Is mild dehydration a risk for progression of childhood chronic kidney disease?
- PMID: 38632124
- PMCID: PMC11413076
- DOI: 10.1007/s00467-024-06332-6
Is mild dehydration a risk for progression of childhood chronic kidney disease?
Abstract
Children with chronic kidney disease (CKD) can have an inherent vulnerability to dehydration. Younger children are unable to freely access water, and CKD aetiology and stage can associate with reduced kidney concentrating capacity, which can also impact risk. This article aims to review the risk factors and consequences of mild dehydration and underhydration in CKD, with a particular focus on evidence for risk of CKD progression. We discuss that assessment of dehydration in the CKD population is more challenging than in the healthy population, thus complicating the definition of adequate hydration and clinical research in this field. We review pathophysiologic studies that suggest mild dehydration and underhydration may cause hyperfiltration injury and impact renal function, with arginine vasopressin as a key mediator. Randomised controlled trials in adults have not shown an impact of improved hydration in CKD outcomes, but more vulnerable populations with baseline low fluid intake or poor kidney concentrating capacity need to be studied. There is little published data on the frequency of dehydration, and risk of complications, acute or chronic, in children with CKD. Despite conflicting evidence and the need for more research, we propose that paediatric CKD management should routinely include an assessment of individual dehydration risk along with a treatment plan, and we provide a framework that could be used in outpatient settings.
Keywords: Children; Chronic kidney disease (CKD); Dehydration; Hypohydration; Underhydration.
© 2024. Crown.
Conflict of interest statement
The authors declare no competing interests.
Figures

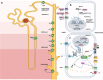
References
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

