Effect of the DASH diet on the sodium-chloride cotransporter and aquaporin-2 in urinary extracellular vesicles
- PMID: 38634133
- PMCID: PMC11386975
- DOI: 10.1152/ajprenal.00274.2023
Effect of the DASH diet on the sodium-chloride cotransporter and aquaporin-2 in urinary extracellular vesicles
Abstract
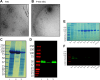
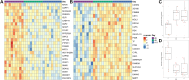
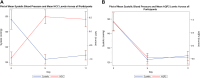
The dietary approach to stop hypertension (DASH) diet combines the antihypertensive effect of a low sodium and high potassium diet. In particular, the potassium component of the diet acts as a switch in the distal convoluted tubule to reduce sodium reabsorption, similar to a diuretic but without the side effects. Previous trials to understand the mechanism of the DASH diet were based on animal models and did not characterize changes in human ion channel protein abundance. More recently, protein cargo of urinary extracellular vesicles (uEVs) has been shown to mirror tissue content and physiological changes within the kidney. We designed an inpatient open label nutritional study transitioning hypertensive volunteers from an American style diet to DASH diet to examine physiological changes in adults with stage 1 hypertension otherwise untreated (Sacks FM, Svetkey LP, Vollmer WM, Appel LJ, Bray GA, Harsha D, Obarzanek E, Conlin PR, Miller ER 3rd, Simons-Morton DG, Karanja N, Lin PH; DASH-Sodium Collaborative Research Group. N Engl J Med 344: 3-10, 2001). Urine samples from this study were used for proteomic characterization of a large range of pure uEVs (small to large) to reveal kidney epithelium changes in response to the DASH diet. These samples were collected from nine volunteers at three time points, and mass spectrometry identified 1,800 proteins from all 27 samples. We demonstrated an increase in total SLC12A3 [sodium-chloride cotransporter (NCC)] abundance and a decrease in aquaporin-2 (AQP2) in uEVs with this mass spectrometry analysis, immunoblotting revealed a significant increase in the proportion of activated (phosphorylated) NCC to total NCC and a decrease in AQP2 from day 5 to day 11. This data demonstrates that the human kidney's response to nutritional interventions may be captured noninvasively by uEV protein abundance changes. Future studies need to confirm these findings in a larger cohort and focus on which factor drove the changes in NCC and AQP2, to which degree NCC and AQP2 contributed to the antihypertensive effect and address if some uEVs function also as a waste pathway for functionally inactive proteins rather than mirroring protein changes.NEW & NOTEWORTHY Numerous studies link DASH diet to lower blood pressure, but its mechanism is unclear. Urinary extracellular vesicles (uEVs) offer noninvasive insights, potentially replacing tissue sampling. Transitioning to DASH diet alters kidney transporters in our stage 1 hypertension cohort: AQP2 decreases, NCC increases in uEVs. This aligns with increased urine volume, reduced sodium reabsorption, and blood pressure decline. Our data highlight uEV protein changes as diet markers, suggesting some uEVs may function as waste pathways. We analyzed larger EVs alongside small EVs, and NCC in immunoblots across its molecular weight range.
Keywords: AQP2; DASH diet; NCC; extracellular vesicles; proteomic analysis.
Conflict of interest statement
J.N.T.: NIH-NCI: Payments or Remuneration, Bio-Ascend LLC/Regional Cancer Care Associates: Payments or Remuneration, Reimbursed or Sponsored, Travel, AstraZeneca: Board of Directors Compensation, Payments or Remuneration, Reimbursed or Sponsored Travel. Clinical Directors Network, Inc.: Board of Directors Compensation, Payments or Remuneration, Reimbursed or Sponsored Travel. None of the other authors has any conflicts of interest, financial or otherwise, to disclose.
Figures


References
-
- Blumenthal JA, Hinderliter AL, Smith PJ, Mabe S, Watkins LL, Craighead L, Ingle K, Tyson C, Lin PH, Kraus WE, Liao L, Sherwood A. Effects of lifestyle modification on patients with resistant hypertension: results of the TRIUMPH randomized clinical trial. Circulation 144: 1212–1226, 2021. doi:10.1161/CIRCULATIONAHA.121.055329. - DOI - PMC - PubMed
-
- Sacks FM, Svetkey LP, Vollmer WM, Appel LJ, Bray GA, Harsha D, Obarzanek E, Conlin PR, Miller ER 3rd, Simons-Morton DG, Karanja N, Lin PH; DASH-Sodium Collaborative Research Group. Effects on blood pressure of reduced dietary sodium and the Dietary Approaches to Stop Hypertension (DASH) diet. DASH-Sodium Collaborative Research Group. N Engl J Med 344: 3–10, 2001. doi:10.1056/NEJM200101043440101. - DOI - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Research Materials

