Left ventricular free wall rupture caused by myocardial ischemia without treatable atherosclerotic coronary disease: a case series
- PMID: 38609970
- PMCID: PMC11010315
- DOI: 10.1186/s13019-024-02690-2
Left ventricular free wall rupture caused by myocardial ischemia without treatable atherosclerotic coronary disease: a case series
Abstract
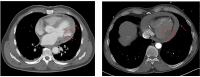
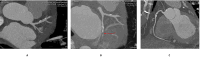
Background: The clinical presentation of left ventricular free wall rupture (LVFWR) varies ranging from uneventful condition to congestive heart failure. Here we report two cases of LVFWR with different clinical presentation and notable outcome. A 53-year-old male presenting emergently with signs of myocardial infarction received immediate coronary angiography and thoracic CT-scan showing occlusion of the first marginal coronary branch without possibility of revascularization and minimal pericardial extravasation. Under ICU surveillance, LVFWR occurred 24 h later and was treated by pericardiocentesis and ECMO support followed by immediate uncomplicated surgical repair. Postoperative therapy-refractory vasoplegia and electromechanical dissociation caused fulminant deterioration and the early death of the patient. The second case is a 76-year old male brought to the emergency room after sudden syncope, clinical sings of pericardial tamponade and suspicion of a type A acute aortic dissection. Immediate CT-angiography excluded aortic dissection and revealed massive pericardial effusion and a hypoperfused myocardial area on the territory of the first marginal branch. Immediate sternotomy under mechanical resuscitation enabled removal of the massive intrapericardial clot and revealed LVFWR. After an uncomplicated surgical repair, an uneventful postoperative course, the patient was discharged with sinus rhythm and good biventricular function. One year after the operation, he is living at home, symptom free.
Discussion: Whereas the younger patient, who was clinically stable at hospital admission received delayed surgery and did not survive treatment, the older patient, clinically unstable at presentation, went into immediate surgery and had a flawless postoperative course. Thus, early surgical repair of LVFWR leads to best outcome and treating LVFWR as a high emergency regardless of the symptoms improve survival.
Keywords: Left ventricular rupture; Myocardial infarction; Resuscitation; Surgery.
© 2024. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures

Similar articles
-
[Myocardial infarction complicating left ventricular free wall blowout rupture: a survival case after surgical repair].Kyobu Geka. 1990 Aug;43(9):738-42. Kyobu Geka. 1990. PMID: 2232395 Japanese.
-
Left ventricular free wall rupture as a result of delayed presentation of an inferior ST-elevation myocardial infarction due to fear of COVID-19: case report.J Cardiothorac Surg. 2021 Apr 22;16(1):106. doi: 10.1186/s13019-021-01495-x. J Cardiothorac Surg. 2021. PMID: 33888133 Free PMC article.
-
Surgical treatment of postinfarction left ventricular free wall rupture.J Card Surg. 2009 Nov-Dec;24(6):624-31. doi: 10.1111/j.1540-8191.2009.00896.x. J Card Surg. 2009. PMID: 20078707
-
Subacute left ventricular free-wall rupture in early course of acute myocardial infarction. Clinical report of two cases and review of the literature.G Ital Cardiol. 1999 Feb;29(2):163-70. G Ital Cardiol. 1999. PMID: 10088074 Review.
-
Meta-analysis of surgical treatment for postinfarction left ventricular free-wall rupture.J Card Surg. 2021 Sep;36(9):3326-3333. doi: 10.1111/jocs.15701. Epub 2021 Jun 1. J Card Surg. 2021. PMID: 34075615 Free PMC article. Review.
References
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

