Which Comprehensive Geriatric Assessment (CGA) instruments are currently used in Germany: a survey
- PMID: 38627620
- PMCID: PMC11022468
- DOI: 10.1186/s12877-024-04913-6
Which Comprehensive Geriatric Assessment (CGA) instruments are currently used in Germany: a survey
Abstract
Background: The Comprehensive Geriatric Assessment (CGA) records geriatric syndromes in a standardized manner, allowing individualized treatment tailored to the patient's needs and resources. Its use has shown a beneficial effect on the functional outcome and survival of geriatric patients. A recently published German S1 guideline for level 2 CGA provides recommendations for the use of a broad variety of different assessment instruments for each geriatric syndrome. However, the actual use of assessment instruments in routine geriatric clinical practice and its consistency with the guideline and the current state of literature has not been investigated to date.
Methods: An online survey was developed by an expert group of geriatricians and sent to all licenced geriatricians (n = 569) within Germany. The survey included the following geriatric syndromes: motor function and self-help capability, cognition, depression, pain, dysphagia and nutrition, social status and comorbidity, pressure ulcers, language and speech, delirium, and frailty. Respondents were asked to report which geriatric assessment instruments are used to assess the respective syndromes.
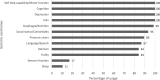
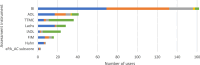
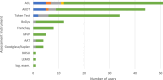
Results: A total of 122 clinicians participated in the survey (response rate: 21%); after data cleaning, 76 data sets remained for analysis. All participants regularly used assessment instruments in the following categories: motor function, self-help capability, cognition, depression, and pain. The most frequently used instruments in these categories were the Timed Up and Go (TUG), the Barthel Index (BI), the Mini Mental State Examination (MMSE), the Geriatric Depression Scale (GDS), and the Visual Analogue Scale (VAS). Limited or heterogenous assessments are used in the following categories: delirium, frailty and social status.
Conclusions: Our results show that the assessment of motor function, self-help capability, cognition, depression, pain, and dysphagia and nutrition is consistent with the recommendations of the S1 guideline for level 2 CGA. Instruments recommended for more frequent use include the Short Physical Performance Battery (SPPB), the Montreal Cognitive Assessment (MoCA), and the WHO-5 (depression). There is a particular need for standardized assessment of delirium, frailty and social status. The harmonization of assessment instruments throughout geriatric departments shall enable more effective treatment and prevention of age-related diseases and syndromes.
Keywords: Activities of daily living; CGA; Cognition; Comorbidities; Comprehensive geriatric assessment; Delirium; Depression; Dysphagia; Frailty; Self-help capability.
© 2024. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures










References
-
- Krupp S. für die AG Assessment der Deutschen Gesellschaft für Geriatrie e. V. S1-Leitlinie Geriatrisches Assessment der Stufe 2, Living Guideline, Version 11.07.2022, AWMF-Register-Nr. 084–002LG.
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Research Materials

