Pain management in chronic pancreatitis
- PMID: 38680261
- PMCID: PMC11045512
- DOI: 10.12998/wjcc.v12.i12.2016
Pain management in chronic pancreatitis
Abstract
Pain in chronic pancreatitis (CP) is difficult to manage. Many patients suffer from inadequate pain relief, completely incapacitating them in their daily activities. Historically, despite their well-known adverse effects, opioids have been the pillar of treatment regimens in painful CP. The management is now gradually evolving with a better understanding of the underlying pathophysiology of CP-related pain. Clinicians should follow a holistic approach to the management of CP-associated pain, which must involve lifestyle changes that are coupled with analgesic medications and other pain-relieving interventions. Furthermore, there is no easy cure for vanquishing CP-associated pain. Each patient must be evaluated on a case-by-case basis by a multidisciplinary team to decide which treatment option is best suited for that individual.
Keywords: Abdominal pain; Analgesics; Life style; Palliative care; Pancreatitis; Psychology.
©The Author(s) 2024. Published by Baishideng Publishing Group Inc. All rights reserved.
Conflict of interest statement
Conflict-of-interest statement: The authors declare no conflict of interest.
Figures
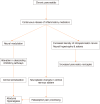
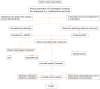
References
-
- Braganza JM, Lee SH, McCloy RF, McMahon MJ. Chronic pancreatitis. Lancet. 2011;377:1184–1197. - PubMed
-
- Dimcevski G, Sami SA, Funch-Jensen P, Le Pera D, Valeriani M, Arendt-Nielsen L, Drewes AM. Pain in chronic pancreatitis: the role of reorganization in the central nervous system. Gastroenterology. 2007;132:1546–1556. - PubMed
-
- Ceyhan GO, Michalski CW, Demir IE, Müller MW, Friess H. Pancreatic pain. Best Pract Res Clin Gastroenterol. 2008;22:31–44. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Miscellaneous

