard B., Signouret T., Fromentin M., Nyunga M., Sossou A., Venot M., Robert R., Follin A., Audibert J., Renault A., Garrouste-Orgeas M., Collange O., Levrat Q., Chaban Y. (2019). Assessment of patients’ self-perceived intensive care unit discomforts: Validation of the 18-item version of the IPREA. Health and Quality of Life Outcomes, 17(1), 1–9. 10.1186/s12955-019-1101-5 - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources

