Shifts in Diagnostic Testing for Headache in the Emergency Department, 2015 to 2021
- PMID: 38639937
- PMCID: PMC11031686
- DOI: 10.1001/jamanetworkopen.2024.7373
Shifts in Diagnostic Testing for Headache in the Emergency Department, 2015 to 2021
Abstract
Importance: Subarachnoid hemorrhage is typically diagnosed by noncontrast head computed tomography (CT); lumbar puncture is recommended if computed tomography is nondiagnostic, although CT cerebral angiography has been promoted as an alternative to lumbar puncture in this diagnostic pathway. The outcomes of this debate in practice have not been studied.
Objective: To determine whether CT cerebral angiography use has increased in lieu of lumbar puncture among emergency department (ED) patients with headache, with an increase in unruptured intracranial aneurysm detection.
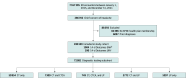
Design, setting, and participants: This retrospective cohort study took place in 21 community EDs of an integrated health care system in Northern California between 2015 and 2021. Participants were adult (aged >17 years) health plan members with a chief concern of headache. Exclusions were prior diagnoses of subarachnoid hemorrhage, unruptured intracranial aneurysm, cerebral arteriovenous malformation, or cerebrospinal fluid shunt. Data were analyzed from October to November 2023.
Exposures: CT cerebral angiography and/or lumbar puncture during the ED encounter.
Main outcomes and measures: Primary and secondary outcomes were 14-day and 90-day unruptured intracranial aneurysm detection, respectively. Safety outcomes were missed diagnoses of subarachnoid hemorrhage or bacterial meningitis. The annual incidence of unruptured intracranial aneurysm detection was normalized to the incidence of subarachnoid hemorrhage (UIA:SAH ratio). Average annualized percentage changes were quantified using joinpoint regression analysis.
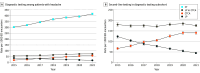
Results: Among 198 109 included ED encounters, the mean (SD) age was 47.5 (18.4) years; 140 001 patients (70.7%) were female; 29 035 (14.7%) were Black or African American, 59 896 (30.2%) were Hispanic or Latino, and 75 602 (38.2%) were White. Per year, CT cerebral angiography use increased (18.8%; 95% CI, 17.7% to 20.3%) and lumbar punctures decreased (-11.1%; 95% CI, -12.0% to -10.4%), with a corresponding increase in the 14-day UIA:SAH ratio (3.5%; 95% CI, 0.9% to 7.4%). Overall, computed tomography cerebral angiography use increased 6-fold relative to lumbar puncture, with a 33% increase in the detection of UIA. Results were similar at 90 days and robust to sensitivity analyses. Subarachnoid hemorrhage (1004 cases) and bacterial meningitis (118 cases) were misdiagnosed in 5% and 18% of cases, respectively, with no annual trends (P = .34; z1003 = .95 and P = .74; z117 = -.34, respectively).
Conclusions and relevance: In this cohort study of ED patients with headache, increases in CT cerebral angiography use were associated with fewer lumbar punctures and higher detection of unruptured intracranial aneurysms, with no significant change in missed diagnoses of subarachnoid hemorrhage or bacterial meningitis. While this shift in diagnostic strategy appeared safe in the short-term, the long-term consequences remain unclear.
Conflict of interest statement
Figures
Comment in
-
Beyond the AJR: Intracranial CTA Versus Lumbar Puncture for Suspected Subarachnoid Hemorrhage With Negative Head CT.AJR Am J Roentgenol. 2025 Mar;224(3):e2431743. doi: 10.2214/AJR.24.31743. Epub 2024 Jul 17. AJR Am J Roentgenol. 2025. PMID: 39016456 No abstract available.
Similar articles
-
Low risk for subsequent subarachnoid hemorrhage for emergency department patients with headache, bloody cerebrospinal fluid, and negative findings on cerebrovascular imaging.J Neurosurg. 2014 Jul;121(1):24-31. doi: 10.3171/2014.3.JNS132239. Epub 2014 Apr 18. J Neurosurg. 2014. PMID: 24745707
-
Can computed tomography angiography of the brain replace lumbar puncture in the evaluation of acute-onset headache after a negative noncontrast cranial computed tomography scan?Acad Emerg Med. 2010 Apr;17(4):444-51. doi: 10.1111/j.1553-2712.2010.00694.x. Acad Emerg Med. 2010. PMID: 20370785 Review.
-
Sensitivity of noncontrast cranial computed tomography for the emergency department diagnosis of subarachnoid hemorrhage.Ann Emerg Med. 2008 Jun;51(6):697-703. doi: 10.1016/j.annemergmed.2007.10.007. Epub 2008 Jan 22. Ann Emerg Med. 2008. PMID: 18207607
-
Prospective Implementation of the Ottawa Subarachnoid Hemorrhage Rule and 6-Hour Computed Tomography Rule.Stroke. 2020 Feb;51(2):424-430. doi: 10.1161/STROKEAHA.119.026969. Epub 2019 Dec 6. Stroke. 2020. PMID: 31805846
-
Comprehensive review of imaging of intracranial aneurysms and angiographically negative subarachnoid hemorrhage.Neurosurg Focus. 2019 Dec 1;47(6):E20. doi: 10.3171/2019.9.FOCUS19653. Neurosurg Focus. 2019. PMID: 31786554 Review.
Cited by
-
NeuroMix with MRA: A Fast MR Protocol to Reduce Head and Neck CTA for Patients with Acute Neurologic Presentations.AJNR Am J Neuroradiol. 2024 Nov 7;45(11):1730-1736. doi: 10.3174/ajnr.A8386. AJNR Am J Neuroradiol. 2024. PMID: 38906674
-
Potential Diagnostic Error for Emergency Conditions, Mortality, and Healthy Days at Home.JAMA Netw Open. 2025 Jun 2;8(6):e2516400. doi: 10.1001/jamanetworkopen.2025.16400. JAMA Netw Open. 2025. PMID: 40526380 Free PMC article.
References
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

