Post-COVID-19 respiratory sequelae two years after hospitalization: an ambidirectional study
- PMID: 38680501
- PMCID: PMC11047789
- DOI: 10.1016/j.lana.2024.100733
Post-COVID-19 respiratory sequelae two years after hospitalization: an ambidirectional study
Abstract
Background: COVID-19 lung sequelae can impact the course of patient lives. We investigated the evolution of pulmonary abnormalities in post-COVID-19 patients 18-24 months after hospital discharge.
Methods: A cohort of COVID-19 patients admitted to the Hospital das Clínicas da Faculdade de Medicina da USP in São Paulo, Brazil, between March and August of 2020, were followed-up 6-12 months after hospital discharge. A subset of patients with pulmonary involvement and chest computed tomography (CT) scans were eligible to participate in this second follow-up (18-24 months). Data was analyzed in an ambidirectional manner, including retrospective data from the hospitalization, and from the first follow-up (6-12 months after discharge), and compared with the prospective data collected in this new follow-up.
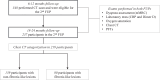
Findings: From 348 patients eligible, 237 (68%) participated in this follow-up. Among participants, 139 (58%) patients presented ground-glass opacities and reticulations, and 80 (33%) presented fibrotic-like lesions (traction bronchiectasis and architectural distortion). Five (2%) patients improved compared to the 6-12-month assessment, but 20 (25%) of 80 presented worsening of lung abnormalities. For those with relevant assessments on both occasions, comparing the CT findings between this follow-up with the previous assessment, there was an increase in patients with architectural distortion (43 [21%] of 204 vs 57 [28%] of 204, p = 0.0093), as well as in traction bronchiectasis (55 [27%] of 204 vs 69 [34%] of 204, p = 0.0043). Patients presented a persistent functional impairment with demonstrated restrictive pattern in both follow-ups (87 [42%] of 207 vs 91 [44%] of 207, p = 0.76), as well as for the reduced diffusion capacity (88 [42%] of 208 vs 87 [42%] of 208, p = 1.0). Length of hospitalization (OR 1.04 [1.01-1.07], p = 0.0040), invasive mechanical ventilation (OR 3.11 [1.3-7.5] p = 0.011), patient's age (OR 1.03 [1.01-1.06] p = 0.0074 were consistent predictors for development of fibrotic-like lung lesions in post-COVID-19 patients.
Interpretation: Post-COVID-19 lung sequelae can persist and progress after hospital discharge, suggesting airways involvement and formation of new fibrotic-like lesions, mainly in patients who were in intensive care unit (ICU).
Funding: São Paulo Research Foundation (22/01769-5) and Instituto Todos pela Saúde (C1721).
Keywords: Ambidirectional cohort; COVID-19; Fibrosis; Lung CT; PASC; Pulmonary function; Small airways disease.
© 2024 The Authors.
Conflict of interest statement
We declare no competing interests.
Figures

References
LinkOut - more resources
Full Text Sources

