Decision theoretical foundations of clinical practice guidelines: an extension of the ASH thrombophilia guidelines
- PMID: 38625997
- PMCID: PMC11319831
- DOI: 10.1182/bloodadvances.2024012931
Decision theoretical foundations of clinical practice guidelines: an extension of the ASH thrombophilia guidelines
Abstract
Decision analysis can play an essential role in informing practice guidelines. The American Society of Hematology (ASH) thrombophilia guidelines have made a significant step forward in demonstrating how decision modeling integrated within Grading of Recommendations Assessment, Developing, and Evaluation (GRADE) methodology can advance the field of guideline development. Although the ASH model was transparent and understandable, it does, however, suffer from certain limitations that may have generated potentially wrong recommendations. That is, the panel considered 2 models separately: after 3 to 6 months of index venous thromboembolism (VTE), the panel compared thrombophilia testing (A) vs discontinuing anticoagulants (B) and testing (A) vs recommending indefinite anticoagulation to all patients (C), instead of considering all relevant options simultaneously (A vs B vs C). Our study aimed to avoid what we refer to as the omitted choice bias by integrating 2 ASH models into a single unifying threshold decision model. We analyzed 6 ASH panel's recommendations related to the testing for thrombophilia in settings of "provoked" vs "unprovoked" VTE and low vs high bleeding risk (total 12 recommendations). Our model disagreed with the ASH guideline panels' recommendations in 4 of the 12 recommendations we considered. Considering all 3 options simultaneously, our model provided results that would have produced sounder recommendations for patient care. By revisiting the ASH guidelines methodology, we have not only improved the recommendations for thrombophilia but also provided a method that can be easily applied to other clinical problems and promises to improve the current guidelines' methodology.
© 2024 by The American Society of Hematology. Licensed under Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International (CC BY-NC-ND 4.0), permitting only noncommercial, nonderivative use with attribution. All other rights reserved.
Conflict of interest statement
Conflict-of-interest disclosure: The authors declare no competing financial interests.
Figures

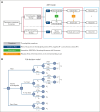
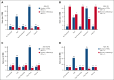
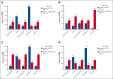

References
-
- Djulbegovic B, Hozo I, Cuker A, Guyatt G. Improving methods of clinical practice guidelines: from guidelines to pathways to fast-and-frugal trees and decision analysis to develop individualized patient care. J Eval Clin Pract. 2024;30(3):393–402. - PubMed
-
- Mercuri M, Baigrie B, Upshur REG. Going from evidence to recommendations: can GRADE get us there? J Eval Clin Pract. 2018;24(5):1232–1239. - PubMed
-
- Djulbegovic B, Hozo I. Springer Nature; 2023. Threshold Decision-making in Clinical Medicine: With Practical Application to Hematology and Oncology.
-
- Djulbegovic B, Hozo I, Lizarraga D, Guyatt G. Decomposing clinical practice guidelines panels' deliberation into decision theoretical constructs. J Eval Clin Pract. 2023;29(3):459–471. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

