Case Series of Endoscopic Papillary Balloon Dilation for Children with Common Bile Duct Stones and a Review of the Literature
- PMID: 38673524
- PMCID: PMC11050672
- DOI: 10.3390/jcm13082251
Case Series of Endoscopic Papillary Balloon Dilation for Children with Common Bile Duct Stones and a Review of the Literature
Abstract
Background: Endoscopic sphincterotomy (EST) has been employed for the endoscopic treatment of common bile duct stones (CBDSs) and has been reported to have a high success rate for stone removal. However, EST is associated with a risk of bleeding, perforation, and sphincter of Oddi function disruption. To avoid these risks, endoscopic papillary balloon dilation (EPBD) is an option for CBDS. Sphincter of Oddi function preservation decreases long-term biliary infection and gallstone recurrence. EPBD may have advantages in children who require a long follow up. However, there have been few reports on pediatric cases, particularly in infants. Methods: From September 2017 to December 2023, we performed EPBD for four pediatric CBDSs. The patients were aged from 5 months to 8 years, including two infants aged 5 and 6 months. Furthermore, we reviewed the stone removal rate and complications of 545 ESTs performed at high-volume centers and 13 EPBD-reported cases in children with CBDSs. Results: CBDSs of all patients who underwent EPBD in our institution were successfully removed. No bleeding or perforation was noted; pancreatitis was observed in three patients. In an analysis of 545 ESTs in children, the stone removal rate was high, ranging from 83% to 100% (mean 96%). The incidence of pancreatitis was 0-9.6% (mean 4.4%), and the grade of pancreatitis was almost mild. The bleeding frequency was 1.3-5.4% (mean 2.7%). With regards to the grade of bleeding, seven cases were mild (64%) and four were moderate (36%). Compared with adults who underwent EST, the frequencies of pancreatitis and bleeding were almost equal in children; however, in children, once bleeding occurs, it has a higher risk of leading to blood transfusion. Stone removal via EPBD in children has a 100% success rate. Pancreatitis was responsible for all complications were related; its frequency was 46% (6/13 patients, including five mild cases and one moderate case), which is higher than that of EST and adult cases who underwent EPBD. In most children with pancreatitis, pancreatic enzyme levels returned to normal within 2-3 days following EPBD, and no severe cases caused by EPBD were reported. Conclusions: CBDS removal via EPBD in children has a high success rate with very low risk of bleeding and perforation. Although pancreatitis frequently occurs, most cases are mild. Sphincter of Oddi function preservation via EPBD is expected to prevent long-term stone recurrence and biliary tract infection, and EPBD is considered to be an effective method for CBDS removal in children.
Keywords: children; choledocholithiasis; common bile duct stone; endoscopic papillary balloon dilation; endoscopic retrograde cholangiopancreatography; endoscopic sphincterotomy.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
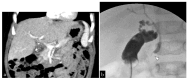
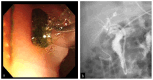
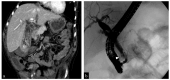
Similar articles
-
Minimal endoscopic sphincterotomy with papillary balloon dilation versus endoscopic sphincterotomy for the treatment of common bile duct stones (MARBLE Trial): study protocol for a multicenter randomized controlled trial.Trials. 2025 Aug 26;26(1):307. doi: 10.1186/s13063-025-09076-2. Trials. 2025. PMID: 40859328 Free PMC article.
-
Endoscopic Papillary Balloon Dilation Versus Small Endoscopic Sphincterotomy for Endoscopic Retrograde Cholangiopancreatography-Related Adverse Events in Patients With Non-Dilated Distal Bile Duct.Surg Laparosc Endosc Percutan Tech. 2025 Apr 1;35(2):e1200. doi: 10.1097/SLE.0000000000001200. Surg Laparosc Endosc Percutan Tech. 2025. PMID: 39895510
-
Effect of endoscopic sphincterotomy and endoscopic papillary balloon dilation endoscopic retrograde cholangiopancreatographies on the sphincter of Oddi.World J Gastrointest Surg. 2024 Jun 27;16(6):1726-1733. doi: 10.4240/wjgs.v16.i6.1726. World J Gastrointest Surg. 2024. PMID: 38983341 Free PMC article.
-
Endoscopic Papillary Large Balloon Dilation Versus Endoscopic Sphincterotomy for Treatment of Bile Duct Stones.Curr Treat Options Gastroenterol. 2019 Jun;17(2):221-230. doi: 10.1007/s11938-019-00234-5. Curr Treat Options Gastroenterol. 2019. PMID: 30945095 Review.
-
Endoscopic treatment of difficult extrahepatic bile duct stones, EPBD or EST: An anatomic view.World J Gastrointest Endosc. 2015 Mar 16;7(3):274-7. doi: 10.4253/wjge.v7.i3.274. World J Gastrointest Endosc. 2015. PMID: 25789099 Free PMC article. Review.
Cited by
-
Pancreaticobiliary Reflux with Normal and Relatively Long Common Channels Causing Cholelithiasis and Acute Pancreatitis in Children.J Clin Med. 2024 Dec 16;13(24):7650. doi: 10.3390/jcm13247650. J Clin Med. 2024. PMID: 39768573 Free PMC article.
-
Analysis of risk factors for bile leakage after laparoscopic exploration and primary suture of common bile duct.World J Gastrointest Surg. 2025 Mar 27;17(3):102190. doi: 10.4240/wjgs.v17.i3.102190. World J Gastrointest Surg. 2025. PMID: 40162406 Free PMC article.
References
-
- Palasciano G., Portincasa P., Vinciguerra V., Velardi A., Tardi S., Baldassarre G., Albano O. Gallstone prevalence and gallbladder volume in children and adolescents: An epidemiological ultrasonographic survey and relationship to body mass index. Am. J. Gastroenterol. 1989;84:1378–1382. - PubMed
-
- Wesdorp I., Bosman D., de Graaff A., Aronson D., van der Blij F., Taminiau J. Clinical presentations and predisposing factors of cholelithiasis and sludge in children. J. Pediatr. Gastroenterol. Nutr. 2000;31:411–417. - PubMed
LinkOut - more resources
Full Text Sources
Research Materials

